In history, COVID-19 was perhaps one of the most serious issues confronting the United States healthcare system, but it was only one of several. That's right; there has been a slew of concerns plaguing healthcare for years, resulting in patient safety mishaps, income losses, and more. However, due to the consequences of COVID-19, these losses skyrocketed, with estimates of $323 billion in 2020. While the pandemic is gradually fading, things are improving as providers open their doors to in-person appointments.
While hospitals, relatively small practices, and significantly bigger healthcare systems are known for saving lives and treating patients, every public health care organization must develop successful financial processes and policies. That's where revenue cycle management in healthcare comes in.
Healthcare revenue cycle management is the financial operation that establishments use to manage the administrative and clinical elements associated with claims processing, payment, and revenue generation. The procedure entails identifying, managing, and collecting revenue from patient services.
Americans are currently confronted with an irony that may apply to healthcare revenue cycle management solutions in 2021. Even in a decent year, norms and standards change quickly, but the pandemic decided to throw healthcare RCM into a whirlwind. It's critical to keep up with these developments, or you'll fall behind. Following COVID, new legislation and shifts to work from home will significantly impact healthcare RCM procedures and cybersecurity requirements. These trends will have an impact on your workflow in the coming year, as shown below.
At the onset of the pandemic, health system and hospital revenue cycle teams were confronted with many challenges, many of which are still impacting today. The closure and the transition to largely virtual treatment created substantial disruption and problems that revenue cycle staff had never encountered before. Simultaneously, revenue cycle workforces went from almost 100% remote to nearly 100% remote; medical coding software process and claims procedures are turned upside down in the face of payer and government reforms, and budgets were slashed as elective surgeries came to a standstill due to the COVID-19 problem.
Impact of Automation on the Healthcare Revenue Cycle Management:
After the COVID- 19 pandemic, new legislation and shifts to work from home will significantly impact healthcare RCM procedures and cybersecurity requirements. Here's how these tendencies are manifesting themselves to support Revenue Cycle Management in Healthcare Industry:
Increase in Remote Work:
Medical Billing and accounting teams in healthcare are close to the front lines. The billing and accounts teams were quickly forced to switch to remote work, although the work never stopped. The resulting increase in security and compliance controls isn't expected to go away anytime soon.
Around 75% of large hospitals and health systems have traditional instructional staffing changes that include work from home. As a result, your RCM procedures must be able to function just as well at home as they do in the hospital.
Increase of Patient as Payer:
With insurance companies' increased denials following COVID, individual patients will be forced to shoulder responsibility for their procedures. Healthcare organizations have struggled to collect payments on time due to
the change, as they are only experienced with the behavior of significant payers, not individual consumers. This step slows down the entire RCM process, and it's starting to become a real revenue issue for about two-thirds of healthcare firms.
Since these Patients have quite different payment cycles than typical payers, it will be critical to pay attention to the data to discover new best practices for engaging the customer and ensuring that the payment is made.
Increase in Consumer Collection Laws:
Surprising billing methods will be restricted by this regulation, which will demand greater attention on compliance. Because billing cycles and standards change, it's critical to keep the RCM practice up to date so that one won't miss out on any compensation due to a clerical error.
Increase in Cyber Security Issues:
Security breaches in the healthcare industry are rising, and sensitive patient information is always a target. The cost of a security rupture is higher than the cost of protection. These standards may appear to be working right now, but it's all too easy to become complacent. As a result, it is necessary to ensure that RCM practices are compliant with industry-standard cybersecurity protocols.
Increase in RCM Automation:
The healthcare revenue management team and the transaction data team will save time due to automation, which will result in more timely compilations from payers and patients. These automation systems will need to be intelligent and scalable to handle multiple care approaches, such as telehealth, to maintain pace with the enormously complex public insurance rules. Conventionally, rules-based technologies have driven automation in patient billing. However, as medical reimbursement becomes more complicated, a shift to intelligent automation powered by machine learning can help maintain productivity.
Furthermore, while healthcare revenue cycle management solutions are complicated due to the numerous technical processes, it is simple to comprehend.
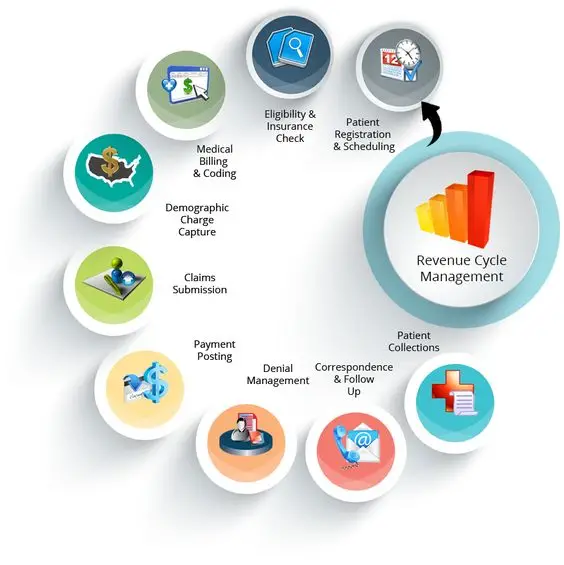
In a word, revenue cycle management healthcare is used by hospitals and health systems to track the “revenue” they earn from treating patients. RCM has several processes, but it begins with the initial encounter with the patient, such as booking an appointment, and continues until caregivers receive the final payment.
The revenue cycle of a healthcare facility typically has seven components:
-
Preregistration:
The primary and most crucial step in the revenue cycle process is preregistration. Pre Registration allows the medical practice to capture demographic information, insurance information, and eligibility in real-time through a clearinghouse. The data is sent to the patient's protection company and then passed through the provider's practice management system, informing the provider of coverage, deductible, co-insurance, and copayment.
The preregistration method allows a practice to establish the financial tone from the start and eliminates payment-related questions. Many categories are usually missed if a practice does not have a strict pre registration procedure.
-
Registration:
From start to finish, registrations ensure that the patient's health information is 100 % accurate. Upon registration, the provider verifies the patient's address, phone number, date of birth, guarantors, and insurance