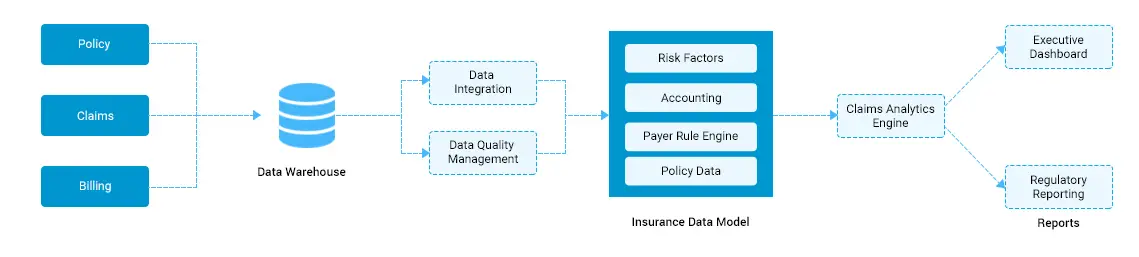
Insurance claim data help insurers find the most relevant and accurate information about customer claims. These insurance analytics solutions can be used for many purposes, such as helping insurers identify fraudulent or exaggerated claims, enabling them to verify the accuracy of claims, and guiding adjusters through the claim process. Health Insurance claim analytics solutions consist of various tools that are designed to help with many different aspects of an insurer’s business. These tools can provide insights into trends in claims, customer behavior, and more.
What is Insurance Data?
It can be difficult to summarize the importance of data in the insurance industry. It is so big, and the industry is so dynamic, that there is a lot of data available, but there is also no single way to look at it. With so many tools at an insurer’s disposal, it’s important to understand what information is important and what data should not be used for. Insurance data is not like data from another industry; it’s constantly changing, and it’s important that a data provider makes it as easy as possible for insurers to integrate the data with their systems. Any report a company has that’s based on financial data must be factored into the fact that insurance claims data must be of high quality. If the data comes from any other industry, it is not guaranteed to be as accurate and complete.
Why is Insurance Data Important?
While there are different ways to evaluate claims, the most important factor that determines the true worth of insurance data is how accurate the data is. Insurance data systems are designed to extract certain pieces of information about the nature and severity of claims. These data systems contain different types of information, including: Claim specific data, which details specific information about the nature of a claim and the nature of an alleged injury. Claim general data, which details general data about the data claim. Claim adjusting information, which details information about how claims are being processed and how they are being corrected. Claim payouts information, which details information about how claims are being paid and why they are paid. And more.
Types of Data in the Insurance Industry
The nature of the insurance industry is such that there are many types of data that are important for insurance companies to collect. One important type of data is claims data. This can be information about a customer’s actual claims, as well as any premium credits or discounts that are applied to these claims. Health insurance analytics can be useful for both individual and business clients, depending on the customer. For example, the claim data can help predict the likelihood of a particular customer’s premium payment falling below a certain level or being denied for a claim. Customers are often keen to know how much their premiums are increasing or decreasing.
The Importance of Analytics in Health Insurance
Various types of analytics solutions are used for analyzing medical claims data. These include: Customer Journey Analytics This method is based on observing a customer as they enter their health plan and over time, observing their activity in their health plan and subsequent healthcare services that they take part in. The aim of this analytics method is to identify the points when a customer is most at risk of fraud. The analytics tool can then take this information and identify areas in which customer behavior may be inconsistent or less than transparent. Insurers can then use this information to improve their customer service processes and improve their customer experience.
Conclusion
Health Insurance claim analytics solutions are extremely important for many Americans. These days, the competition for customers is fierce. With that in mind, an insurance provider’s claim analytics tool can be a tool that can help to reduce losses to fraud, lower costs, and improve efficiency. With the right analytics tool, a business can better understand its customers and determine which health insurance products are a good fit for its business.