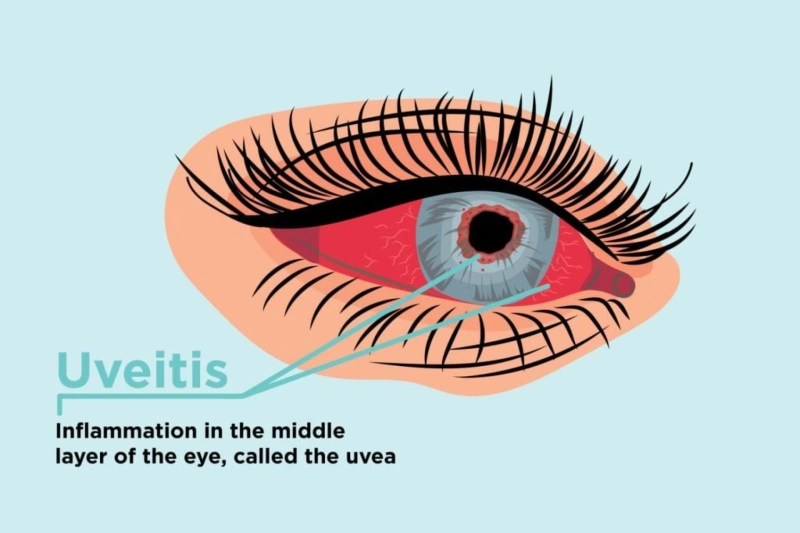
Uveitis is a general term for inflammation of the uvea, the middle layer of the eye, which consists of the iris, ciliary body, and choroid. It is a potentially serious eye condition that can lead to vision loss if not treated promptly and effectively. It can occur at any age, although it is most commonly diagnosed in people between the ages of 20 and 60.
Types of Uveitis
Uveitis is classified based on the part of the uvea affected:
Anterior Uveitis: Inflammation of the iris (iritis) or the iris and ciliary body (iridocyclitis). This is the most common type.
Intermediate Uveitis: Involves the ciliary body and the vitreous (gel-like substance in the eye).
Posterior Uveitis: Affects the choroid and may also involve the retina.
Panuveitis: Inflammation that affects all parts of the uvea.
Causes of Uveitis
Uveitis can result from a wide range of underlying causes. In many cases, the exact cause remains unknown. However, common causes include:
- Autoimmune Disorders: Conditions like rheumatoid arthritis, spondylitis, lupus can trigger uveitis as the immune system attacks the body’s own tissues, including the eye.
- Infections: Bacterial, viral, fungal, or parasitic infections can lead to uveitis.
- Eye Injury or Surgery: Trauma to the eye or complications from surgery may result in inflammation.
- Systemic Inflammatory Conditions: Like inflammatory bowel disease or multiple sclerosis.
- Genetic Factors: Some individuals have a genetic predisposition to uveitis.
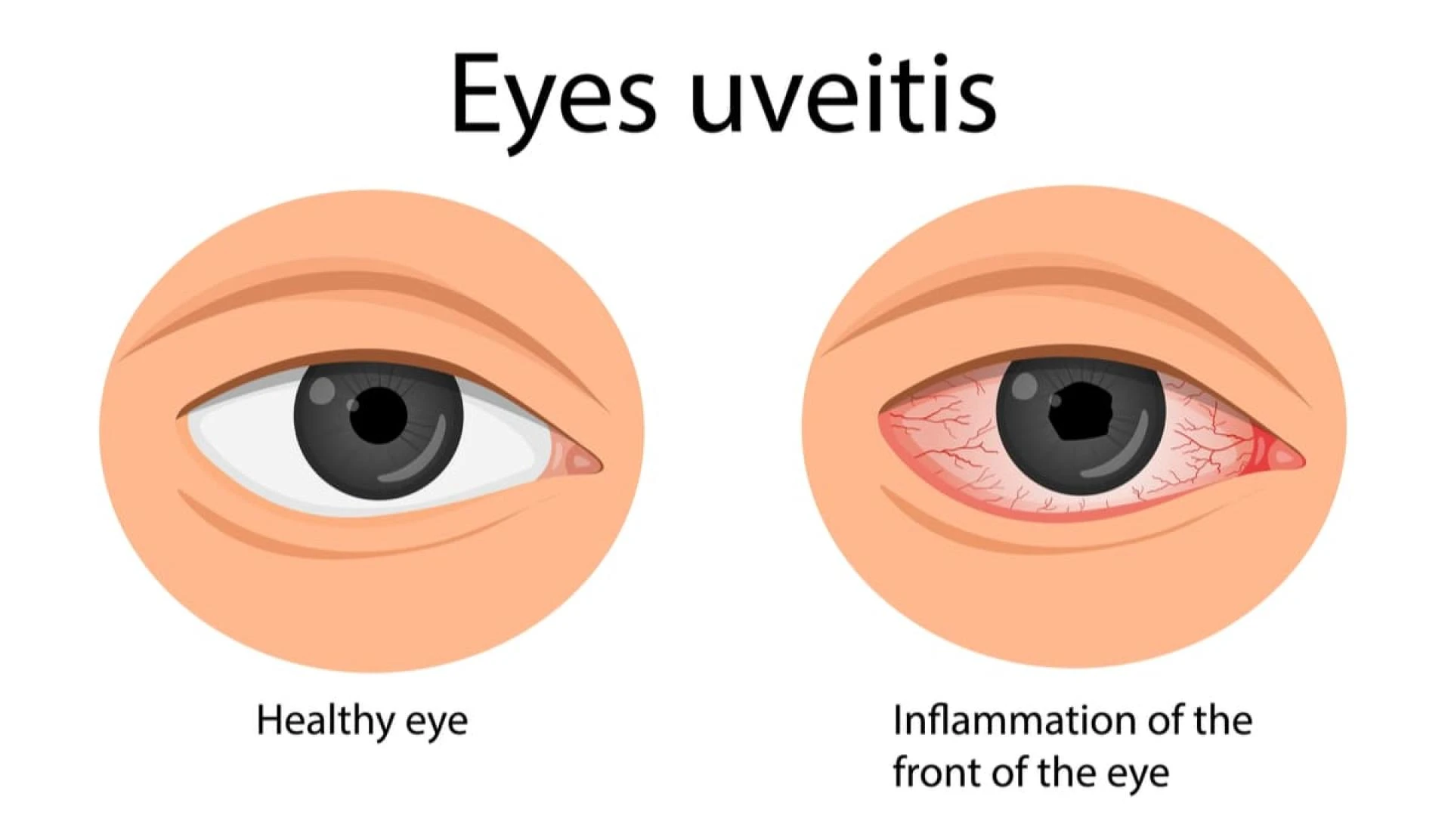
Symptoms of Uveitis
The symptoms can develop suddenly or gradually, depending on the type and cause. Common symptoms include:
- Eye redness
- Eye pain
- Blurred or decreased vision
- Light sensitivity (photophobia)
- Floaters (dark spots in vision)
The symptoms can range from mild to severe, and if untreated, they can lead to complications such as glaucoma, cataracts, retinal detachment, or even blindness.
Diagnosis
Diagnosing uveitis requires a thorough eye examination by an ophthalmologist. Key diagnostic procedures include:
- Slit-lamp examination
- Fundoscopy
- Ocular coherence tomography (OCT)
- Fluorescein angiography
Treatment Options
The primary goal in treating Uveitis is to reduce inflammation, relieve pain, and prevent vision loss. Treatment depends on the type, cause, and severity of the condition.
Corticosteroids: The mainstay of treatment, given as eye drops, oral tablets, or injections to reduce inflammation.
Immunosuppressive drugs: For patients who do not respond to steroids or have chronic uveitis.
Antibiotics or antivirals: If the cause is infectious.
Mydriatic eye drops: To dilate the pupil and prevent painful spasms in the iris.
Surgery: In rare cases, surgical procedures like vitrectomy may be required.
Complications of Uveitis
If not treated properly, uveitis can lead to serious complications, including:
- Glaucoma
- Cataracts
- Retinal detachment
- Macular edema
- Permanent vision loss
Regular follow-ups and monitoring are critical to managing these risks.
Conclusion
Uveitis is a potentially serious condition that can affect people of all ages. Early recognition, proper diagnosis, and timely treatment are crucial for preventing complications and preserving vision. If you experience persistent eye redness, pain, or vision changes, consult an eye care professional promptly. For those living with autoimmune diseases or infections known to cause uveitis, regular eye exams are essential. With modern treatments and interdisciplinary care at RENUKA EYE INSTITUTE, most people with uveitis can maintain good vision and lead normal lives.