

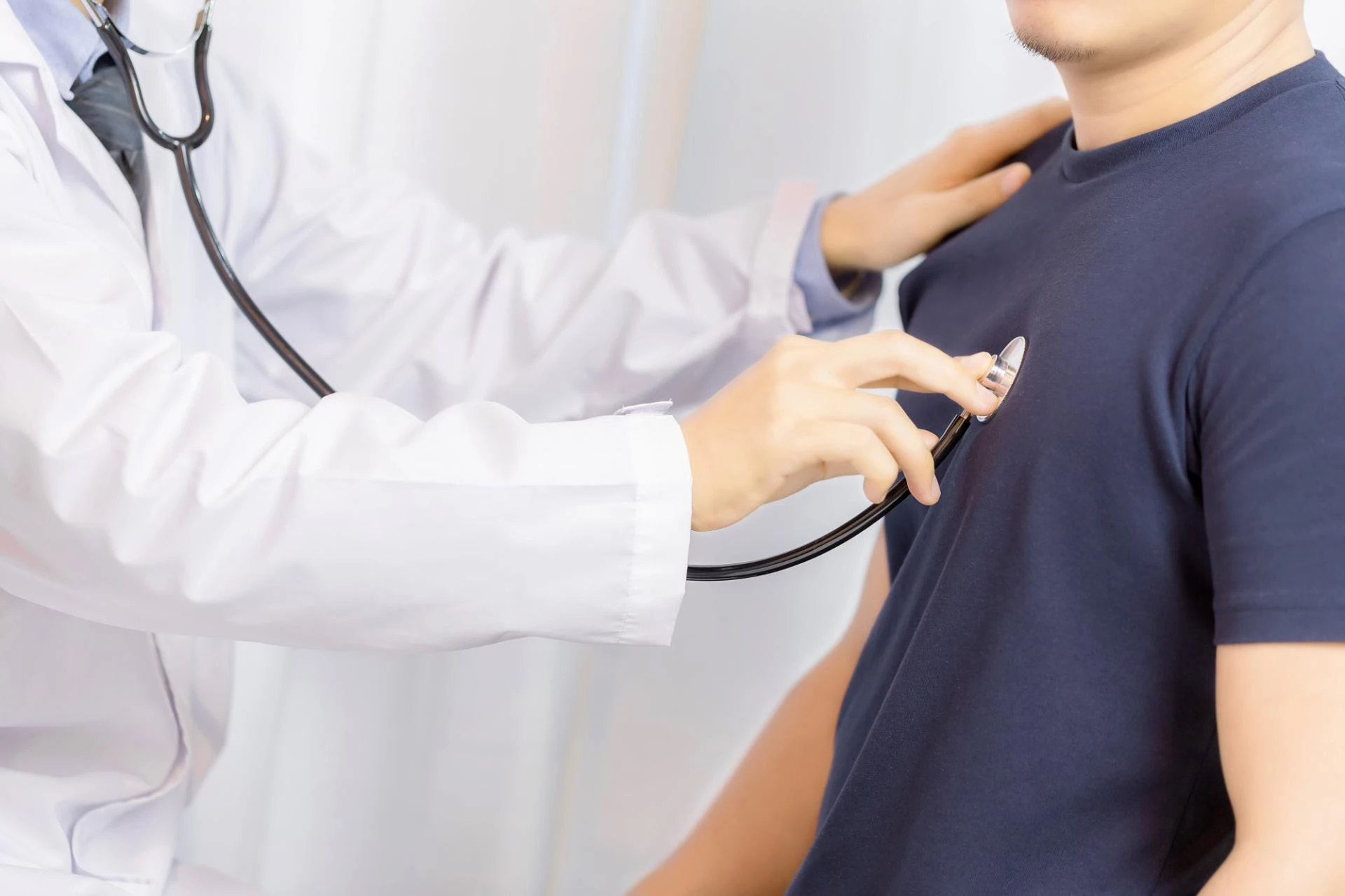

Billing operations in modern healthcare have become a strategic revenue function. This evolution from a back-office procedure to centralized revenue protecti...

Complex drug reimbursement is not a cakewalk. The biggest point of the said complexity is that it involves a lot of parties which include patients, pharmacies, providers, payers, and manufacturers, each with their own set of rules.

There are basically two steps in the billing process, which include pre-billing and post-delivery billing. There are four steps in the pre-billing process which include order intake, physician communication, documentation follow-up, and order processing. The post delivery process includes billing process, claim submission, and resubmission.

There are several reasons as to why CPT codes are denied in billing for gastroenterology services. Firstly, being unable to identify and assign the correct codes for services can lead to upcoding and under coding, leading to billing inaccuracy. Similarly, unable to use modifiers properly will not allow the insurance company to understand additional clinical context.

Infusion services are an essential component of modern healthcare treatment that involves managing medications by using specialized equipment and protocols. However, the task of billing for these services can be complex, especially for CPT codes like 96413. This code is used for initial IV chemotherapy infusion or the use of other drugs for at least a period of 16-90 minutes or the initial first house. Billing these infusion services without the proper coding knowledge could lead to possible errors in documentation or claim submissions, which affects the reimbursement process.

Currently, many healthcare providers are facing difficulties in managing in-house medical billing, required for reimbursing insurance claims. This is happening mainly because the insurance policies and coding systems keep on evolving, which could be overwhelming for in-house billers. The billing process is also affected because of delays in claim reimbursement.

Infusion billing services go through multiple stages to complete the reimbursement for the providers. These stages include registration of patient details, authorization and validation, coding, claims submission, and accounts receivable.
We know that managing cardiology billing can be extremely daunting and challenging affair. While there are many procedure that because tension but transthoracic Echocardiography (93306) remains one of the most frequently denied claims in 2026. It is mainly because the documentation doesn't meet the full study requirements. As for a 93306, you must document the M-mode, 2D imaging, Doppler and even the color flow.

It is no secret that infusion therapy has evolved into one of the most clinically significant and administratively taxing sectors of medicine. As with the specialty drugs for oncology, rheumatology, and neurology becoming more advanced, the financial stakes for practices providing these life-saving treatments have never been higher.

Weak medical billing can cause high denial rates, delayed payments, underpaid claims, aging accounts receivable, staff burnout, and compliance risks. Small mistakes—like a missed modifier, an outdated payer rule, or a denied claim that isn’t appealed—add up quickly and can cost a practice thousands or even millions of dollars over time. The worst part is that most of these losses don’t show clearly on reports, quietly hurting your revenue.

Health system billing refers to the end-to-end process which includes documenting patient services, creating coded entries based on standards, processing patients' claims payments, making payments, and processing patient statements for outstanding payments.
Cardiology is one of the major specialties which focuses on treating and diagnosing heart conditions. Echocardiography requires clear documentation of study type, whether Doppler or color flow mapping was utilized, and clinical necessity supporting the procedure. Moreover, cardiology adds complexity with the use of radiopharmaceuticals and technical versus professional components.

Infusion billing plays an essential role in streamlining the claim submission process. You need to create an accurate billing process to make sure no issue occurs. Your staff needs to know all the complex ICD, CPT, and HCPCS codes along with the right modifiers to streamline the process.

Health system billing is the process of collecting payment for medical services. It involves charges, codes, insurance claims, and patient statements.

Urgent care centers are one of the vital domains in the healthcare unite that experience a rapid growth. However, every successful story begins with a constructive objective and for yours, its patient care. While doctors focus on treating patients quickly, billing teams face a tough job. They must deal with confusing codes, insurance rules, and denied claims. Let’s be honest: urgent care billing is more than just sending claims.

The process of health system billing is a bit complex, which sets it apart from other types of billing. However, there are several must-known facts about this billing process which are divided into two parts such as hospital billing and professional billing. Hospital billing is the process to bill the inpatient and outpatient services, skilled nursing services, laboratory services, medical equipment and supplies.

The specialty pharmacy billing industry is quickly evolving as it is driven by increasing demand for expensive specialty medications. It has been observed that the key trends will influence the billing process of specialty pharmacies to a large extent. These shifts can enhance billing accuracy and streamline all the administrative workflows.

Billing for gastroenterology can be considered a highly challenging task. It involves complex coding requirements, documentation needs, prior authorization changes, and ever-evolving regulations. Now, you may have this question: "Why do the regulations change so often"? It is because new diseases are coming every single year.

Cardiology is one of the most in-demand medical specialties, but it also comes with some of the most complex procedures, coding requirements, and strict insurance rules. You might think billing is just about sending claims and getting paid, but in reality, cardiology billing services handle claims that involve high-value treatments and sensitive compliance requirements. The harsh truth is that you have several bumpy roads ahead, like wrong codes, missing documentation, prior authorization issues, etc.

Healthcare is growing fast, with hospitals, physician groups, outpatient centers, and specialty clinics all under one system. But this growth creates a hidden problem—fragmented billing. Different processes across facilities mean money slips away. Denials rise. Payments slow. Staff get stressed. Patients get annoyed. And health systems lose millions without even noticing. Now you need to know what fragmented billing is, the real cost of fragmented billing is, and how a professional health system billing company can fix it and protect your revenue.