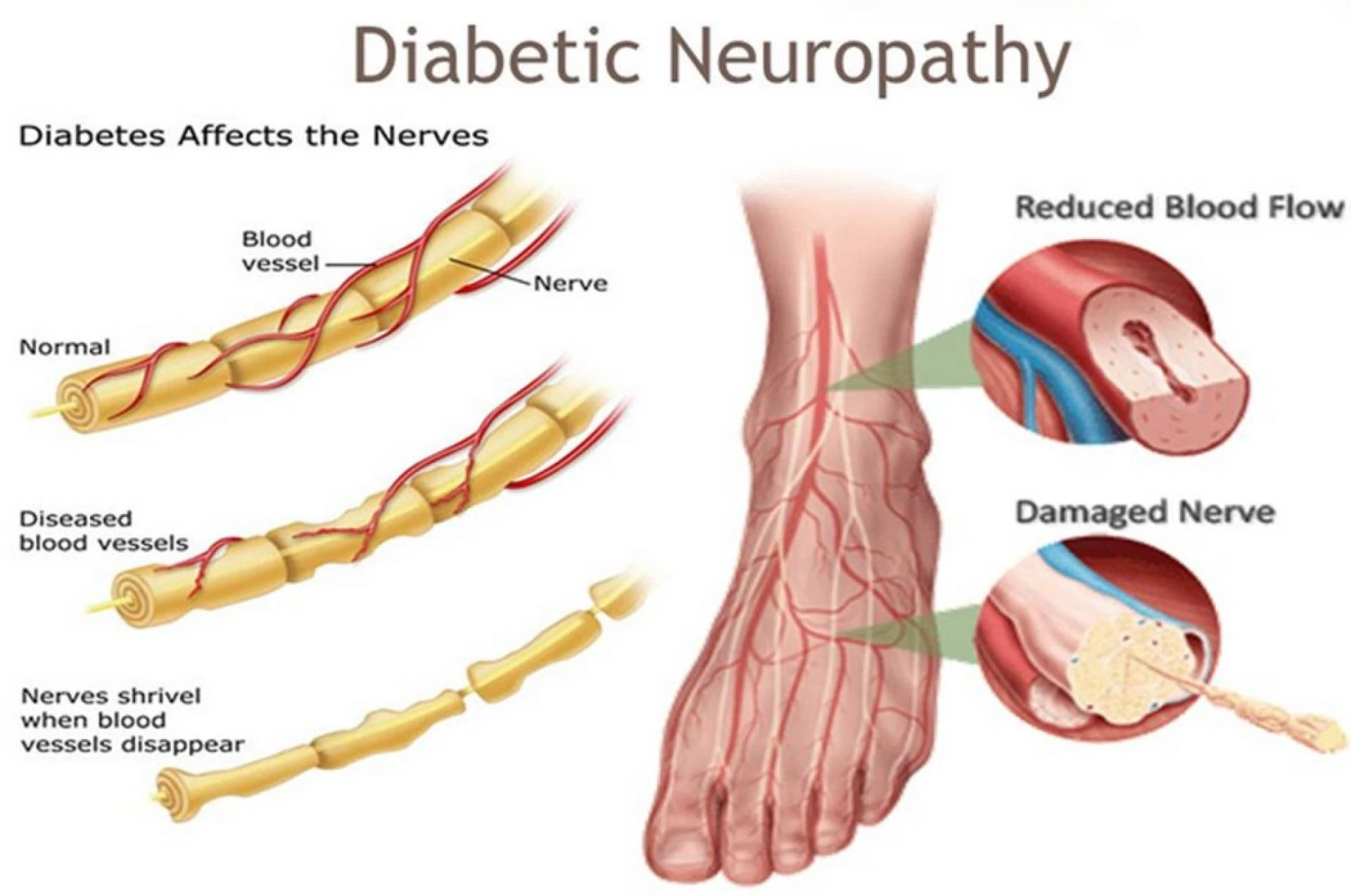
Diabetic neuropathy is a type of nerve injury that can result from high blood sugar. In both type 1 and type 2 diabetes, diabetic neuropathy is a dangerous and common consequence. It is a form of nerve injury brought on by persistently high blood sugar. In most cases, the condition takes years or even decades to fully manifest.
One potential side effect of persistently high blood sugar levels is nerve damage. Your nerves are damaged by high blood sugar, and as a result, they may stop communicating with various body organs. The health effects of nerve injury can range from mild tingling to excruciating pain that makes it difficult to carry out daily tasks. Your diabetes treatment plan must include regular blood sugar monitoring. You can avoid significant health issues in the future by doing this, in addition to helping you maintain normal health.
Most diabetics suffer from nerve degeneration. The good news is that you can delay or possibly prevent it by maintaining blood sugar levels that are as close to ideal as you can. The goal of diabetic neuropathy treatment is to lessen painful symptoms and slow the progression of the disease. It's essential to identify your symptoms early in order to take steps to prevent nerve damage from worsening. Symptoms of nerve damage typically appear gradually.
TYPES OF DIABETIC NEUROPATHY
There are various forms of diabetic neuropathy. This is due to the various types of nerves that our bodies contain and their varied functions. Depending on the type of diabetic neuropathy you have, your symptoms and treatments will vary.
The four main types of diabetic neuropathy are:
Peripheral NeuropathyAutonomic NeuropathyProximal NeuropathyFocal Neuropathy
PERIPHERAL NEUROPATHY
The terms distal polyneuropathy and peripheral diabetic nerve pain are also used to describe peripheral neuropathy. The most typical diabetes-related neuropathy is peripheral neuropathy. It affects the nerves that control your feet, legs, hands, and arms. The nerves in your feet are the longest in your body because they must travel a significant distance from the lumbar area (low back), where they split off from the spinal cord, to the feet and legs. Since the nerves connecting to your feet are so lengthy, it is most frequently these nerves that are destroyed. This nerve damage can result in the foot problems that are frequently linked to diabetes, such as foot deformities, infections, ulcers, and amputations. Symptoms include tingling, numbness, pain, and burning sensation. Every diabetes patient needs to inspect their feet and legs every day, moisturise their feet if they are dry, wear comfortable shoes, and take care of their toenails.
AUTONOMIC NEUROPATHY
Autonomic neuropathy is the second most typical kind of neuropathy in diabetics. Blood pressure, heart rate, sweat glands, eyes, bladder, digestive system, and sex organs are all under the control of the autonomic nervous system. Any of these nerves can be impacted by diabetes. Sexual issues including erectile dysfunction, dry vagina, or difficulties eliciting an orgasm can also be brought on by autonomic neuropathy. Bladder neuropathy can result in incontinence or make it difficult to completely empty your bladder. Constipation, diarrhoea, difficulty swallowing, and gastroparesis (a condition where the stomach empties into the small intestines too slowly) can all be brought on by nerve injury to the digestive tract.
Additionally, individuals with autonomic neuropathy may not notice hypoglycemic signs like perspiration and heart palpitations. This may result in you being unaware that you have low blood sugar, which raises the possibility of a hypoglycemia emergency. Some heart attack symptoms may be difficult to recognise if you have autonomic neuropathy. When your heart doesn't get enough oxygen, you might not experience any chest pain. Your heart rate and blood pressure can respond more slowly if the nerves that regulate them are damaged. When you rise up after sitting or lying down, or when you exert yourself, you can notice a dip in blood pressure and feel lightheaded or dizzy. An unusually rapid heart rate can also be brought on by autonomic neuropathy.
PROXIMAL NEUROPATHY
This is also known as diabetic amyotrophy. Typically, the nerves in the thighs, hips, buttocks, or legs are affected by this type of neuropathy. The chest and abdominal regions may also be impacted. Typically, symptoms only affect one side of the body, although they occasionally affect the other side as well. Symptoms include excruciating hip, thigh, or buttock pain, weakening and shrinking leg muscles, trouble getting out of a sitting position, and pain in the chest or abdominal wall. It typically affects diabetic elderly persons. Unlike peripheral neuropathy, it usually goes away with time or medication.
FOCAL NEUROPATHY
When one particular nerve or set of nerves are damaged, it is known as focal neuropathy or mononeuropathy and results in weakness in the affected area. You typically experience this in your hand, head, body, or leg. It comes suddenly and is usually excruciatingly painful. Most focal neuropathies disappear after a few weeks or months, much like proximal neuropathy, and do not cause any long-term harm.
Neuropathy caused by diabetes cannot be reversed. The best approach at the moment is to control blood sugar levels by medication and lifestyle modifications. The risk of developing neuropathy and associated effects can be decreased by maintaining glucose levels within the therapeutic range.
0






Sign in to leave a comment.