Diabetic retinopathy is a potentially serious eye condition that can result from diabetes, particularly when it's poorly controlled. It affects the blood vessels in the retina, which is the light-sensitive tissue at the back of the eye. Diabetic retinopathy can lead to vision impairment and even blindness if left untreated. While there is no cure for diabetic retinopathy in the sense of reversing the damage completely, there are several effective treatments and management strategies to prevent or slow down its progression and preserve vision. In this detailed guide, we will explore these treatments and strategies.
Understanding Diabetic Retinopathy:
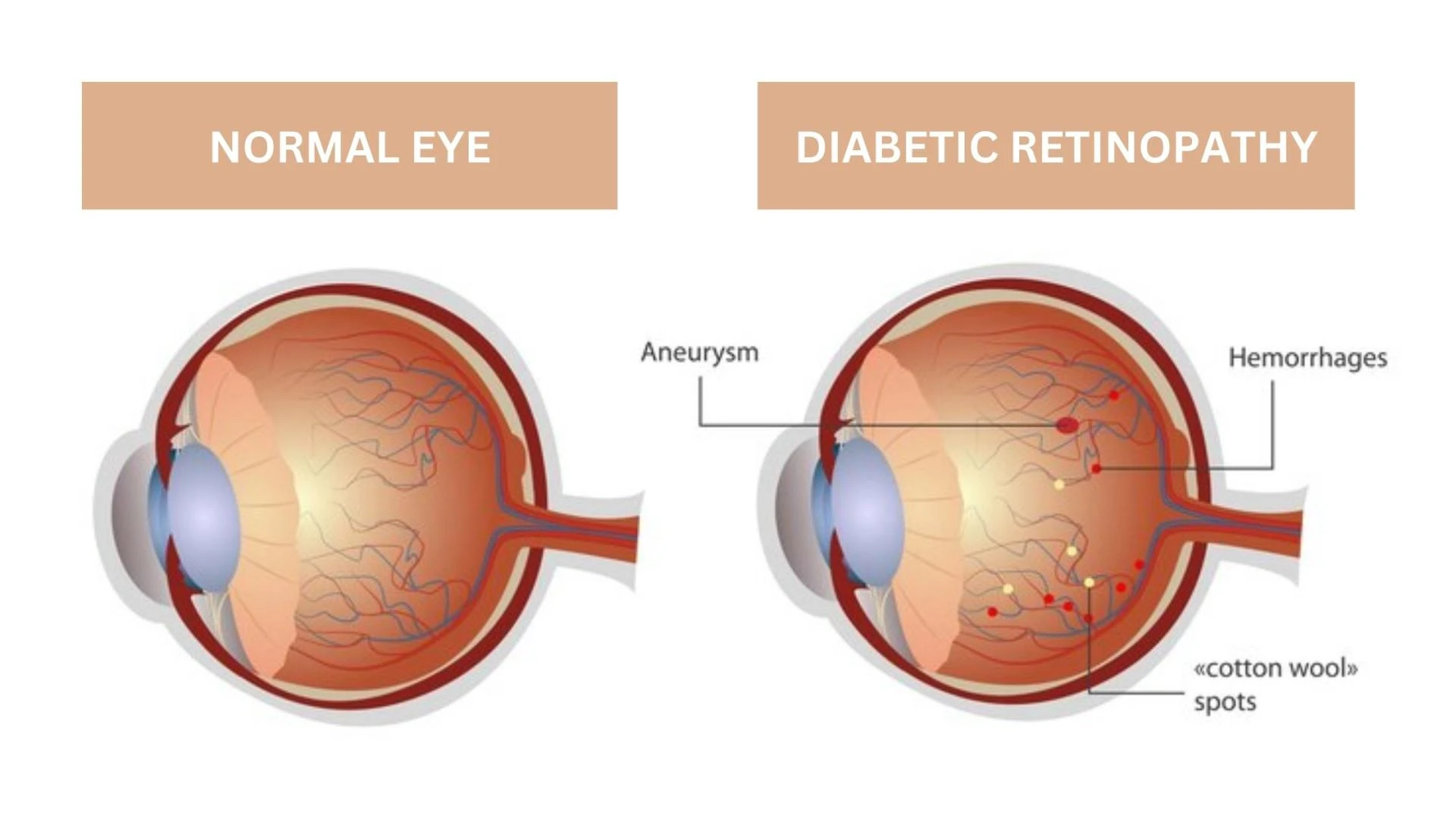
Diabetic retinopathy develops due to prolonged exposure to high blood sugar levels, which can damage the delicate blood vessels in the retina. There are two main stages of diabetic retinopathy:
Non-Proliferative Diabetic Retinopathy (NPDR): In this early stage, small blood vessels in the retina leak fluid or blood. Symptoms may not be noticeable at this stage, but it can progress to more severe forms of the disease if not managed.
Proliferative Diabetic Retinopathy (PDR): In this advanced stage, new, abnormal blood vessels begin to grow on the surface of the retina. These new vessels are fragile and can cause bleeding, scarring, and retinal detachment, leading to severe vision loss.
Prevention and Management:
The best approach to managing diabetic retinopathy is through prevention and early intervention. Here are key steps to prevent or slow its progression:
1. Diabetes Control:
The most critical aspect of managing diabetic retinopathy is keeping your diabetes under control. This involves:
Monitoring blood sugar levels regularly and as directed by your healthcare provider.Adhering to a diabetes management plan that may include medication, insulin, diet, and exercise.Maintaining a target HbA1c level as advised by your healthcare provider.Good blood sugar control can significantly reduce the risk of developing or progressing diabetic retinopathy.
2. Regular Eye Exams:
Annual comprehensive eye exams are crucial for individuals with diabetes, even if there are no apparent vision problems. Early detection of diabetic retinopathy is key to effective treatment.3. Blood Pressure and Cholesterol Control:
High blood pressure and cholesterol can exacerbate diabetic retinopathy. Monitor and manage these conditions as recommended by your healthcare provider.4. Lifestyle Changes:
Adopt a healthy lifestyle that includes a balanced diet, regular exercise, and avoiding smoking and excessive alcohol consumption. These changes can help manage diabetes and protect your eyes.5. Medication Adherence:
If your healthcare provider prescribes medications or eye drops to manage diabetes or eye-related issues, take them as directed and do not skip doses.Treatment Options for Diabetic Retinopathy:
While there is no cure for diabetic retinopathy, several treatment options are available to manage the condition and prevent vision loss:
1. Laser Therapy (Photocoagulation):
Laser treatment is commonly used to treat diabetic retinopathy. In this procedure, a laser beam is focused on the damaged blood vessels to seal leaks or shrink abnormal vessels.Laser therapy can help reduce swelling and prevent further damage to the retina.It may be used in both NPDR and PDR stages.2. Intravitreal Injections:
Intravitreal injections involve injecting medication directly into the vitreous gel of the eye. These medications can help reduce swelling, inhibit the growth of abnormal blood vessels, and slow the progression of diabetic retinopathy.Anti-VEGF drugs (Vascular Endothelial Growth Factor inhibitors) are commonly used for this purpose.3. Vitrectomy:
Vitrectomy is a surgical procedure used in advanced cases of diabetic retinopathy, particularly when there is significant bleeding or retinal detachment.During a vitrectomy, the vitreous gel is removed, and any scar tissue or blood is carefully cleared. The eye is then filled with a clear solution.This procedure can help improve vision but is usually considered when other treatments have not been successful.4. Focal Laser Treatment:
Focal laser treatment, also known as focal/grid photocoagulation, is used to treat macular edema (swelling of the macula, the central part of the retina).In this treatment, the laser is applied to specific, well-defined areas of the retina to reduce edema and improve vision.5. Scatter Laser Treatment (Panretinal Photocoagulation):
Panretinal photocoagulation is used to treat proliferative diabetic retinopathy. It involves applying scattered laser burns to the peripheral retina to reduce the growth of abnormal blood vessels.While this treatment can be effective, it may cause some loss of peripheral vision.6. Corticosteroids:
Corticosteroids, delivered as injections or implants, may be used to reduce inflammation and swelling in the eye, especially in cases of diabetic macular edema.7. Artificial Retina:
In some advanced cases, an artificial retina (ocular prosthesis) may be considered to restore partial vision. This is a complex procedure and not commonly performed.8. Regular Follow-up:
Regardless of the treatment method chosen, regular follow-up appointments with your ophthalmologist are essential to monitor the condition and adjust the treatment plan as needed.9. Supportive Measures:
Visual aids such as magnifiers and low-vision devices can be helpful for individuals with significant vision loss due to diabetic retinopathy.Conclusion:
While there is no cure for diabetic retinopathy, early detection, good diabetes management, and timely treatment can help prevent or slow down its progression and preserve vision. Regular eye exams, lifestyle changes, and adherence to medical advice are essential components of managing diabetic retinopathy. Each individual's case is unique, so it's important to work closely with your healthcare team, including your eye specialist, to develop a personalized plan for managing diabetic retinopathy and maintaining optimal eye health.






Sign in to leave a comment.