Intracytoplasmic Sperm Injection (ICSI) has transformed the landscape of assisted reproductive technology (ART), offering hope to couples struggling with severe male infertility. This article explores the nuances of ICSI, its distinctions from traditional IVF, and its pivotal role in modern fertility treatments.
Understanding ICSI: Precision in Fertilization
ICSI is a cutting-edge ART procedure where a single sperm is directly injected into an egg’s cytoplasm to achieve fertilization. This technique is particularly vital for cases involving:
- Severe male infertility (e.g., extremely low sperm count or poor motility).
- Abnormal sperm morphology (misshapen sperm).
- Failed prior IVF attempts or surgically retrieved sperm.
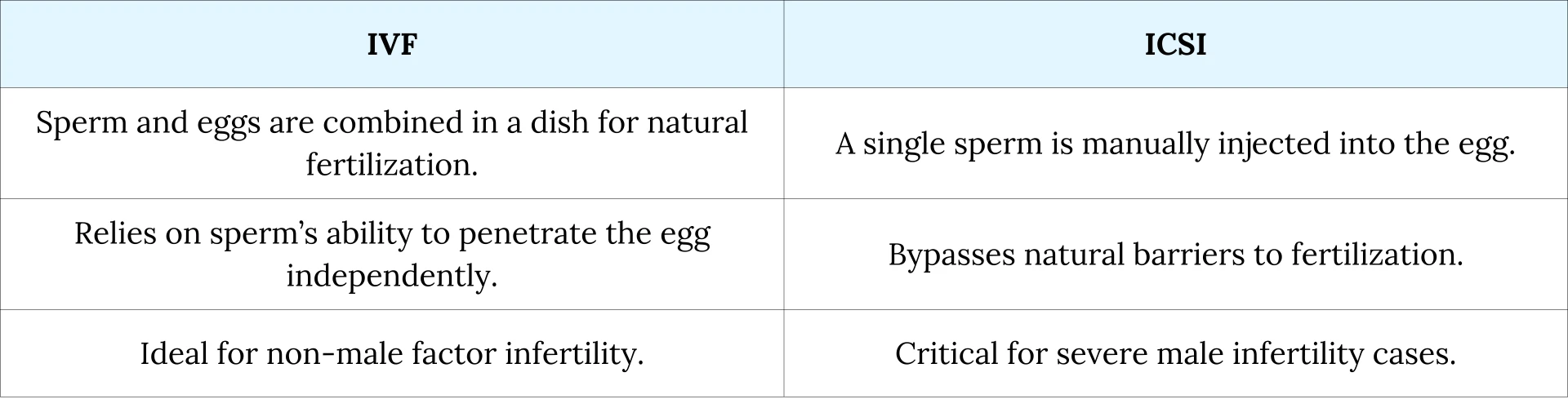
ICSI vs. IVF : Key Differences
While both ICSI and IVF involve fertilizing eggs outside the body, their approaches differ fundamentally :
ART encompasses methods to achieve pregnancy through medical intervention. ICSI stands out as one of the most advanced techniques, alongside:
- IVF-ET (In Vitro Fertilization-Embryo Transfer).
- IUI (Intrauterine Insemination).
- FET (Frozen Embryo Transfer).
- GIFT/ZIFT (Gamete/Zygote Intrafallopian Transfer).
Success Rates and Factors Influencing ICSI Outcomes
ICSI boasts high success rates, particularly for male infertility, but outcomes depend on:
- Female partner’s age and egg quality.
- Sperm viability (even with severe abnormalities).
- Embryologist expertise in micromanipulation.
Studies show that ICSI achieves fertilization in 70-80% of cases where traditional IVF might fail.
The ICSI Procedure: Step-by-Step
- Ovarian Stimulation: The female undergoes hormone therapy to produce multiple eggs.
- Egg Retrieval: Mature eggs are collected via a minor surgical procedure.
- Sperm Collection: Sperm is obtained via ejaculation or surgical extraction (e.g., TESE).
- Microinjection: An embryologist injects a single sperm into each egg using a specialized glass needle.
- Embryo Monitoring: Fertilized eggs develop into embryos over 3–5 days.
- Embryo Transfer: Viable embryos are implanted into the uterus.
Who Benefits from ICSI?
- Couples with male factor infertility (low count, poor motility, abnormal morphology).
- Those with prior IVF failures due to fertilization issues.
- Individuals requiring surgical sperm retrieval (e.g., obstructive azoospermia).
Best Practices for Couples Undergoing ICSI
Do’s:
- Follow medication protocols strictly.
- Prioritize a nutrient-rich diet and stress management.
- Don’ts:
- Avoid strenuous activities post-embryo transfer.
- Skip alcohol or tobacco during treatment.
FAQs for Aspiring Embryologists
Q: Is ICSI riskier than IVF?
A: Risks are minimal but include slight chances of egg damage. Success hinges on embryologist skill.
Q: How long does ICSI take?
A: The injection itself takes minutes per egg, but the full cycle spans 4–6 weeks.
Q: Can ICSI guarantee pregnancy?
A: No, but it significantly improves fertilization chances in male infertility cases.
Q: Are ICSI babies healthy?
A: Most ICSI-conceived children are healthy, though genetic counseling is advised for severe male factor cases.
ICSI’s Legacy in Fertility Care
ICSI remains a cornerstone of ART, offering hope where natural conception seems impossible. For embryologists, mastering this technique demands precision, but the reward—helping families thrive—is unparalleled. As male infertility rates rise globally, ICSI’s role in fertility treatment will only grow, underscoring the need for continuous innovation and expertise.







Sign in to leave a comment.