Orthopedic practices face some of the highest claim denial rates in all of medicine. Complex surgical bundling rules, implant billing, and multi-stage treatment plans create a revenue cycle nightmare that generic billing teams simply cannot solve.
The right orthopedic billing company changes everything. Practices that invest in specialty-specific billing expertise recover lost revenue, cut denial rates dramatically, and reclaim the time surgeons waste on administrative chaos.
This guide reveals exactly what separates elite orthopedic billing services from generic alternatives, which critical metrics to track, and how to choose a partner that protects every dollar your practice earns.
What Does an Orthopedic Billing Company Do?
An orthopedic billing company manages the complete revenue cycle for orthopedic surgery practices, sports medicine clinics, and musculoskeletal care providers. Services include insurance verification, orthopedic-specific CPT and ICD-10 coding, claim submission, implant and device billing, payment posting, denial management, and patient collections. Because orthopedic procedures carry high reimbursement values and extreme coding complexity, specialized billing expertise directly impacts a practice's financial survival.
Why Orthopedic Billing Requires Specialty-Level Expertise
Orthopedics is not a simple evaluation-and-management specialty. Surgeons perform multi-level spinal fusions, total joint replacements, arthroscopic repairs, and fracture fixations each carrying unique coding, documentation, and payer rules. A general billing team without orthopedic training leaves significant revenue on the table.
Surgical Bundling and Unbundling
Orthopedic procedures trigger more NCCI (National Correct Coding Initiative) bundling edits than nearly any other specialty. Payers aggressively bundle related procedures performed during a single surgical session.
Consider a surgeon who performs an ACL reconstruction and a partial meniscectomy during the same knee arthroscopy. Without proper modifier application and clinical documentation, the payer bundles the meniscectomy into the ACL repair and pays for only one procedure. A skilled orthopedic billing company identifies every legitimately separable service, applies the correct modifier 59 or XE/XS/XP/XU modifiers, and submits supporting operative notes to justify unbundled billing.
This single capability can recover thousands of dollars per case.
Implant and Hardware Billing
Joint replacements and spinal surgeries frequently involve expensive implants, screws, plates, and cages. Billing for these devices varies drastically by payer. Some commercial insurers reimburse implants separately. Medicare bundles them into the facility payment under MS-DRG rules.
An experienced orthopedic billing company understands these distinctions. They track implant costs, negotiate carve-out agreements when possible, and ensure device charges appear correctly on claims to maximize reimbursement without triggering audits.
Global Period Management
Most orthopedic surgeries carry 90-day global periods. During this window, the payer considers follow-up visits part of the original surgical fee. However, unrelated problems, complications requiring a return to the operating room, or new injuries during the global period qualify for separate billing.
Accurately applying modifier 24 (Unrelated E/M During Global Period), modifier 78 (Return to OR for Related Procedure), or modifier 79 (Unrelated Procedure During Global Period) requires deep orthopedic billing knowledge. Errors here either leave money uncollected or create compliance risks.
Core Orthopedic Billing Services Your Practice Needs
Comprehensive orthopedic billing services cover every revenue-impacting touchpoint. Here is what a top-tier partner delivers:
- Pre-Authorization and Verification: Confirming insurance eligibility, surgical pre-authorization, and implant pre-certification before every procedure to eliminate front-end denials.
- Orthopedic-Specific Coding: Certified coders trained in musculoskeletal CPT codes (20000–29999 series), spinal surgery coding, pain management injection coding, and DME billing.
- Operative Note Review: Detailed analysis of surgeon dictation to capture every billable component including assistant surgeon fees, co-surgery arrangements, and add-on procedures.
- Clean Claim Submission: Scrubbing claims against NCCI edits, LCD/NCD policies, and payer-specific rules before electronic submission to clearinghouses.
- Payment Reconciliation: Comparing every ERA/EOB against contracted fee schedules to detect underpayments, incorrect adjustments, and improper bundling by payers.
- Denial Management and Appeals: Root-cause analysis of every rejected claim with rapid corrective resubmission and multi-level appeals backed by clinical documentation.
- Workers' Compensation and Auto Accident Billing: Managing the unique requirements of injury-related claims, including state-specific fee schedules, adjuster communications, and lien tracking.
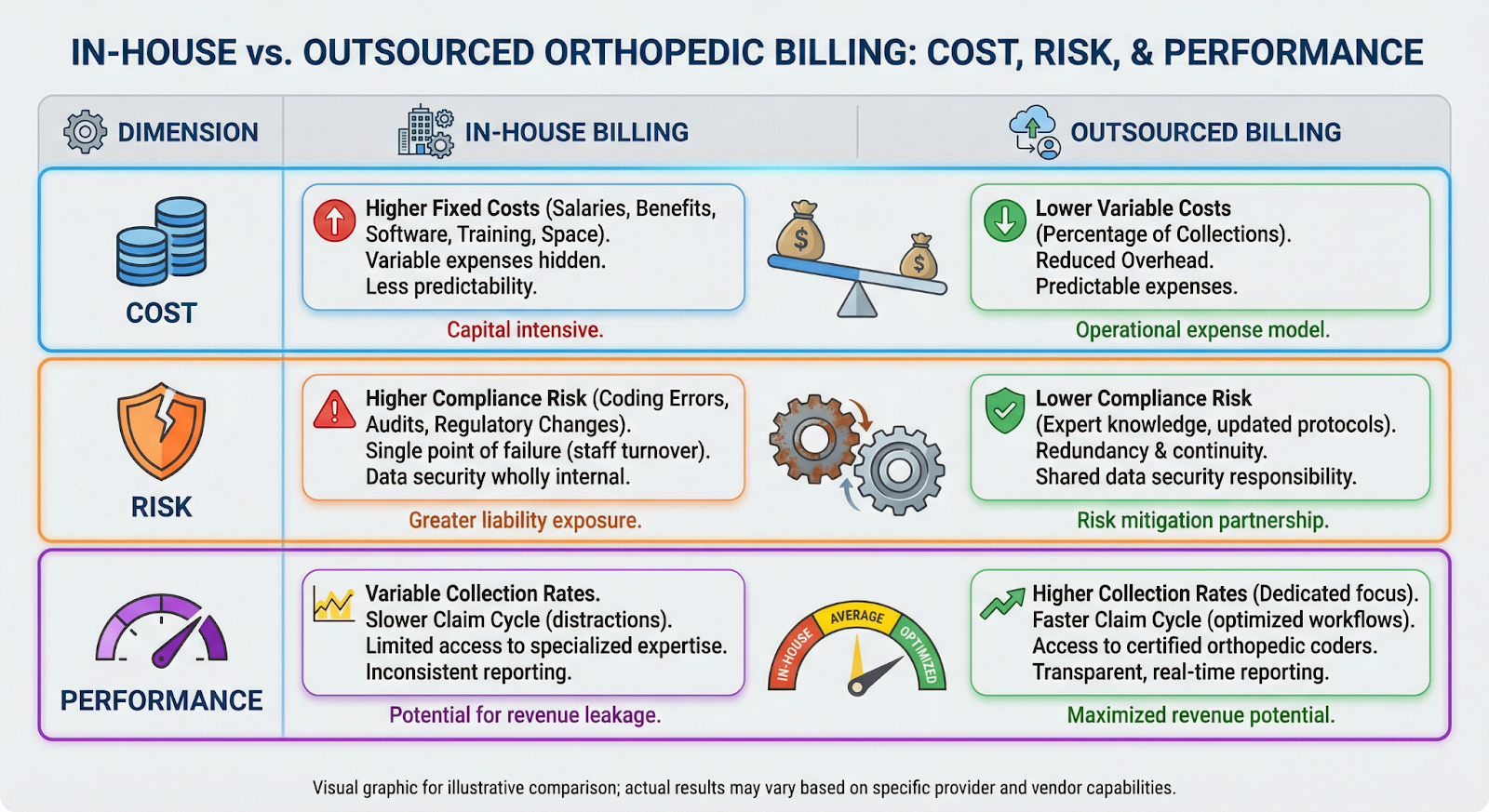
In-House Billing vs. Outsourced Orthopedic Billing Company
The decision between managing billing internally and outsourcing to a specialist partner shapes your practice's long-term profitability.
Hidden Costs of In-House Operations
Building an internal team demands hiring certified orthopedic coders a scarce and expensive talent pool. You must also fund billing software, clearinghouse subscriptions, compliance training, and employee benefits. Staff turnover disrupts claim flow and creates immediate revenue gaps during recruitment cycles.
Many orthopedic practices discover their true cost-to-collect exceeds 10% of revenue when they fully account for overhead, technology, and lost productivity.
The Outsourcing Advantage
An orthopedic billing company distributes premium technology and specialized coder salaries across its entire client base. Your practice accesses enterprise-level tools and deep orthopedic expertise at a fraction of the in-house cost.
Performance-based pricing typically a percentage of net collections aligns the billing company's financial incentive directly with your revenue. They earn more only when you collect more.
| Factor | In-House Billing | Outsourced Orthopedic Billing |
| Coder Expertise | Hard to recruit; costly to retain | Orthopedic-certified team included |
| Technology Cost | Self-funded software and updates | Included in service |
| Staffing Risk | Revenue disruption during turnover | Fully managed, no gaps |
| Scalability | Limited by headcount | Scales with volume instantly |
| Pricing Model | Fixed overhead regardless of revenue | Variable, pay-for-performance |
KPIs an Orthopedic Billing Company Must Deliver
Track these metrics to evaluate whether your billing operation performs at an elite level:
- First-Pass Clean Claim Rate: Claims accepted by payers on initial submission. A strong orthopedic billing company maintains rates above 96%.
- Days in Accounts Receivable: The average collection timeline. Aim for fewer than 35 days for optimal cash flow.
- Denial Rate: Percentage of claims rejected. Specialty billing partners keep this below 4%, far under the industry average.
- Net Collection Rate: Revenue collected versus total allowed charges. Top performers consistently exceed 97%.
- Underpayment Recovery Rate: The percentage of detected underpayments successfully recovered from payers. This metric alone can add tens of thousands annually.
Costly Orthopedic Billing Mistakes to Eliminate
Even experienced teams make errors that silently drain revenue. Watch for these common pitfalls:
- Missed Add-On Codes: Surgeons frequently perform additional procedures during a primary surgery. Failing to capture add-on CPT codes like 22614 (additional spinal segment) leaves significant money uncollected.
- Incorrect Laterality Coding: Orthopedics demands precise laterality modifiers (LT, RT, 50). Submitting a right knee arthroscopy code without modifier RT triggers an immediate denial.
- Ignoring LCD Medical Necessity Requirements: Payers enforce Local Coverage Determinations that require specific ICD-10 diagnosis codes to justify advanced imaging and surgical procedures. Generic diagnosis codes result in denied claims.
- Failing to Bill for DME: Post-surgical braces, crutches, bone stimulators, and CPM machines qualify for separate reimbursement. Many practices never submit these claims.
- Accepting Payer Underpayments: Without systematic fee schedule comparison, practices unknowingly accept payments below contracted rates. Over a year, these shortfalls accumulate into massive revenue losses.
How to Choose the Best Orthopedic Billing Company
Use this structured evaluation framework to identify a partner that truly protects your revenue:
- Demand Orthopedic-Specific References: Ask for client testimonials and case studies from orthopedic surgery practices, sports medicine groups, or spine surgery centers. Reject vendors who cannot demonstrate deep specialty experience.
- Verify Coder Certifications: Ensure the team includes AAPC-certified coders with orthopedic specialization (COSC-Certified Orthopedic Surgery Coder) or equivalent credentials.
- Test EHR and PM Integration: Confirm seamless connectivity with your existing practice management system and EHR. Data should flow without manual entry or double documentation.
- Evaluate Reporting Transparency: Require 24/7 access to real-time dashboards displaying claim status, denial trends, AR aging, and collection performance. Never accept monthly PDF summaries as your only window into financial data.
- Assess Compliance Rigor: Confirm the company conducts regular internal coding audits, maintains HIPAA compliance certifications, and carries errors-and-omissions insurance.
Frequently Asked Questions
What makes orthopedic billing harder than other specialties?
Orthopedic billing involves complex surgical bundling rules, 90-day global surgical periods, implant and hardware billing, laterality modifiers, and frequent workers' compensation claims. These factors demand coders with specific orthopedic training to prevent revenue loss and compliance issues.
How much does an orthopedic billing company charge?
Most orthopedic billing companies charge between 4% and 9% of net collections. The percentage depends on practice size, surgical volume, payer mix, and scope of services. Performance-based pricing ensures you pay only when revenue is successfully collected.
How fast will I see results after switching billing companies?
Practices typically notice measurable improvements within 60 to 90 days. Denial rates drop, AR days shorten, and net collections increase as the new team corrects systemic errors and implements proactive claim management workflows.
Will I still control my financial data?
Yes. A reputable orthopedic billing company provides full transparency through real-time reporting dashboards. You maintain complete visibility into every claim, payment, denial, and financial trend often with greater detail than in-house teams provide.
Can an orthopedic billing company handle workers' comp and personal injury cases?
Absolutely. Experienced orthopedic billing services manage workers' compensation, auto accident, and personal injury claims. They navigate state-specific fee schedules, handle adjuster communications, file liens when appropriate, and pursue full reimbursement on complex injury cases.
Take Control of Your Orthopedic Revenue Today
Every undercoded surgery, missed implant charge, and accepted underpayment costs your practice real money. These losses multiply over months and years, quietly undermining your financial foundation.
You built your practice around clinical excellence. Your billing operation should match that standard. A specialized orthopedic billing partner brings the coding precision, payer expertise, and relentless follow-up your revenue cycle demands.
Stop leaving earned revenue behind. Explore how a trusted orthopedic billing company can eliminate denials, recover underpayments, and accelerate your cash flow starting now.




Sign in to leave a comment.