Sterilization plays a vital role in maintaining safety and preventing contamination in laboratories, hospitals, and pharmaceutical facilities. Instruments, medical tools, and laboratory materials must be completely free of microorganisms to ensure accurate research results and safe medical procedures. One of the most reliable methods used worldwide is the autoclave sterilization process.
Autoclaves use high-temperature steam under pressure to eliminate bacteria, viruses, fungi, and spores from equipment and materials. This method is widely trusted because it is both effective and consistent. From research laboratories to surgical departments, autoclaves are essential tools for maintaining strict sterilization standards.
While understanding how the sterilization cycle works is important, organizations must also consider equipment selection, maintenance, and operational factors such as the cost of an autoclave. This guide explains how autoclave sterilization works, the steps involved in the process, and why it is widely used in both laboratory and medical environments.
What Is an Autoclave?
An autoclave is a specialized machine designed to sterilize equipment and materials using pressurized steam at high temperatures. The combination of heat, moisture, and pressure destroys microorganisms that could cause contamination or infection.
Autoclaves are commonly used in:
- Hospitals and healthcare facilities
- Medical research laboratories
- Biotechnology laboratories
- Pharmaceutical manufacturing plants
- Academic research institutions
The device typically consists of a sealed pressure chamber, a heating system, control panels, safety valves, and monitoring sensors. These components work together to create a controlled environment where steam sterilization can occur safely and effectively.
Autoclaves are capable of sterilizing a wide variety of materials, including surgical instruments, glassware, laboratory media, metal tools, and certain types of waste.
How an Autoclave Work
Understanding how an autoclave works helps explain why steam sterilization is so effective. The system relies on the ability of steam under pressure to transfer heat efficiently and penetrate surfaces.
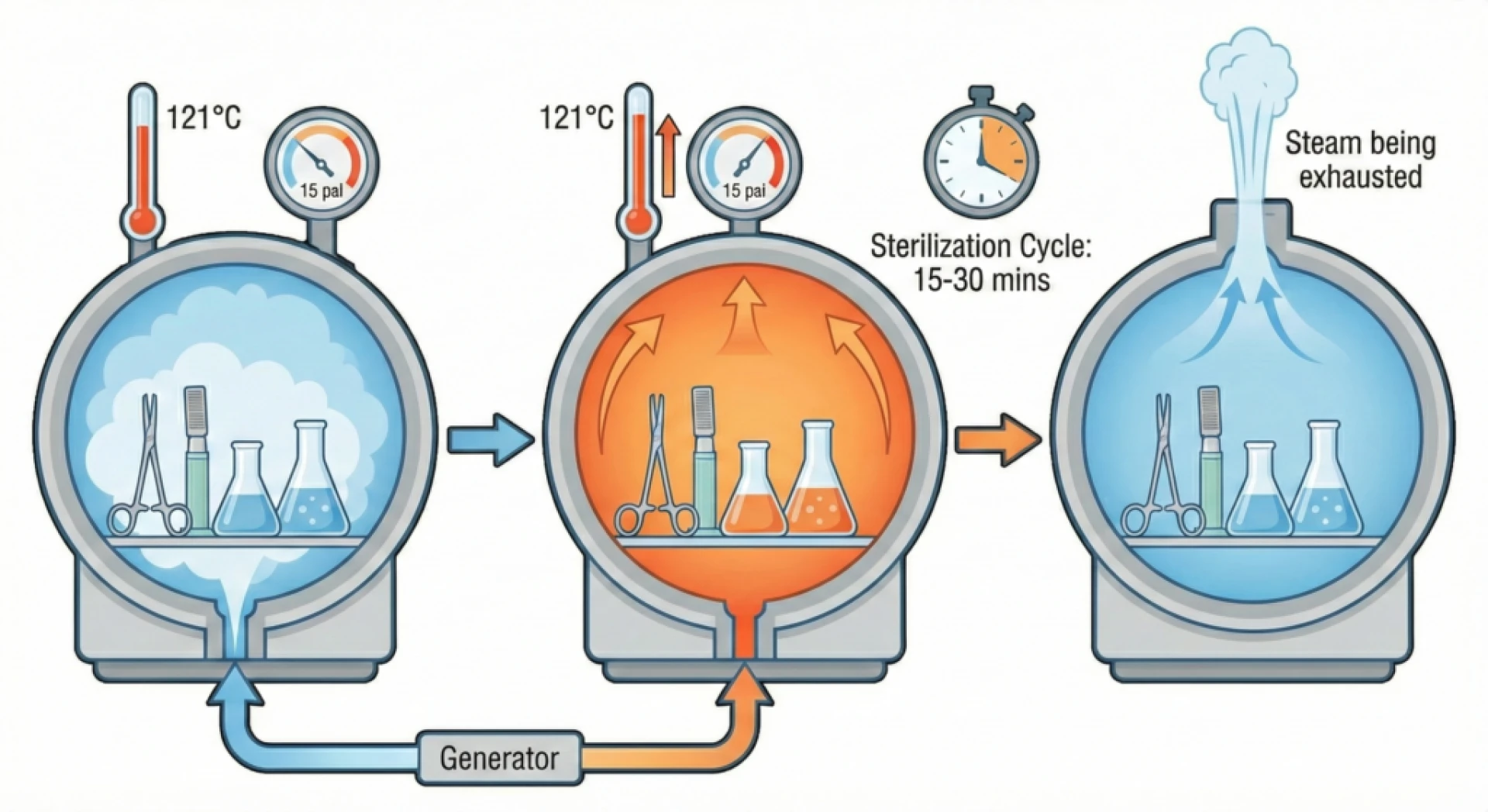
The process begins when water inside the autoclave is heated to produce steam. As the chamber fills with steam, air is removed either through gravity displacement or a vacuum pump. Removing air is important because steam transfers heat much more effectively than dry air.
Once the chamber is filled with steam, pressure increases. This allows the temperature inside the chamber to rise above the normal boiling point of water. Most sterilization cycles operate at temperatures between 121°C and 134°C.
At these high temperatures, microorganisms are destroyed because their proteins and enzymes become denatured. This effectively kills bacteria, viruses, and spores that may be present on the items being sterilized.
Steps in the Autoclave Sterilization Process
The sterilization cycle inside an autoclave follows several carefully controlled stages to ensure effective results.
Preparation and Loading
Before sterilization begins, all items must be properly prepared. Instruments and materials should be cleaned to remove visible debris because organic material can interfere with the sterilization process.
Items are then arranged inside the chamber to allow steam to circulate freely. Overloading the chamber can reduce the effectiveness of sterilization.
Air Removal
Air trapped inside the chamber must be removed before sterilization can occur. Autoclaves typically use one of two methods for this step: gravity displacement or vacuum systems.
Removing air allows steam to reach every surface of the materials being sterilized.
Sterilization Phase
Once the chamber is filled with steam and the required pressure is reached, the sterilization stage begins. During this stage, the temperature and pressure remain constant for a predetermined period.
This exposure time ensures that microorganisms are completely destroyed.
Exhaust Phase
After sterilization is complete, the autoclave gradually releases pressure and steam from the chamber. This stage prepares the chamber for the final drying process.
Drying Phase
In the final stage, moisture is removed from sterilized items. Many modern autoclaves include drying cycles that use heat or vacuum systems to eliminate remaining moisture.
Drying is especially important for medical instruments and laboratory materials that must remain sterile until use.
Sterilization Process for Medical Devices
Autoclaves play a critical role in the sterilization process for medical devices used in hospitals and healthcare facilities. Surgical instruments, diagnostic tools, and reusable medical equipment must be completely sterile to prevent infections.
Medical sterilization standards are strictly regulated by health authorities to ensure patient safety. Hospitals follow detailed procedures to ensure that instruments are cleaned, packaged, sterilized, and stored correctly.
Monitoring systems are also used to confirm that sterilization cycles reach the required temperature and pressure levels. Biological and chemical indicators are often used to verify that the sterilization process has been successful.
These quality control measures ensure that sterilized medical devices meet strict healthcare safety standards.
Types of Autoclave Sterilization Cycles
Different types of sterilization cycles are used depending on the materials being processed.
Gravity Displacement Cycle
This is one of the most common sterilization methods. Steam enters the chamber and displaces the air downward and out through a drain.
This cycle is typically used for sterilizing glassware, liquids, and simple laboratory equipment.
Pre-Vacuum Cycle
Pre-vacuum autoclaves remove air from the chamber using a vacuum pump before steam is introduced. This method ensures more thorough steam penetration and is often used for complex medical instruments.
Flash Sterilization
Flash sterilization is a rapid cycle used in situations where instruments are needed immediately. While effective, it is generally reserved for emergency situations due to the short cycle time.
Factors That Affect Sterilization Efficiency
Several factors influence how effective an autoclave sterilization cycle will be.
Temperature and pressure must be maintained at the correct levels throughout the cycle. Insufficient heat or pressure may allow microorganisms to survive.
Exposure time is also critical. Items must remain at the required temperature for a specific duration to ensure complete sterilization.
Proper loading of the chamber is equally important. If materials are packed too tightly, steam may not reach all surfaces.
Regular maintenance of the autoclave ensures that sensors, valves, and heating systems function correctly. Proper maintenance helps maintain consistent sterilization performance.
Cost Considerations for Autoclave Equipment
When laboratories or healthcare facilities invest in sterilization equipment, they must evaluate both performance and budget considerations.
The price of an autoclave can vary widely depending on its size, capacity, automation features, and safety systems. Smaller laboratory models are generally less expensive, while large hospital-grade units with advanced control systems cost significantly more.
Organizations should also consider long-term operating expenses such as energy consumption, maintenance, and replacement parts when evaluating equipment options.
Although the purchase price is an important factor, selecting a reliable and efficient system often provides better value over time.
Advantages of the Autoclave Sterilization Method
Autoclave sterilization offers several advantages that make it one of the most widely used sterilization techniques.
First, it is extremely effective at destroying microorganisms, including highly resistant bacterial spores. This ensures a high level of sterilization reliability.
Second, steam sterilization is relatively fast compared to some chemical sterilization methods. Many autoclave cycles can be completed within a short period of time.
Third, the process is environmentally friendly because it uses water and heat rather than potentially harmful chemicals.
Finally, autoclaves are widely accepted in both medical and laboratory industries due to their consistent and proven performance.
Conclusion
Sterilization is essential for maintaining safe laboratory environments and protecting patients in healthcare facilities. Autoclaves provide one of the most reliable and widely accepted methods for eliminating microorganisms from instruments and materials.
By understanding the stages of the sterilization cycle, laboratories and medical professionals can ensure that equipment is processed safely and effectively. Proper loading techniques, correct cycle settings, and regular maintenance all contribute to successful sterilization outcomes.
Autoclaves continue to play a vital role in scientific research, medical treatment, and pharmaceutical development, helping organizations maintain the highest standards of safety and hygiene.

















Sign in to leave a comment.