When parents hear the term hand foot and mouth disease, it often triggers immediate concern - and for good reason. This viral illness spreads quickly, especially among young children, and can move silently through homes, schools, and daycare centers before anyone realizes what is happening. While the condition is usually mild, understanding how it spreads and what symptoms appear at each stage can make a significant difference in controlling infection and reducing complications.
Rather than viewing hand foot and mouth disease as a sudden illness that appears overnight, it is more accurate to think of it as a process - one that unfolds in stages. Recognizing those stages early is the key to timely care, isolation, and better health outcomes.
Understanding Hand Foot and Mouth Disease and How It Begins
Hand foot and mouth disease is caused by a group of viruses known as enteroviruses, most commonly the Coxsackievirus. It primarily affects infants and children under the age of five, although adults can contract it as well - sometimes without obvious symptoms.
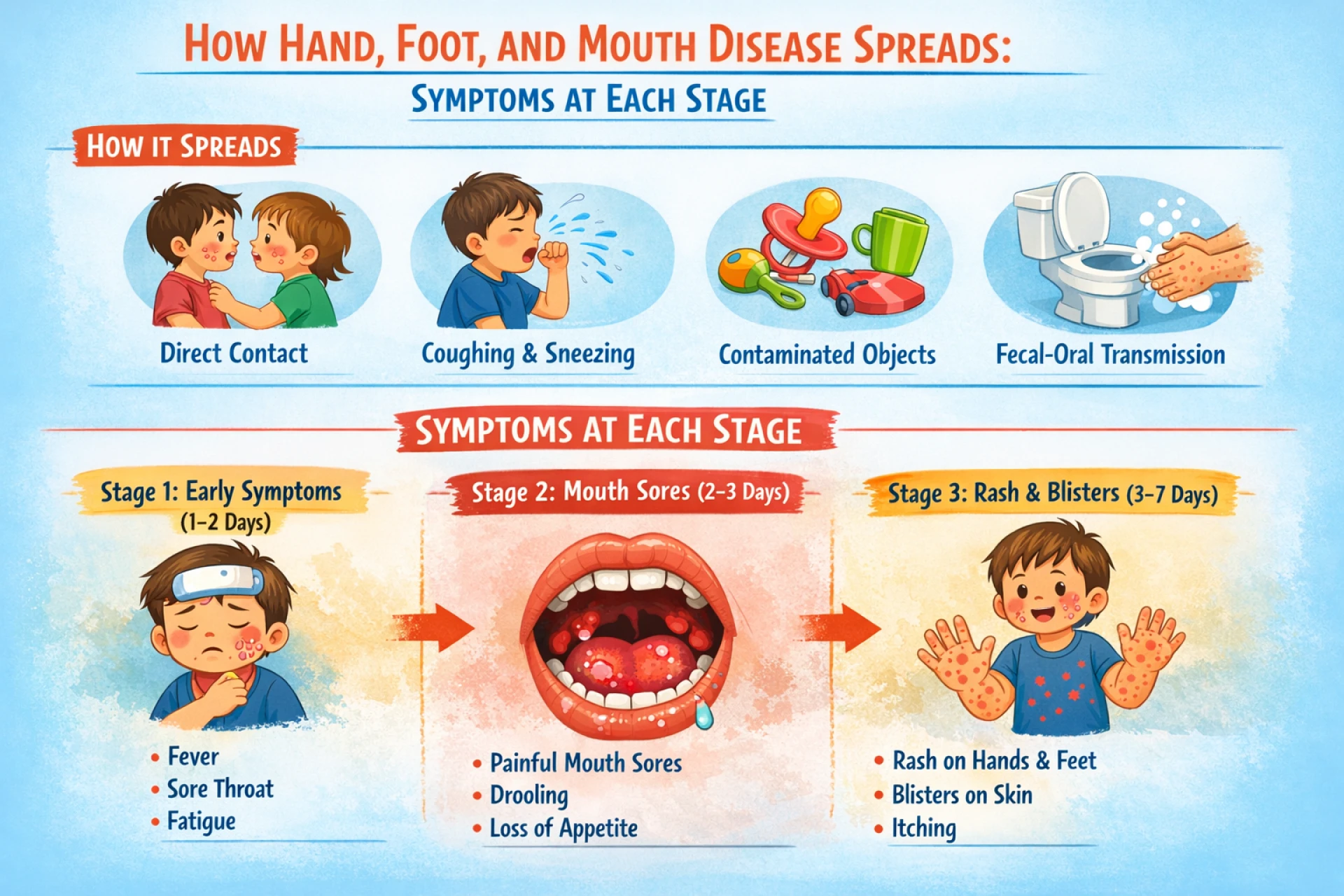
The disease spreads easily because it does not require close or prolonged contact. Simple, everyday interactions are enough. The virus can be transmitted through:
Saliva and respiratory droplets
Fluid from blisters
Nasal secretions
Stool from an infected person
This makes shared toys, unwashed hands, and contaminated surfaces major contributors to transmission. From a public health perspective, this high level of contagiousness is why awareness and preventive care are emphasized by healthcare providers and health insurance organizations alike.
Stage One: Early Exposure and Incubation Period
The first stage begins quietly. After exposure to the virus, there is an incubation period that usually lasts 3 to 6 days. During this time, the infected person may appear completely healthy while still carrying the virus.
This stage is particularly concerning because children may continue attending school or daycare, unknowingly spreading the virus to others. There are typically no visible symptoms at this point, which makes prevention difficult without good hygiene practices.
From a Health Insurance perspective, early detection and education play a crucial role in minimizing outbreaks and reducing unnecessary medical visits later.
Stage Two: Early Symptoms That Often Go Unnoticed
The second stage marks the beginning of symptoms, which are often mild and mistaken for a common viral illness. These early signs may include:
Low-grade fever
Sore throat
Fatigue
Reduced appetite
Mild headache
At this stage, hand foot and mouth disease is already contagious. Because the symptoms resemble a cold or flu, children may still attend school, increasing the risk of spreading the infection further.
This is why health professionals stress staying alert to symptom patterns rather than isolated signs. Acting early can prevent complications and limit transmission within households.
Stage Three: Visible Signs on Hands, Feet, and Mouth
The third stage is when hand foot and mouth disease becomes more recognizable. This is the phase most people associate with the condition.
Symptoms typically include:
Painful sores or ulcers inside the mouth
Red rashes or blisters on the palms of the hands
Blisters or spots on the soles of the feet
Occasionally, rashes on knees, elbows, or buttocks
These sores can make eating and drinking uncomfortable, especially for young children, increasing the risk of dehydration. While this stage may look alarming, it is often the point at which diagnosis becomes clearer and appropriate care can begin.
At this phase, medical guidance - often covered under preventive Health Insurance plans - helps ensure proper symptom management and monitoring.
Stage Four: Recovery and Continued Contagious Risk
As the blisters begin to heal, symptoms gradually fade over 7 to 10 days. Fever subsides, appetite improves, and energy levels return to normal.
However, this stage comes with a common misunderstanding: even after visible symptoms disappear, the virus can remain in the body - particularly in stool - for several weeks. This means individuals can still spread hand foot and mouth disease even after they appear fully recovered.
Good hygiene practices, such as thorough handwashing and surface disinfection, remain essential well beyond visible recovery.
Why Understanding the Spread Matters for Families and Caregivers
Knowing how hand foot and mouth disease spreads is not about fear - it is about preparedness. When families understand each stage, they are better equipped to:
Isolate infected individuals early
Prevent reinfection within households
Protect vulnerable family members
Avoid unnecessary complications
From a broader perspective, informed prevention reduces healthcare strain and supports long-term wellness goals - values that align closely with the preventive focus of Health Insurance providers.
Prevention, Awareness, and Long-Term Health Planning
There is no specific cure for hand foot and mouth disease, but prevention remains highly effective. Simple habits such as frequent handwashing, disinfecting shared surfaces, and avoiding close contact during illness significantly reduce transmission.
Health Insurance coverage that emphasizes preventive care and health education plays an important role in supporting families through such common childhood illnesses - ensuring access to guidance, consultations, and follow-up when needed.
Conclusion
Hand foot and mouth disease is a highly contagious but generally manageable illness when understood correctly. By recognizing how it spreads and identifying symptoms at each stage, families can take timely action that protects both individual and community health.
Awareness, hygiene, and early response form the strongest defense. When combined with informed healthcare support and Health Insurance coverage focused on prevention, these steps help turn a common viral illness into a manageable - and far less disruptive - experience.






Sign in to leave a comment.