Why Feedback Matters So Much in Oncology Care
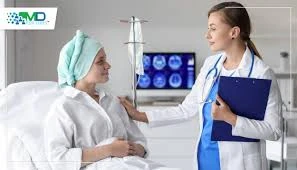
Cancer care is deeply personal. When patients face a diagnosis, they trust their oncologist not only with their health—but with their hopes, fears, and future. In that fragile space, understanding patient experiences becomes more than just “how satisfied are you?” It becomes a way to ensure care is compassionate, clear, and tailored to real needs. Listening to patients can transform cancer treatment into a more human, patient-centered journey.
How Oncologist Surveys Bridge the Gap Between Patients and Providers
Oncologist Surveys provide a structured yet empathetic way for patients to voice what truly matters to them: how well treatment side-effects were explained, whether their concerns were heard, how comfortable they felt in consultations, and whether follow-up care met their expectations. These surveys give oncologists valuable insight into patient experiences—helping them to improve communication, trust, and the overall quality of care. When patients are asked the right questions and feel that their feedback leads to real change, they are more likely to feel respected and supported throughout their cancer journey.
Real-World Impact: How Oncology Clinics Benefit from Patient Feedback
Imagine a cancer center where patients frequently mention confusion about treatment timelines, or uncertainty about how to manage side-effects at home. Without feedback, oncologists may assume that instructions are clear, but deep down patients are silently struggling. Once the clinic introduces a thoughtful survey, patterns begin to emerge: many patients want a follow-up call after chemotherapy, others feel frightened by the lack of clear written guidance, and some believe psychological support is not easily accessible. By acting on this feedback, the oncology team sets up post-treatment check-ins, distributes plain-language care guides, and strengthens their psychosocial support program. Over time, patients report reduced anxiety, better understanding, and a greater sense of being cared for — not just as patients, but as whole individuals.
Key Areas Where Oncologist Surveys Make a Big Difference
- Communication About Treatment & Side-Effects
- Oncologists often explain complex regimens and risks. Surveys help assess whether patients truly understood their options, the potential side-effects, and how to manage them.
- Emotional & Psychological Support
- Cancer is not just a physical disease; it impacts mental health deeply. Surveys can highlight patients’ emotional needs — whether they feel supported, whether they have space to talk, and how accessible counseling services are.
- Care Coordination & Follow-up
- Treatment often involves multiple specialists. Feedback from surveys can identify whether patients feel their care is well coordinated, whether they know who to contact for questions, and whether follow-up appointments are timely.
- Treatment Experience
- Patients may comment on how they feel during treatment sessions: the comfort of the space, the kindness of staff, the clarity of instructions, and the responsiveness to concerns. These insights guide improvements in the clinic environment and patient interaction.
- Patient Empowerment
- When patients feel heard, they become partners in their care. Surveys that ask how much patients feel involved in decision-making can encourage more shared decision-making and respect for patient autonomy.
Best Practices for Running Effective Oncology Surveys
- Be Sensitive & Respectful: Recognize that cancer patients may be emotionally vulnerable; use gentle, respectful language and provide options to skip uncomfortable questions.
- Keep It Manageable: A survey with 8–12 thoughtful questions is more likely to be completed than a long questionnaire.
- Offer Multiple Formats: Distribute the survey via paper, email, tablet in the clinic, or via secure patient portals to accommodate different patient preferences.
- Ensure Anonymity & Confidentiality: Patients are more open when they trust their responses remain private.
- Act on Feedback & Close the Loop: After collecting data, the oncology team should identify actionable insights and implement changes. Then, communicate back to patients about improvements made — this “you said, we did” cycle builds stronger trust.
Overcoming Challenges in Oncology Survey Programs
It’s natural for a cancer clinic to worry that patients may feel burdened by the survey or may not respond. To tackle this, staff can gently introduce the survey during routine visits and reassure patients that their feedback is voluntary and confidential. Assigning a dedicated team or staff member to manage survey implementation, collect responses, and drive follow-up ensures that the feedback doesn’t just sit in a report — it sparks real improvement.
Conclusion
Oncologist Surveys are much more than data collection tools — they are a heartfelt conversation between patients and their cancer care team. When oncologists actively listen, reflect on patient feedback, and make meaningful changes, they don’t just treat the disease — they honor the person behind it. By embracing patient-centered feedback, oncology practices can become safer, more compassionate, and more effective at guiding people through some of life’s toughest moments.















Sign in to leave a comment.