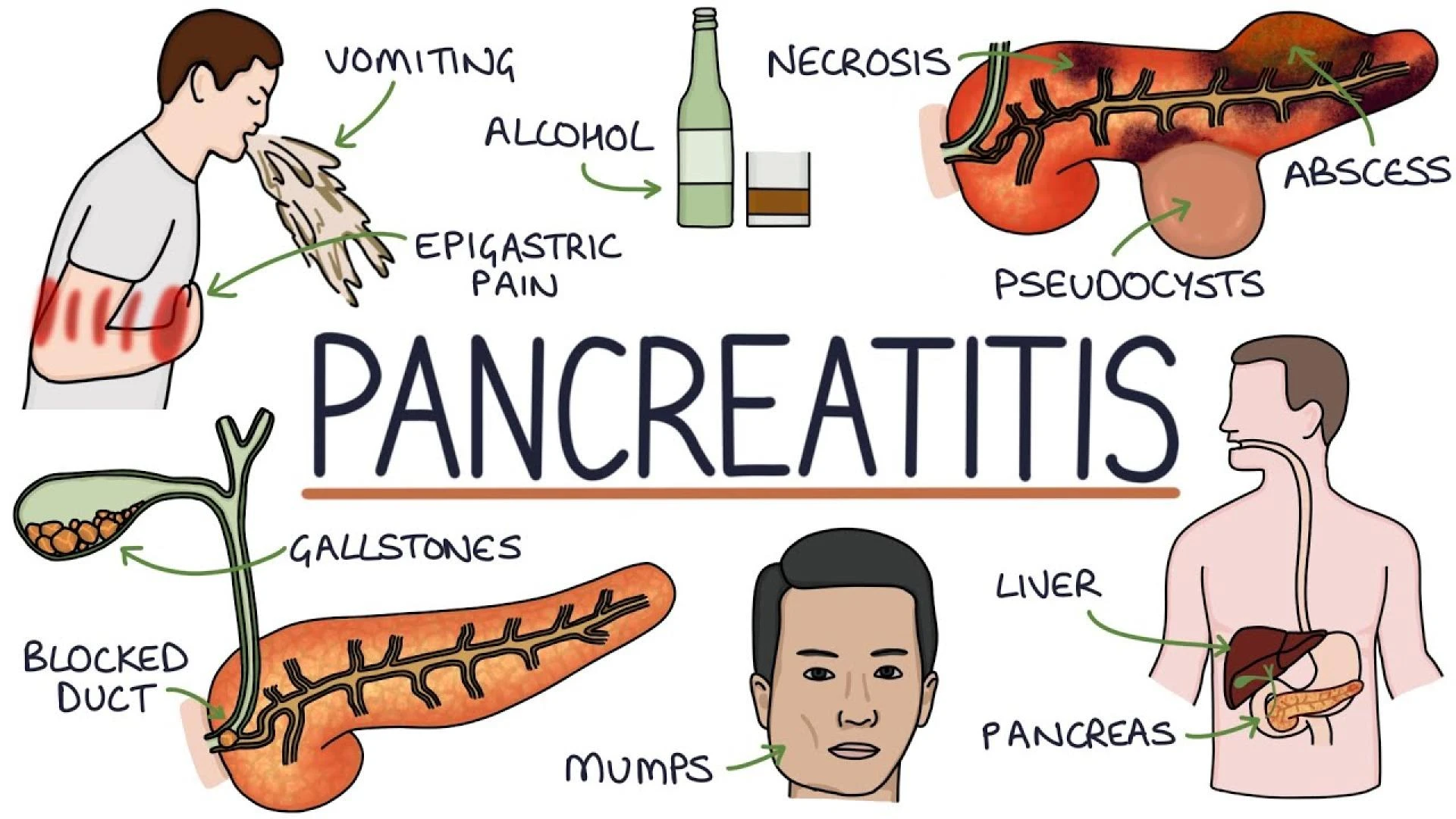
The pancreas is a part of the digestive system and a vital organ that produces digestive enzymes and insulin to regulate blood sugar levels. Pancreatitis is a condition that occurs when the pancreas becomes inflamed. It could be due to numerous reasons, including excessive alcohol consumption, gallstones, high triglycerides, or some medications. Pancreatitis may be acute or chronic. In both cases, it may take a toll on your overall health.
Acute pancreatitis occurs when the pancreas becomes inflamed suddenly. Under this type, the symptoms are easy to notice and may cause you discomfort. The severity of symptoms depends on the cause of inflammation. Chronic pancreatitis occurs when the pancreas gets inflamed over a long time. Under this type, the symptoms develop slowly and damage the pancreas over time.
What are the Signs of Pancreatitis?
It is vital to be watchful of the following signs and symptoms and seek medical care before they worsen.
Persistent Abdominal Pain
One of the most common signs of pancreatitis is persistent abdominal pain. You may experience constant pain in your upper abdomen. The pain starts mildly and becomes severe and persistent over time. It may radiate to the back or worsen after eating. Unlike a common stomachache, the pain doesn’t go away easily.
Nausea and Vomiting
People with acute or chronic pancreatitis often experience nausea and vomiting. Even after vomiting, the discomfort persists, and you feel slightly uncomfortable, especially after eating anything.
Loss of Appetite
Pancreatitis also causes loss of appetite or unintentional weight loss. Inflammation affects digestion, leading to rapid weight loss. It may happen due to difficulty digesting food properly. It occurs because the pancreas is unable to produce enough enzymes to break down fats and nutrients. Get yourself checked when you feel your appetite has changed or you are losing weight unintentionally.
Fever and Chills
In some cases of pancreatitis, the above-listed symptoms are accompanied by low-grade fever, which may indicate infection or inflammation. Do not ignore this symptom and visit a gastroenterologist for the diagnosis.
Bloating and Indigestion
Many patients with pancreatitis experience abdominal bloating, gas, and indigestion. It happens due to the inability of the pancreas to digest the food properly.
Jaundice
Another common symptom of acute pancreatitis is the yellowing of the skin or eyes, also known as jaundice. This yellowing of the skin and eyes is also accompanied by dark urine.
Foul-Smelling Stools
When the pancreas is unable to produce enough enzymes, the digestion of fat is impaired. It may result in pale, greasy, and foul-smelling stools. You should take persistent changes in the stool seriously and visit a doctor for further investigation.
What Happens if Pancreatitis is Left Untreated?
Pancreatitis is a serious condition, and it should not be left untreated; otherwise, it may become life-threatening.
- Leaving pancreatitis untreated may lead to pancreatic necrosis. It occurs when a part of the pancreas dies permanently due to severe inflammation, leading to infections.
- Not getting treated for this condition may lead to infections, cysts, or fluid collections, which may require drainage or surgery.
- Severe pancreatitis may lead to complications in other organs like the lungs, kidneys, or heart, causing organ failure.
- Chronic pancreatitis may potentially damage insulin-producing cells, resulting in diabetes.
- Chronic inflammation in the pancreas may increase your risk of developing pancreatic cancer.
When to Seek Help from a Doctor?
If you experience persistent abdominal pain or the combination of the symptoms mentioned above, you must seek immediate medical attention. Any delay in the treatment may lead to further complications. A gastroenterologist is an expert who will check your symptoms, discuss your health history, and suggest suitable treatment options after ordering the following tests:
- Blood tests to check for elevated pancreatic enzymes.
- Imaging tests, such as a CT scan, MRI, or ultrasound, are used to assess pancreatic inflammation.
- Endoscopic ultrasound to check for duct blockages or gallstones.
- Stool tests to check for malabsorption in case of chronic pancreatitis.
What are the Treatment Options for Pancreatitis?
The treatment for pancreatitis depends on its type, severity, and the underlying cause. Based on your health history and the above-mentioned factors, the gastroenterologist will suggest one of the following options:
- Hospitalization for close monitoring, especially in moderate to severe cases of pancreatitis
- Intravenous fluids to prevent dehydration
- Pain management to reduce abdominal discomfort
- Temporary fasting to allow the pancreas to rest
- Enzyme supplements to improve digestion in chronic cases of pancreatitis
- Antibiotics in case of infection
- Surgical or endoscopic procedure upon the identification of duct blockages or gallstones.
Recovery and Lifestyle Changes
The treatment of pancreatitis also includes lifestyle changes to ensure smooth long-term healing. If you are recovering from pancreatitis, you must focus on the following lifestyle changes.
- Consumption of a low-calorie, nutritious diet to support digestion
- Reducing or quitting alcohol can help reduce stress levels in the pancreas
- Quitting smoking to reduce inflammation
- Maintaining a healthy weight to support metabolic activities
- Staying hydrated to aid digestive functions
- Attending regular follow-ups to monitor problems and management of symptoms in the long term.
Takeaway
Most patients with pancreatitis can gradually return to normal activities while maintaining long-term digestive health under professional health supervision. Be watchful of your symptoms and contact the doctor immediately upon experiencing them.














Sign in to leave a comment.