In recent years, the healthcare industry has witnessed a revolutionary transformation with the integration of digital technology. Among these innovations, Telemedicine ICU has emerged as a powerful tool, allowing critical care specialists to monitor patients remotely and provide timely interventions. Organizations like NIAC are at the forefront of implementing tele-ICU solutions, bridging gaps in care, and improving patient outcomes across hospitals worldwide.
How Telemedicine ICU Enhances Critical Care with Remote Monitoring Solutions
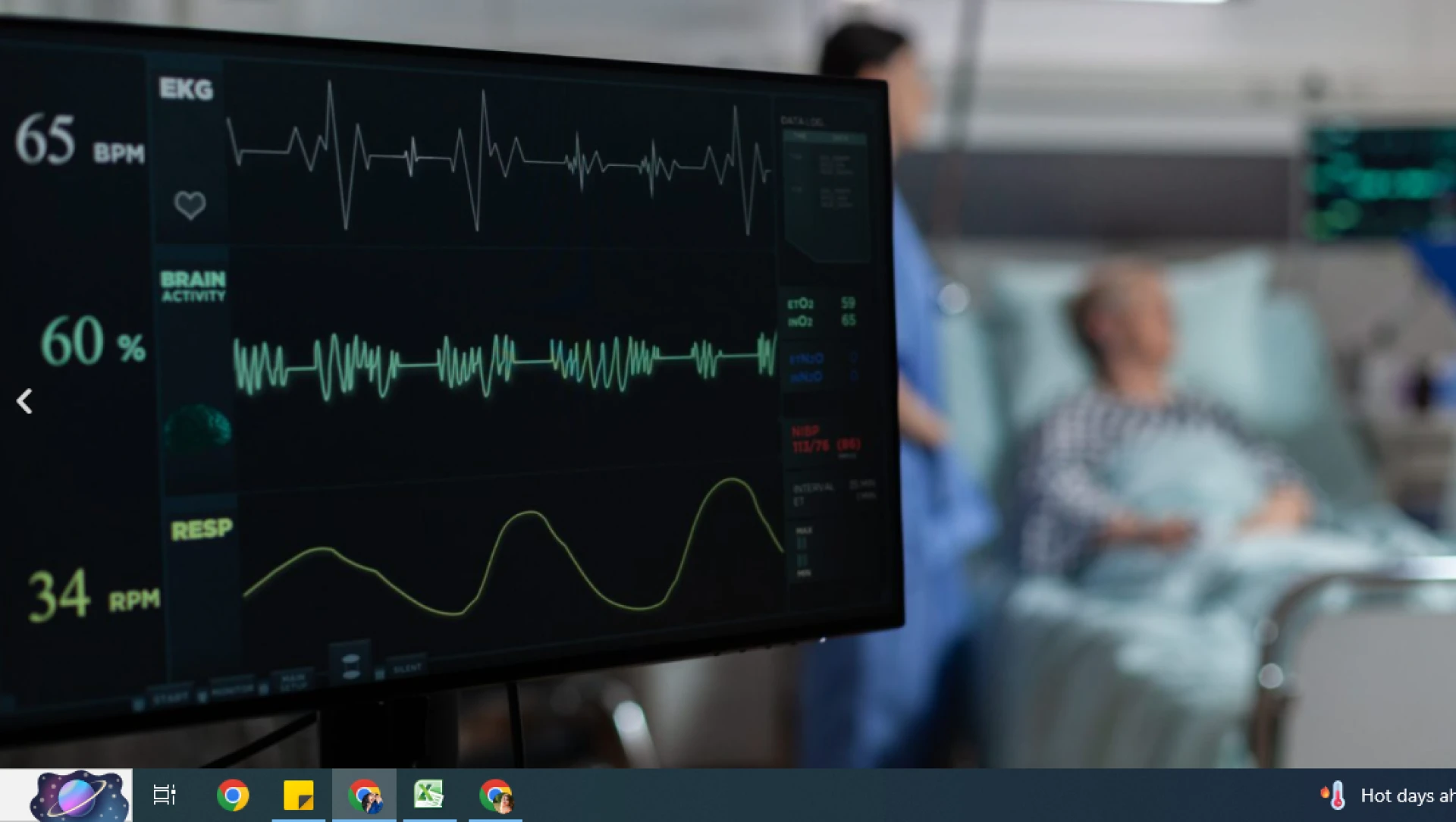
A Telemedicine ICU (Intensive Care Unit) leverages advanced digital platforms, real-time data analytics, and continuous remote monitoring to ensure that patients in critical condition receive the best possible care. This system connects bedside ICU teams with remote critical care specialists, enabling collaborative decision-making even when experts are not physically present in the hospital.
Some of the key long-tail benefits of Telemedicine ICU include:
- Continuous 24/7 monitoring – Remote specialists can track vital signs, lab results, and ventilator settings round the clock.
- Rapid intervention for critical events – Alerts and real-time notifications allow immediate medical action, reducing mortality rates.
- Enhanced resource management – Hospitals can utilize specialists across multiple ICUs, improving coverage in underserved or rural areas.
- Data-driven decision-making – AI and analytics provide predictive insights, helping anticipate patient deterioration before it occurs.
NIAC’s Telemedicine ICU Model: Transforming Patient Care
NIAC has been a pioneer in integrating tele-ICU solutions that focus on improving outcomes for critically ill patients. By combining technology with expert clinical oversight, NIAC’s Telemedicine ICU model enables:
- Collaborative care teams: Remote intensivists work alongside bedside nurses and doctors, ensuring every decision is informed by specialist insight.
- Reduced ICU length of stay: Timely interventions prevent complications, helping patients recover faster.
- Improved patient safety: Continuous monitoring reduces errors, medication issues, and adverse events.
- Access to expert care in remote areas: Smaller hospitals benefit from specialist consultations without the need for patient transfers.
Advantages of Telemedicine ICU for Hospitals and Patients
Implementing Telemedicine ICU systems has proven advantages for both healthcare providers and patients. Hospitals experience enhanced efficiency, while patients receive timely, high-quality care. Key advantages include:
- Scalable monitoring – One remote team can manage multiple ICUs across different facilities.
- Cost-effective care – Reduces unnecessary ICU admissions and transfers.
- Enhanced patient satisfaction – Continuous oversight and timely interventions lead to better recovery experiences.
- Support for clinicians – Reduces burnout by distributing workload and offering expert guidance when needed.
Future of Critical Care with Telemedicine ICU
The future of intensive care is closely tied to telemedicine. With innovations in AI, machine learning, and IoT-enabled devices, Telemedicine ICU will continue to evolve. Hospitals partnering with NIAC are already seeing measurable improvements in patient outcomes, including lower mortality rates, shorter ICU stays, and higher satisfaction scores.
Conclusion
In conclusion, Telemedicine ICU represents a paradigm shift in the way critical care is delivered. By harnessing remote monitoring technology, continuous data analysis, and expert collaboration, it ensures that patients receive timely and effective interventions regardless of location. Organizations like NIAC are leading the charge, demonstrating that integrating tele-ICU solutions not only enhances operational efficiency for hospitals but, most importantly, saves lives. As healthcare continues to evolve, Telemedicine ICU will play an increasingly vital role in improving patient outcomes and shaping the future of critical care.














Sign in to leave a comment.