In recent years, implant dentistry has revolutionised the way we approach tooth replacement. Dental implants provide a durable and aesthetically pleasing solution for individuals with missing teeth. However, the success of implant dentistry is intrinsically linked to the health and density of the underlying bone. Understanding the connection between bone health and implant dentistry is crucial for anyone considering dental implants and can significantly influence the overall success of the procedure.
What Are Dental Implants?
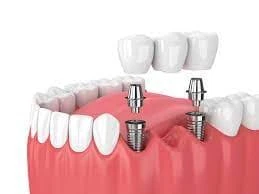
Dental implants are artificial tooth roots made from biocompatible materials, typically titanium. They are surgically placed into the jawbone to provide a stable foundation for replacement teeth, such as crowns, bridges, or dentures. The process involves several stages, starting with the surgical placement of the implant, followed by a healing period where the implant fuses with the bone through a process known as osseointegration.
This integration is a critical factor in the longevity and functionality of dental implants. A strong bond between the implant and the jawbone ensures that the replacement teeth can withstand the forces of chewing and biting, providing a natural feel and appearance.
The Role of Bone Health in Implant Success
The health of the jawbone is perhaps the most significant factor influencing the success of implant dentistry. Adequate bone density and volume are essential for securely anchoring the implant. If the bone is too thin or weak, it may not provide the necessary support, leading to implant failure.
Bone Quality and Density
Bone quality refers to the structural integrity of the bone, while density refers to the amount of mineral content within the bone tissue. Both factors play a vital role in determining whether a patient is a suitable candidate for dental implants. A thorough evaluation of bone health typically involves dental imaging techniques, such as X-rays or 3D scans, which allow dentists to assess the condition of the bone before proceeding with the implant procedure.
Patients with conditions such as osteoporosis, which leads to decreased bone density, may face challenges with implant placement. In such cases, dentists may recommend additional procedures to enhance bone health before implants can be successfully placed.
Bone Loss and Its Causes
Bone loss in the jaw can occur for several reasons, including:
- Tooth Loss: When a tooth is lost, the bone that once supported it begins to deteriorate due to a lack of stimulation. The roots of natural teeth provide necessary mechanical stress to the bone, promoting its health and density. Without this stimulation, the bone can resorb, leading to diminished volume and quality.
- Periodontal Disease: Gum disease can cause inflammation and infection in the supporting structures of the teeth, leading to bone loss around the teeth. Patients with a history of periodontal disease may have compromised bone health, making implant placement more complex.
- Medical Conditions: Certain medical conditions, such as diabetes, can impair bone healing and density. Additionally, hormonal changes, particularly in postmenopausal women, can lead to increased bone loss.
- Lifestyle Factors: Smoking and excessive alcohol consumption can negatively impact bone health, reducing the chances of successful osseointegration. These habits can also impair blood flow and healing, further complicating the implant process.
Assessing Bone Health Before Implant Placement
Before proceeding with implant dentistry, a thorough assessment of bone health is essential. Dentists will typically conduct a comprehensive evaluation that includes:
- Medical History Review: Understanding a patient's medical history, including any conditions that may affect bone health, is crucial for determining candidacy for dental implants.
- Dental Imaging: Advanced imaging techniques, such as Cone Beam Computed Tomography (CBCT), can provide detailed information about the bone's structure, allowing dentists to visualise the quality and quantity of available bone.
- Clinical Examination: A thorough clinical examination will assess gum health, existing teeth, and any signs of periodontal disease that may impact bone health.
Based on this assessment, dentists can develop a tailored treatment plan that may include bone grafting or other procedures to improve bone health if necessary.
Bone Grafting Procedures
For patients with insufficient bone density, bone grafting procedures can be an effective solution. Bone grafting involves the surgical placement of bone material—either from the patient (autograft), from a donor (allograft), or synthetic materials—into the area where bone density is lacking. This procedure aims to stimulate new bone growth, creating a solid foundation for the dental implant.
Types of Bone Grafts
- Autograft: This type of graft uses bone harvested from another area of the patient's body, such as the hip or chin. Autografts typically have a higher success rate due to the use of the patient's own living tissue.
- Allograft: An allograft involves using bone from a deceased donor, which is processed and sterilised to ensure safety. This option is often more convenient and less invasive than harvesting bone from the patient's body.
- Synthetic Grafts: Biocompatible materials can also be used to promote bone growth. These synthetic grafts provide a scaffold for new bone to develop, and they are increasingly popular due to their effectiveness and lower risk of complications.
Healing and Integration
After a bone grafting procedure, a healing period is necessary for new bone to form and integrate with the existing bone. This process can take several months, during which the dentist will monitor progress through follow-up appointments and imaging.
Once sufficient bone density is achieved, the dentist can proceed with the placement of dental implants, ensuring a solid foundation for long-term success.
Maintaining Bone Health After Implant Placement
Once dental implants are successfully placed, maintaining bone health is critical for the longevity of the implants. Patients should adopt good oral hygiene practices, including:
- Regular Brushing and Flossing: Maintaining excellent oral hygiene can prevent infections and complications that could jeopardise the health of the implants and surrounding bone.
- Routine Dental Check-Ups: Regular visits to the dentist for cleanings and examinations can help identify any potential issues early on.
- Healthy Lifestyle Choices: Avoiding smoking and limiting alcohol consumption can significantly impact bone health and overall oral health.
- Balanced Diet: Consuming a diet rich in calcium and vitamin D supports bone density, promoting long-term health.
Incorporating these practices into daily life can help ensure the success of dental implants and the overall health of the jawbone.
The connection between bone health and implant dentistry cannot be overstated. Understanding the importance of bone density and quality is essential for anyone considering dental implants. With appropriate assessments, treatments, and maintenance, individuals can successfully navigate the journey of implant dentistry, leading to restored function and confidence through a beautiful smile. The advancements in dental technology and techniques continue to offer hope and solutions for those facing tooth loss, bridging the gap between health and aesthetics in dental care.
















Sign in to leave a comment.