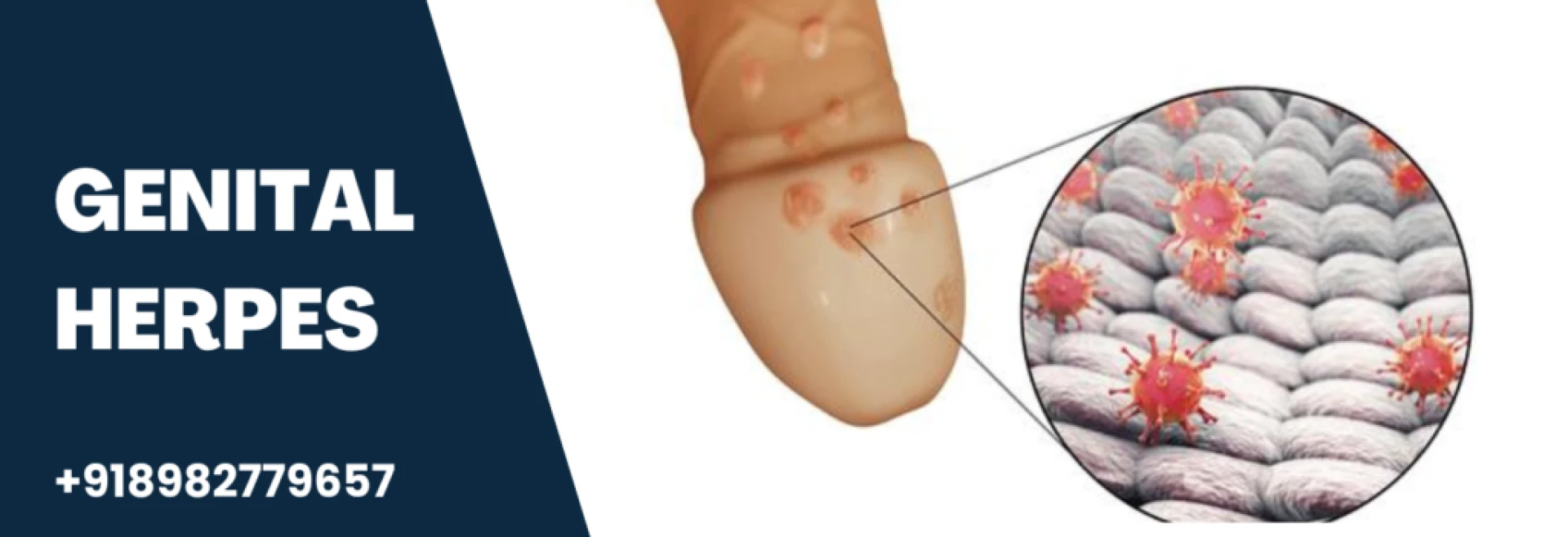
Genital herpes, a common sexually transmitted infection (STI), continues to be a source of physical discomfort and emotional distress for millions across the globe. It is primarily caused by the herpes simplex virus type 2 (HSV-2), although HSV-1—commonly associated with oral herpes—can also be a culprit in genital infections. Despite its prevalence, genital herpes is often misunderstood and stigmatized, leaving many individuals uncertain about how to manage outbreaks, reduce transmission, and live confidently. This article offers a comprehensive overview of the current treatment for genital herpes, blending scientific insight with practical advice.
Causes and Transmission
The herpes simplex virus spreads through skin-to-skin contact, typically during vaginal, anal, or oral sex. It can be transmitted even when the infected individual has no visible symptoms. Once the virus enters the body, it remains there for life, lying dormant in the nerve cells and reactivating intermittently.
Primary infections—often more severe—can occur days or weeks after exposure. These episodes may be accompanied by painful sores, flu-like symptoms, swollen lymph nodes, and general malaise. Subsequent outbreaks tend to be less intense but can still cause emotional strain and physical discomfort.
Recognizing the Symptoms
Symptoms vary from person to person. Some may remain asymptomatic, while others experience recurrent sores or blisters around the genital area, buttocks, or thighs. Warning signs before an outbreak often include tingling, itching, or pain in the affected area.
The unpredictability of flare-ups makes management a priority for those diagnosed. While there is currently no cure for herpes, several therapeutic strategies exist to control the symptoms and improve quality of life.
Antiviral Medications
The cornerstone of medical management involves antiviral therapy. These medications do not eradicate the virus but can suppress its activity.
1. Acyclovir – One of the first antivirals developed for herpes, acyclovir is available in both oral and topical forms. It shortens the duration of outbreaks and can be taken daily for suppression.
2. Valacyclovir – A more bioavailable derivative of acyclovir, it requires fewer doses and is commonly prescribed for both episodic and suppressive treatment.
3. Famciclovir – Another oral antiviral option that effectively reduces the severity and frequency of outbreaks.
Episodic Therapy is taken at the onset of symptoms to speed healing and reduce discomfort. In contrast, Suppressive Therapy involves daily medication to prevent or reduce the frequency of outbreaks and lower the risk of transmission.
Lifestyle and Home Management
Managing genital herpes effectively extends beyond prescription medication. Lifestyle changes and home care practices play a critical role in minimizing outbreaks and maintaining overall well-being.
- Stress Reduction: Emotional and physical stress are known triggers. Mindfulness, meditation, yoga, or therapy may help keep outbreaks at bay.
- Proper Hygiene: Keeping the affected area clean and dry prevents secondary infections and promotes healing.
- Avoiding Triggers: Common triggers include illness, fatigue, menstruation, and excessive sun exposure. Learning your personal triggers is key.
- Dietary Adjustments: Some individuals find relief by limiting foods high in arginine (like nuts and chocolate), which can encourage viral replication, and increasing lysine intake (found in dairy and fish).
Emotional and Psychological Support
The social stigma surrounding genital herpes can take a toll on mental health. Individuals often experience feelings of shame, guilt, or anxiety, especially when disclosing their condition to partners. Professional counseling, support groups, and open communication can ease the emotional burden.
It's important to remember that genital herpes is manageable and does not define one’s worth or relationships. Millions live healthy, fulfilling lives despite the diagnosis.
Preventing Transmission
Even with no visible sores, it’s possible to transmit the virus to others. Preventive steps include:
- Consistent Condom Use: While not foolproof, condoms reduce the risk significantly.
- Antiviral Suppression: Daily use of antivirals lowers the chance of passing the virus.
- Open Dialogue with Partners: Transparency fosters trust and mutual responsibility.
- Avoiding Sexual Contact During Outbreaks: This is when the virus is most contagious.
The Role of Medical Experts
Managing genital herpes requires a personalized approach. Regular consultations with healthcare professionals ensure the right treatment strategy is in place. This is where reputable clinics like Bestsexologist stand out, offering holistic and empathetic care tailored to individual needs. Their expertise encompasses not only the physical dimensions of STI management but also the emotional and relational aspects.
From initial diagnosis to long-term care, professional guidance ensures individuals receive the most effective support, reducing the impact of herpes on their daily lives.
Promising Research and Future Therapies
Ongoing research continues to push the boundaries of herpes treatment. New antiviral formulations, vaccines under development, and gene-editing technologies offer hope for more effective long-term management—and possibly a cure in the future.
Several therapeutic vaccines aim to reduce the frequency and severity of outbreaks. Although none are commercially available yet, clinical trials are showing encouraging results.
Gene therapy is another emerging field. Scientists are exploring ways to target and eliminate latent herpes viruses hidden within nerve cells. Though still in early stages, this could revolutionize the approach to chronic viral infections.
Conclusion
Living with genital herpes can be challenging, but with the right tools, support, and information, it becomes a manageable part of life. Today’s medical options—from antiviral medications to lifestyle strategies—offer effective solutions to control symptoms and reduce transmission risks. The shame and stigma often associated with the condition are unwarranted and counterproductive; knowledge, compassion, and self-care are key to moving forward.
By taking a proactive approach, consulting professionals like Bestsexologist, and staying informed about new developments, individuals can regain control and live confidently. Herpes is not a life sentence—it is a manageable condition, and you are not alone.
















Sign in to leave a comment.