There are some medical emergencies that announce themselves with pain — a broken bone, a heart attack, a burst appendix. You know something is seriously wrong because your body tells you loudly and unmistakably.
Retinal detachment is not one of those emergencies.
It is completely painless. It can begin so quietly that many people mistake the early signs for nothing more than tiredness or a minor visual glitch. And yet, if left untreated for even a matter of hours, it can lead to permanent, irreversible blindness.
That contrast — the silence of the condition versus the severity of the consequences — is exactly why retinal detachment is one of the most important eye emergencies to understand. Knowing what to look for could, quite literally, save your sight.
In this guide, the specialists at Skipper Eye-Q International Eye Hospital walk you through everything you need to know: what retinal detachment is, what causes it, the warning signs you must never ignore, and the treatment options available to you right here in Nigeria.
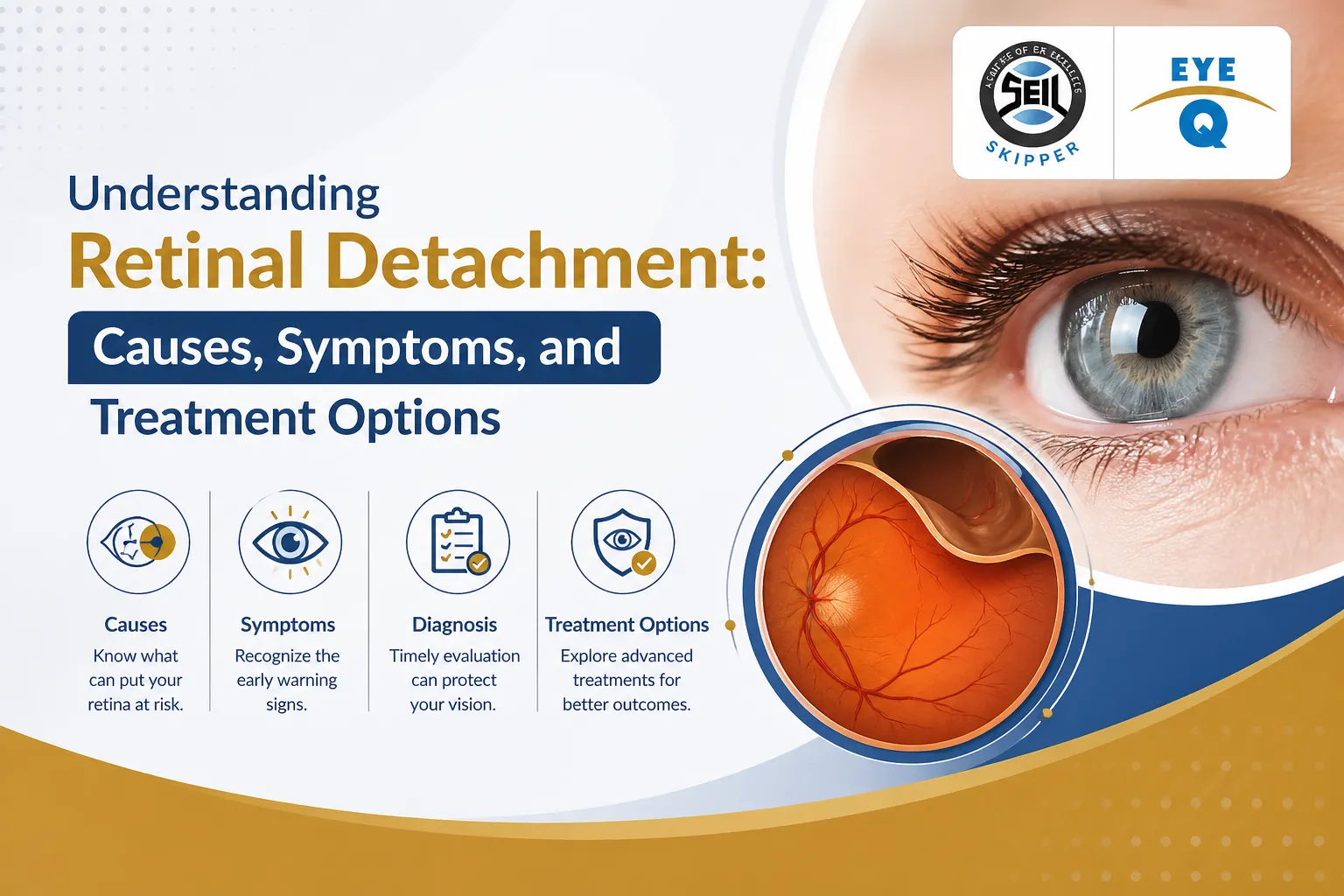
What Is Retinal Detachment?
To understand retinal detachment, it helps to understand what the retina does.
Your retina is a thin, delicate layer of light-sensitive tissue lining the inside of the back of your eye. When light enters your eye through the lens, it lands on the retina, which converts it into electrical signals and sends those signals to the brain via the optic nerve. Your brain then interprets those signals as the images you see.
In other words, the retina is your eye's film — the surface on which every image you've ever seen has been captured.
Retinal detachment happens when this layer of tissue peels away from its normal position at the back of the eye. When it detaches, it loses the blood supply and oxygen it needs to function, and the visual information it was processing is interrupted. The longer it remains detached, the greater the risk of permanent vision loss.
A helpful analogy: Think of your retina like wallpaper on a wall. When it's perfectly flat against the surface, everything looks fine. But if moisture gets behind the wallpaper and causes a bubble, it lifts away — and once it starts, it can spread further and further unless you address it quickly.
Is Retinal Detachment Common?
Retinal detachment is not an everyday occurrence, but it is far from rare. It affects approximately one to two people out of every 10,000 each year. While that sounds small, when you consider Nigeria's population of over 200 million, that translates to thousands of potential cases annually.
Treatment for retinal detachment works well, especially if the detachment is caught early. In some cases, a second treatment or surgery may be needed if the retina detaches again — but treatment is ultimately successful for about nine out of ten people.
The critical word in that sentence is early. The outcome difference between someone who acts on their symptoms immediately and someone who waits is enormous.
Three Types of Retinal Detachment
Not all retinal detachments are the same. There are three distinct types, each with different causes and slightly different considerations for treatment.
1. Rhegmatogenous Retinal Detachment (Most Common)
This is the type most people mean when they talk about retinal detachment, and it's the most common.
The most common type of retinal detachment is often due to a tear or hole in the retina. Eye fluid may leak through this opening, causing the retina to separate from the underlying tissues — much like a bubble under wallpaper. This is most often caused by a condition called posterior vitreous detachment.
As we age, the vitreous — the gel-like substance that fills the inside of the eye — gradually shrinks and liquefies. This is a normal part of ageing. But as it shrinks, it can pull on the retina, and in some cases, it creates a tear. Fluid from inside the eye then seeps through the tear and collects behind the retina, pushing it away from the back of the eye.
2. Tractional Retinal Detachment
In this type, scar tissue on the retina can pull it away from the back of the eye. Diabetes is a common cause of these retinal detachments. Extended periods of high blood sugar can damage blood vessels in the eye and cause scar tissue, which can then tug the retina away from the back of the eye.
This type is common in people with advanced diabetic retinopathy and is one of the reasons why regular eye examinations are so important for anyone living with diabetes.
3. Exudative (Serous) Retinal Detachment
This happens when fluid builds up under the retina due to inflammation, blood vessel problems, or injury. There is no hole, break, or tear in this type of retinal detachment.
This type is less common and is often associated with conditions like uveitis (inflammation inside the eye), age-related macular degeneration (wet form), or tumours affecting the eye.
What Causes Retinal Detachment?
Understanding the causes helps you assess your own risk — and know when to be extra vigilant about your eye health.
Ageing and Posterior Vitreous Detachment (PVD)
The most common cause. As the vitreous gel shrinks with age, it pulls on the retina. In most people, the vitreous separates cleanly — causing some floaters and flashes but no lasting damage. But in some cases, the pulling is strong enough to tear the retina, setting the stage for detachment.
Severe Short-Sightedness (High Myopia)
People with high myopia (nearsightedness above -6 dioptres) have longer eyeballs than average. This means the retina is stretched thinner and is more vulnerable to tears and detachment. Retinal detachment is caused by holes or tears in the retinal tissue. These occur most often due to aging, eye trauma, severe myopia, or prior eye surgeries.
If you are highly short-sighted, regular retinal check-ups are essential — not optional.
Eye Trauma or Injury
A significant blow to the eye — from a sports injury, a road accident, or any direct impact — can cause the retina to tear or detach. This is why protective eyewear during contact sports and high-risk activities is so important.
Previous Eye Surgery
Certain eye surgeries, including cataract surgery in some cases, can increase the risk of retinal detachment — particularly in people who already have other risk factors.
Diabetes
As mentioned, diabetic retinopathy — the eye complication of long-term diabetes — can lead to tractional retinal detachment through the formation of scar tissue on the retina.
Family History
A number of risk factors may increase the likelihood of developing a retinal detachment, in particular, a family history of the disorder, nearsightedness, or the occurrence of diabetes. If a close relative has had a retinal detachment, your personal risk is higher than average.
Other Eye Conditions
Conditions like lattice degeneration (areas of thinning in the peripheral retina), retinoschisis, and uveitis can all increase susceptibility to retinal detachment.
Warning Signs of Retinal Detachment: What to Look For
This section could save your vision. Please read it carefully.
Retinal detachment is painless; however, it often comes with additional symptoms that can increase in severity before the detachment occurs.
Here are the warning signs you must never ignore:
Sudden Increase in Floaters
We all see the occasional floater — those tiny specks or squiggly lines that drift across your vision. But a sudden, dramatic increase in floaters is a red flag. This sudden surge often means the vitreous is pulling on or has already torn the retina.
Flashes of Light (Photopsia)
Sudden flashes of light — especially in your peripheral (side) vision — are a classic early warning sign. These occur because the pulling or tugging of the vitreous on the retina creates a visual disturbance that your brain interprets as light.
Real-life example: Emeka, a 52-year-old accountant in Abuja, noticed flashing lights at the edge of his vision while driving home one evening. He assumed it was fatigue and went to bed. By morning, a shadow had spread across his lower visual field. When he finally visited Skipper Eye-Q, he was diagnosed with a partial retinal detachment. Fortunately, he reached the clinic in time for surgery to preserve his central vision.
A Dark Shadow or "Curtain" Across Your Vision
This is often described as a grey curtain, shadow, or veil creeping in from one side of your visual field. It typically starts at the periphery (sides) and moves inward. This shadow represents the area where the retina has already detached.
Blurred Vision
Sudden, unexplained blurring — especially in one eye — can indicate that the retina is no longer sitting properly against the back of the eye.
Reduced Peripheral Vision
A noticeable decrease in your side vision, sometimes described as "tunnel vision", can be a sign that the peripheral retina has begun to detach.
When Should You Go to the Emergency Room?
If you experience any combination of the symptoms above — especially new floaters with flashes, or a shadow spreading across your vision — do not wait. Do not wait to see if it improves overnight. Do not try to make an appointment for next week.
If you experience any symptoms of retinal detachment, go to your eye doctor or the emergency room right away. Retinal detachment can cause permanent vision loss — but getting treatment right away can help protect your vision.
Time is everything with this condition. The sooner treatment begins, the better the outcome.
How Is Retinal Detachment Diagnosed?
When you arrive at a specialist eye clinic like Skipper Eye-Q, the diagnostic process for retinal detachment involves several steps.
Diagnosing a retinal detachment involves several steps. First, patients will typically undergo a retinal exam, and if there is any bleeding in the eye, ultrasound imaging may be performed. The physician will examine both eyes, even if symptoms are only present in one. If no detachment is found, a follow-up appointment will usually be scheduled to monitor for any delayed detachment.
Diagnostic tools at Skipper Eye-Q include:
- Dilated fundus examination — the ophthalmologist uses dilating drops and specialised lenses to examine the entire retina in detail
- Optical Coherence Tomography (OCT) — produces detailed cross-sectional images of the retina to assess the extent of any detachment or fluid
- B-scan ultrasound — used when the view of the retina is obscured by bleeding or other opacity
- Fluorescein angiography — maps blood flow and can reveal areas of retinal damage
One important point: your doctor will examine both eyes, even if only one has symptoms. This is because someone who has had a retinal detachment in one eye has an increased risk in the other.
Treatment Options for Retinal Detachment
The treatment for retinal detachment depends on the type, size, and location of the detachment — and crucially, how quickly you seek help.
In some cases, laser therapy or freezing techniques can seal small retinal tears before they progress. More advanced cases may require surgical procedures, such as vitrectomy or scleral buckle, to reattach the retina and stabilise vision.
Here is a breakdown of the main options:
Treatment 1: Laser Photocoagulation (for Small Tears)
If a retinal tear is caught before significant detachment has occurred, laser treatment can seal the tear by creating small burns around it. These burns create scar tissue that acts like a weld, anchoring the retina in place and preventing fluid from passing through the tear.
This is a clinic-based procedure with minimal recovery time and excellent results when performed early.
Treatment 2: Cryopexy (Freezing Treatment)
Similar in principle to laser treatment, cryopexy uses a freezing probe applied to the outside of the eye to seal a retinal tear. Like laser treatment, it creates a scar that bonds the retina to the underlying tissue, preventing further detachment.
Treatment 3: Pneumatic Retinopexy
If you have a small detachment, your eye doctor may place a gas bubble in the eye. This is called pneumatic retinopexy. It helps the retina float back into place. The hole is sealed with a laser.
After the gas bubble is injected, the patient must maintain a specific head position for several days so the bubble presses against the correct area of the retina. As the retina reattaches and the tear is sealed, the bubble gradually dissolves on its own.
This technique is best suited for certain types of uncomplicated detachments. If you have a gas bubble in your eye, you cannot fly — the change in air pressure can cause serious complications.
Treatment 4: Scleral Buckle Surgery
In the scleral buckle procedure, a surgeon attaches a tiny flexible band of silicone rubber or sponge onto the sclera — the white of the eye. The band pushes the sides of the eye toward the retina, which helps it reattach.
This remains one of the most effective long-term surgical options, particularly for younger patients. It is performed under anaesthesia in an operating theatre and typically takes one to two hours.
The silicone band remains permanently in place around the eye — it is not visible and causes no discomfort in the vast majority of patients.
Treatment 5: Vitrectomy
Vitrectomy is the most commonly performed surgery for complex retinal detachments. During the procedure, the surgeon removes the vitreous gel from inside the eye — along with any scar tissue pulling on the retina — and replaces it with a gas bubble, silicone oil, or saline solution to hold the retina flat while it heals.
Surgery for a detached retina is typically an outpatient procedure, though vision improvement can take weeks to months. Some patients may not regain their full vision depending on how long the retina was detached and whether central vision was affected.
At Skipper Eye-Q, vitrectomy procedures are performed using state-of-the-art microincisional surgical technology by our experienced vitreoretinal surgeons — providing world-class care without the need to travel abroad.
Recovery After Retinal Detachment Surgery
Recovery varies depending on the procedure performed, but here is what most patients can expect:
- First few weeks: Some redness, discomfort, and blurred vision are normal. Your surgeon will prescribe eye drops to prevent infection and reduce inflammation.
- Positioning: If a gas bubble was used (in pneumatic retinopexy or vitrectomy), you will need to maintain a specific head position for several days — usually face-down. This is essential for the bubble to press correctly against the repaired area.
- Driving: You cannot drive until your vision has adequately recovered and your surgeon gives you clearance.
- Flying: Not permitted while a gas bubble is in your eye — sometimes for several weeks.
- Full visual recovery: This can take three to six months, sometimes longer. Be patient with the process.
The most important thing to know about recovery is this: if surgery is performed before central vision is lost, surgeons can reattach the retina to the back of the eye and preserve eyesight. However, if central vision is already lost, surgical results are less favourable — and scar tissue that develops over time makes surgery harder to perform.
Can Retinal Detachment Be Prevented?
Not always — particularly when it is caused by ageing or genetic factors. But there are practical steps that significantly reduce your risk:
1. Get Regular Eye Examinations Comprehensive dilated eye exams can help your eye doctor find a small retinal tear or detachment early, before it starts to affect your vision. If you're over 40, or have any of the risk factors mentioned above, annual dilated eye exams are essential.
2. Wear Protective Eyewear If you play contact sports, use power tools, or work in environments with flying debris, wear appropriate protective eyewear. A single preventable eye injury is all it takes.
3. Control Your Blood Sugar (If You Have Diabetes) Keeping blood glucose levels well-controlled dramatically reduces the risk of diabetic retinopathy progressing to the point of tractional retinal detachment.
4. Know Your Risk Factors If you are highly myopic, have a family history of retinal detachment, or have had a previous detachment in one eye, make sure your ophthalmologist knows. More frequent monitoring can catch problems before they become emergencies.
5. Act Immediately on New Symptoms If you notice a sudden increase in floaters or new flashes of light — even if you feel fine otherwise — call your eye clinic the same day. This cannot be overstated.
Why Choose Skipper Eye-Q for Retinal Detachment Care?
At Skipper Eye-Q International Eye Hospital, we have built our reputation on one thing: delivering world-class eye care to patients in Nigeria without the need to travel abroad.
Our vitreoretinal team is experienced in managing the full spectrum of retinal conditions — from early retinal tears treated with laser, through to complex vitrectomy surgery for advanced detachments.
What we offer:
- Emergency retinal assessments — same-day appointments available for urgent cases
- State-of-the-art diagnostic equipment: OCT, ultrasound, wide-field retinal imaging
- Laser photocoagulation and cryopexy for retinal tears
- Pneumatic retinopexy, scleral buckle, and vitrectomy surgery
- Post-operative care and long-term retinal monitoring
- Locations in Lagos and Abuja, HMO-empanelled for corporate and insurance patients
Get in touch: 📍 Victoria Island Lagos 📍 Abuja 📍 Gwarinpa📍 Ilupeju Lagos 📍 📧 [email protected]
Conclusion: Time Is the One Thing You Cannot Get Back
Retinal detachment doesn't give you a warning loud enough to make you panic. It creeps in quietly — a few extra floaters, a flash of light at the edge of your vision, a shadow that seems to grow.
That quietness is the danger.
By the time many people realise something is seriously wrong, irreversible damage has already been done to their vision. But the stories with the best endings are always the same: someone noticed something unusual, acted immediately, and walked out of surgery with their sight intact.
If there is one thing to take away from this guide, it is this: don't wait. If you see sudden floaters, flashes, or any shadow in your vision, treat it as the emergency it is. Call Skipper Eye-Q, go to the nearest eye hospital, or go to an emergency room.
Your retina — and the vision it gives you — is worth protecting with everything you have.














Sign in to leave a comment.