Dental infections can start small and stay local. Or they can grow, cause major pain, and very rarely travel to the brain. This article explains how dental infections start, what raises the risk, how dentists treat them, when antibiotics like zylomox 500mg capsules are used, and what signs mean the infection may be spreading. If you have symptoms now, please contact a dentist or doctor.
How dental infections begin
Most dental infections begin inside a tooth or around the gum. The two common starting points are:
- A dead or damaged nerve inside a tooth. Bacteria enter the pulp (the soft tissue inside) and cause a periapical abscess. This is the classic “tooth abscess.”
- Gum disease or a pocket around the tooth. Bacteria gather and cause a periodontal abscess.
Poor oral hygiene, deep tooth decay, cracked teeth, failed root canals, and smoking raise the chance of infection. Implants can also become infected if bacteria colonize the area around the implant; this is called peri-implantitis and is one cause of dental implants infections.
Signs and symptoms to watch for
Common signs of a dental infection:
- Sharp or throbbing tooth pain that may be constant.
- Swelling of the gum, cheek, or face.
- A pimple-like bump on the gum that may drain pus.
- Bad taste in the mouth or bad breath.
- Fever, feeling unwell, or swollen lymph nodes (in worse cases).
If swelling is large or affects breathing, swallowing, or speech, treat it as an emergency.
Root canals, implants, and infection — the specifics
Root canals: When a tooth nerve is infected, a dentist often performs a root canal to remove the infected tissue and seal the tooth. This usually stops the infection if done well. However, root canal-treated teeth can fail. A failed treatment can lead to renewed infection that may require retreatment or extraction.
Implants: Dental implants can fail when the surrounding bone or gum becomes infected. Implant infections can be stubborn. Early detection and cleaning around the implant can save it. In advanced cases, the implant may need removal.
How dentists treat dental infections
The first goal is to remove the source of infection. That may mean:
- Draining a pus pocket.
- Performing or redoing a root canal to clear infected pulp.
- Extracting the tooth, if it can’t be saved.
- Cleaning around an infected implant, and sometimes removing the implant.
Antibiotics are an adjunct — they help when the infection is spreading, when there is systemic illness (fever), or when the patient has a weak immune system. Local surgical care (drainage, root canal, extraction) is usually the definitive step. Repeated courses of antibiotics without drainage are not usually effective. This principle is emphasized in UK dental guidance.
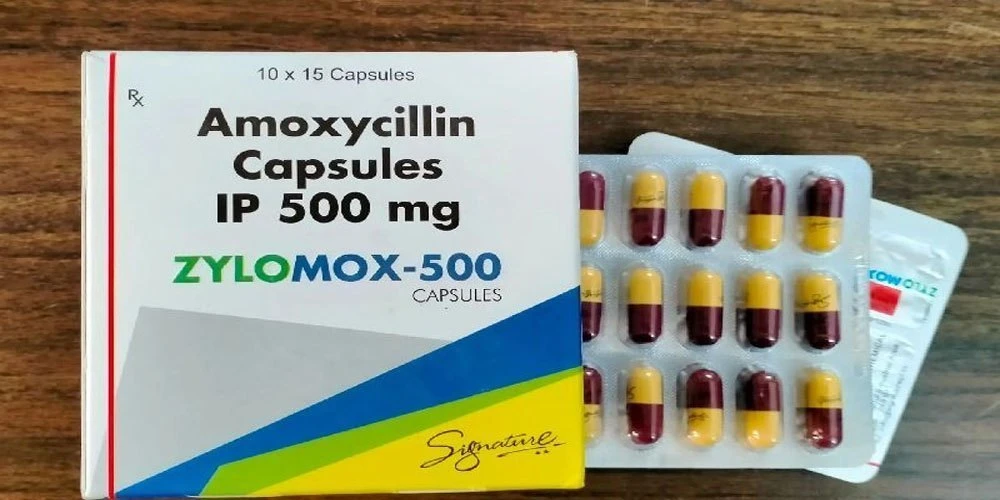
When are antibiotics like zylomox 500mg capsules used?
Zylomox capsules of 500mg is a brand of amoxicillin, a common penicillin-type antibiotic used for many bacterial infections. Amoxicillin is frequently a first-line choice for dental infections when an antibiotic is needed. However, it should be prescribed by a clinician who has examined you. Never self-prescribe.
Key points about antibiotic use in dental infections:
- Antibiotics are recommended when the infection shows signs of spreading beyond the tooth or gums, or if the patient shows systemic symptoms (fever, malaise), or has major health risks. Otherwise, local dental treatment is the main action.
- Amoxicillin is listed on official FDA drug labeling as an approved treatment for infections caused by susceptible bacteria; dosing, interactions, and safety details are in the FDA label. Clinicians consult that label when prescribing.
If you are prescribed zylomox capsules of 500mg (amoxicillin), take the full course. Stopping early can let bacteria survive and become resistant. Report any allergic reactions (rash, breathing trouble) immediately.
Can a dental infection spread to the brain?
Yes — but it is rare. The mouth sits close to the sinuses, neck spaces, and the skull base. In some cases, bacteria from an oral infection can travel to nearby tissues and then reach the skull or brain. When this happens, it can cause a brain abscess or intracranial infection. These are serious, life-threatening conditions that need urgent hospital care.
Medical literature and reviews document cases where oral bacteria caused brain abscesses. Although rare, the connection exists and is more likely if the dental infection is untreated, if the person has weakened immunity, or if the infection spreads through deep neck spaces.
What are warning signs of a spreading infection?
If a dental infection starts spreading, you may see:
- High fever or chills.
- Increasing facial or neck swelling.
- Severe headache, confusion, or changes in alertness.
- Trouble breathing or swallowing.
- Stiff neck, visual changes, or seizures (these may suggest intracranial spread).
If you have these signs, go to emergency care right away.
How doctors diagnose a spreading infection
Doctors and dentists use:
- Clinical exam (look and feel).
- Imaging: dental X-rays, panoramic X-ray, CT scan of head/neck, or MRI if brain involvement is suspected.
- Blood tests to look for infection markers.
- If a brain abscess is suspected, neurosurgery and infectious disease specialists are involved. Cultures from drained pus help pick the best antibiotic.
MedlinePlus and NCBI summaries explain how brain abscess presents and is diagnosed.
Treatment of dental infections that reach deep spaces or brain
When a dental infection spreads beyond the tooth:
- Hospital care may be needed.
- IV antibiotics that cross into the brain may be used. Treatment is guided by cultures and local resistance patterns.
- Surgical drainage is often required for deep neck infections and brain abscesses. Neurosurgeons may drain brain abscesses.
- The origin tooth or implant still needs definitive dental care after stabilization (root canal, extraction, implant removal).
Outcomes are much better when care is prompt.
Prevention — what you can do
Simple steps lower risk:
- Brush twice daily and floss once a day.
- Visit your dentist for routine checks and cleanings.
- Treat cavities early — don’t wait.
- If you have an implant, follow special hygiene steps your dentist gives you.
- Control medical issues: diabetes, immune conditions, and smoking all raise the risk of severe infections.
- If a dentist prescribes antibiotics like zylomox 500mg capsules, take them exactly as instructed.
Special cases: when antibiotics are not the full answer
Antibiotics alone rarely fix an abscess that needs drainage. UK dental guidance and prescribing sources emphasize that surgical drainage and dental care are the main treatments, and antibiotics are used when the infection is severe or spreading. Overuse of antibiotics raises resistance and harms patients.
Safety and side effects of amoxicillin (and zylomox 500mg capsules)
Amoxicillin is generally safe for many people. Common side effects:
- Upset stomach, diarrhea, mild rash.
- Serious allergic reactions can occur; they are rare but require immediate medical help (hives, breathing trouble, swelling of face or throat).
- Amoxicillin can interact with some medications and alter blood clotting tests; clinicians consult FDA labeling for details.
If you think you are allergic to penicillin, tell your clinician. They will choose a safe alternative.
Quick action plan if you think you have a dental infection
- Call your dentist right away.
- Use warm salt rinses and pain relief (paracetamol/ibuprofen) as advised while you wait.
- If you have facial swelling, fever, trouble breathing, swallowing, severe headache, confusion, or double vision — go to emergency care.
- If a dentist prescribes zylomox 500mg capsules, take as directed and finish the course.
- Get the dental procedure (drainage/root canal/extraction) you were advised to have — antibiotics alone are often not enough.
Five Most Important Facts
- Dental abscesses need dental treatment; antibiotics alone are not usually enough.
- Amoxicillin (the drug in many brands including zylomox 500mg capsules) is a common first-line antibiotic for dental infections when indicated; dosing and safety are in the FDA label.
- Oral bacteria can, in rare cases, cause brain abscesses, which is documented in medical literature.
- Majorly, the spread of this is more likely in people with weakened immunity, delayed treatment, or infections that are not drained.
- Prompt dental and medical care greatly reduces the risk of severe complications.
Conclusion
Most dental infections can be treated if they are addressed early, but if you don't, they can cause serious problems, such as a brain abscess, which is very rare. The main way to treat it is to get rid of the source of the infection, which could be drainage, root canal, extraction, or implant care. If the infection spreads, Zylomox 500mg (amoxicillin) may be given, but it is not a substitute for dental care. Good oral hygiene, regular checkups, and getting care early are all important for preventing problems. You should visit your doctor right away if you have swelling, a fever, or have experienced trouble breathing or swallowing.
Frequently Asked Questions (FAQs)
Q1. Are antibiotics always needed for a tooth abscess?
No, if the infection is local and can be drained or treated with a root canal or extraction, antibiotics may not be needed. Antibiotics are used when the infection is spreading, the patient has systemic symptoms, or the patient is at high risk.
Q2. How fast do antibiotics like zylomox 500mg capsules work?
Many people feel less pain or swelling within 48–72 hours of starting an effective antibiotic. But the infected tooth often still needs a dental procedure (drainage, root canal, or extraction). Finish the full antibiotic course if one is prescribed.
Q3. Can a root canal spread infection to the brain?
A properly done root canal treats the infected tooth and reduces spread risk. If a tooth infection is left untreated or a treatment fails and the infection spreads, rare complications like brain abscess can occur. Prompt dental care lowers this risk.
Q4. If my implant is sore and the gum is red could this be a sign of infection?
Yes, early peri-implant infection looks like swollen, bleeding gums around the implant and can sometimes cause pain. See your dentist quickly. Early cleaning and antibiotics can help; advanced infection may require implant removal.
Q5. How rare is a dental infection reaching the brain?
It is rare in places with good dental care, but it still happens. Medical reviews show that oral bacteria can cause brain abscesses in some cases, especially with delayed care or weakened immunity. Any sudden severe headache, confusion, or neurological sign with a dental infection needs emergency care.
References (FDA, NHS, NIH & key clinical sources)
- NHS — Dental abscess. Information on symptoms and dental treatment.
- https://www.nhs.uk/conditions/dental-abscess/
- FDA — AMOXIL (amoxicillin) prescribing information (label). Useful for dosing, interactions, and safety. https://www.accessdata.fda.gov/drugsatfda_docs/label/2015/50542s02950754s01950760s01950761s016lbl.pdf
- NCBI / PubMed Central — case reports and reviews on brain abscesses linked to dental infections.
https://pmc.ncbi.nlm.nih.gov/articles/PMC7026700/
- MedlinePlus (NIH) — overview of brain abscess causes and diagnosis.
https://medlineplus.gov/ency/article/000783.htm















Sign in to leave a comment.