Hey there, if you're dipping your toes into the world of healthcare administration, you've probably heard about medical billing and coding. It's one of those behind-the-scenes roles that keeps the whole system running smoothly, especially here in the USA where regulations can get pretty tangled. I'm no stranger to this field—I've chatted with coders who juggle ICD-10 codes like pros and billers who chase down insurance claims with the persistence of a detective. Today, let's break it down in a way that's easy to digest, without all the jargon overload. We'll cover what it really entails, why it's booming, and how you can get started or level up your game.
What Exactly Is Medical Billing and Coding Anyway?
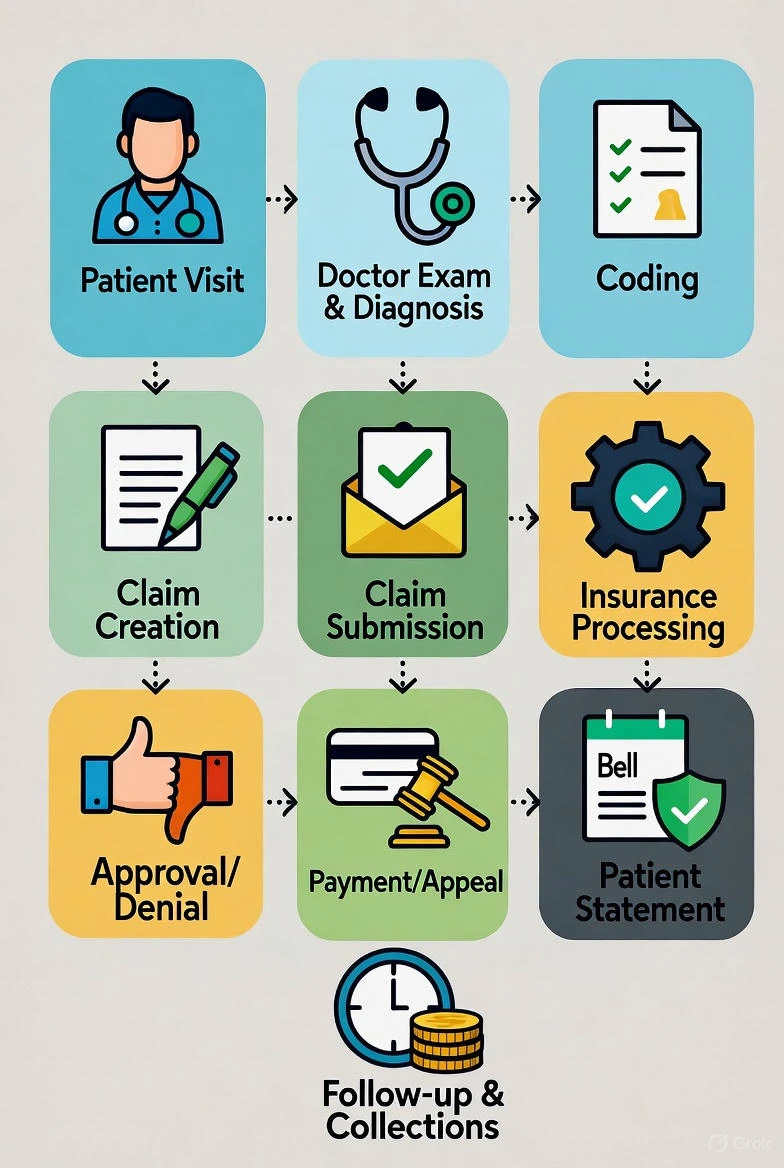
Okay, let's start from square one. Medical coding is basically translating doctors' notes, diagnoses, and procedures into standardized codes. Think of it as turning a patient's story—"Hey, I broke my arm playing basketball"—into something like S42.301A for a fractured humerus. These codes come from systems like ICD-10 for diagnoses, CPT for procedures, and HCPCS for supplies. It's crucial because without accurate codes, hospitals and clinics can't get paid properly.
Billing, on the other hand, takes those codes and turns them into claims sent to insurance companies or patients. It's the money side of things—making sure reimbursements come in on time, handling denials, and sometimes negotiating with payers. In the USA, with laws like HIPAA protecting patient privacy and the Affordable Care Act shaking things up, you gotta stay sharp.
Why does this matter? Well, errors can lead to big headaches—delayed payments, audits, or even legal troubles. But get it right, and you're the hero keeping cash flowing. Fun fact: The Bureau of Labor Statistics says jobs in this field are growing faster than average, thanks to an aging population and more folks needing healthcare.
The Daily Grind: What a Typical Day Looks Like
Ever wonder what it's like on the job? It's not all sitting in a cubicle staring at screens—though there's plenty of that. A coder might start their morning reviewing patient charts from the night before, assigning codes while sipping coffee. Afternoon could involve double-checking work to avoid those pesky denials.
For billers, it's more about follow-ups. Picture this: You submit a claim, but it bounces back because the code doesn't match the diagnosis. Time to investigate—call the insurer, tweak the claim, resubmit. It's a mix of detective work and customer service.
Here are some real-talk tips to make your day smoother:
- Stay organized with tools: Use software like Epic or Cerner to track everything. Don't rely on sticky notes; they'll betray you eventually.
- Double-check everything: One misplaced digit in a code can cost thousands. I once heard of a clinic losing out on $50K because of a simple typo—yikes!
- Keep learning: Certifications like CPC or CCS aren't just paper; they open doors. Renew them every couple years to stay current.
- Handle stress like a boss: Denials happen. Take a breath, appeal if needed, and move on. It's part of the game.
If you're remote—which is super common now post-pandemic—set up a cozy workspace. Noise-canceling headphones are a lifesaver when you're deep in concentration.
Challenges in the USA Landscape and How to Tackle Them
No sugarcoating it: Medical billing and coding in the USA isn't always a walk in the park. With constant updates to codes—ICD-11 is looming—and varying state regulations, it's easy to feel overwhelmed. Plus, insurance companies love throwing curveballs, like changing reimbursement rates or requiring pre-authorizations for everything.
Then there's the tech side. Electronic health records (EHRs) are great, but glitches happen. And don't get me started on payer mix—Medicare, Medicaid, private insurers—they all have their own rules.
But hey, you're not alone. Here's how to navigate these bumps:
- Embrace audits: Regular internal checks catch issues early. Think of them as tune-ups for your processes.
- Network with peers: Join forums like AAPC's community or LinkedIn groups. Sharing war stories can lead to killer advice.
- Outsource when it makes sense: Small practices often farm out billing to pros, freeing up time for patient care.
- Stay compliant: HIPAA violations can sting with fines up to $50K per incident. Train your team regularly—better safe than sorry.
One colleague of mine switched to AI-assisted coding tools, and it cut her error rate in half. Tech's evolving fast, so keep an eye on it.
Skills You Need to Shine in This Field
Alright, let's talk brass tacks: What do you need to succeed? It's not just about memorizing codes; it's a blend of smarts and soft skills.
First off, attention to detail is non-negotiable. Miss a modifier on a CPT code? Boom, claim denied. Analytical thinking helps too—connecting diagnoses to procedures logically.
Communication's key. You'll explain billing to patients who are confused or upset, or negotiate with insurers. Be empathetic; nobody likes surprise bills.
Tech savvy? Absolutely. Familiarity with billing software and Microsoft Office is a must. And medical terminology—learn it like your favorite playlist.
To build these up:
- Get certified: Start with the Certified Professional Coder (CPC) exam. It's tough but worth it—salaries jump to around $50K-$70K average in the USA.
- Hands-on experience: Internships or entry-level jobs in clinics build real-world chops.
- Continuous education: Webinars, workshops—heck, even YouTube channels on coding updates.
- Soft skills practice: Role-play patient interactions. It feels awkward at first, but pays off.
Remember, everyone starts somewhere. I knew a gal who began as a receptionist and climbed to billing manager in five years. Persistence wins.
Future Trends: What's Coming Down the Pike?
Looking ahead, medical billing and coding in the USA is shifting gears. Telehealth exploded during COVID, bringing new codes for virtual visits. Value-based care is pushing for outcomes over volume, meaning billers track quality metrics too.
AI and automation? Game-changers. Tools that auto-suggest codes or flag errors are popping up, but they won't replace humans—yet. You'll still need that human touch for complex cases.
Sustainability's creeping in too—digital claims reduce paper waste. And with healthcare costs rising, efficiency is king.
To stay ahead:
- Watch policy changes: Follow CMS updates; they dictate a lot.
- Adopt new tech: Learn about blockchain for secure claims or RPA for repetitive tasks.
- Diversify skills: Specialize in areas like oncology coding—niche expertise commands higher pay.
- Advocate for yourself: Push for better work-life balance; burnout's real in this field.
It's an exciting time—jobs are projected to grow 8% by 2032, per BLS. Jump in now, and you'll ride the wave.
Wrapping It Up: Your Next Steps
So, we've covered the basics, the challenges, and the bright future of medical billing and coding in the USA. It's a rewarding career if you like puzzles, helping people, and a steady paycheck. Whether you're just curious or ready to dive in, start with education and build from there. And if it all feels a bit much, remember: pros are out there to help.
For top-notch support, check out 247 Medical Billing Services—they're pros at handling the nitty-gritty so you can focus on what matters. They've got round-the-clock expertise to streamline your processes. Give 'em a shout if you're overwhelmed; it could be a game-changer.



















Sign in to leave a comment.