In every hospital, clinic, or physician’s office, there’s a quiet rhythm that keeps everything moving — care is delivered, patients are comforted, and claims are filed. But when those claims are denied, that rhythm falters.
What was once a smooth process suddenly becomes a maze of rework, resubmissions, and revenue uncertainty. Denials don’t just cost money — they cost time, trust, and sometimes even patient satisfaction.
This is where the story of Denial Management in Healthcare begins — and how Fine Claim LLC helps rewrite its ending.
The Hidden Cost of Denials
Every denied claim tells a story. Sometimes it’s a coding error buried deep in documentation. Other times, it’s a simple eligibility mismatch that slipped through the cracks. But when hundreds or thousands of denials pile up, the financial impact becomes staggering.
Studies show that nearly 1 in 5 medical claims are denied, and more than 60% of those denials are never resubmitted. For hospitals, this means millions in uncollected revenue — money that could have supported staff, upgraded equipment, or expanded care services.
For healthcare administrators, denial management often feels like fighting an invisible enemy — one that constantly changes form.
The Turning Point: From Frustration to Focus
Meet a mid-sized community hospital that was struggling with rising denial rates and shrinking margins. Their billing team worked tirelessly, yet reimbursement delays kept mounting. The CFO described it best:
“We weren’t losing because of bad care — we were losing because of bad data.”
That’s when they turned to Fine Claim LLC.
Instead of simply appealing denials, Fine Claim LLC dug deeper. Their experts analyzed every stage of the revenue cycle — from patient registration to claims submission. Using advanced analytics and denial tracking tools, they uncovered patterns that had gone unnoticed for months.
Errors in patient eligibility. Missing modifiers. Outdated payer rules. Each insight was a small revelation — and together, they painted a roadmap to recovery.
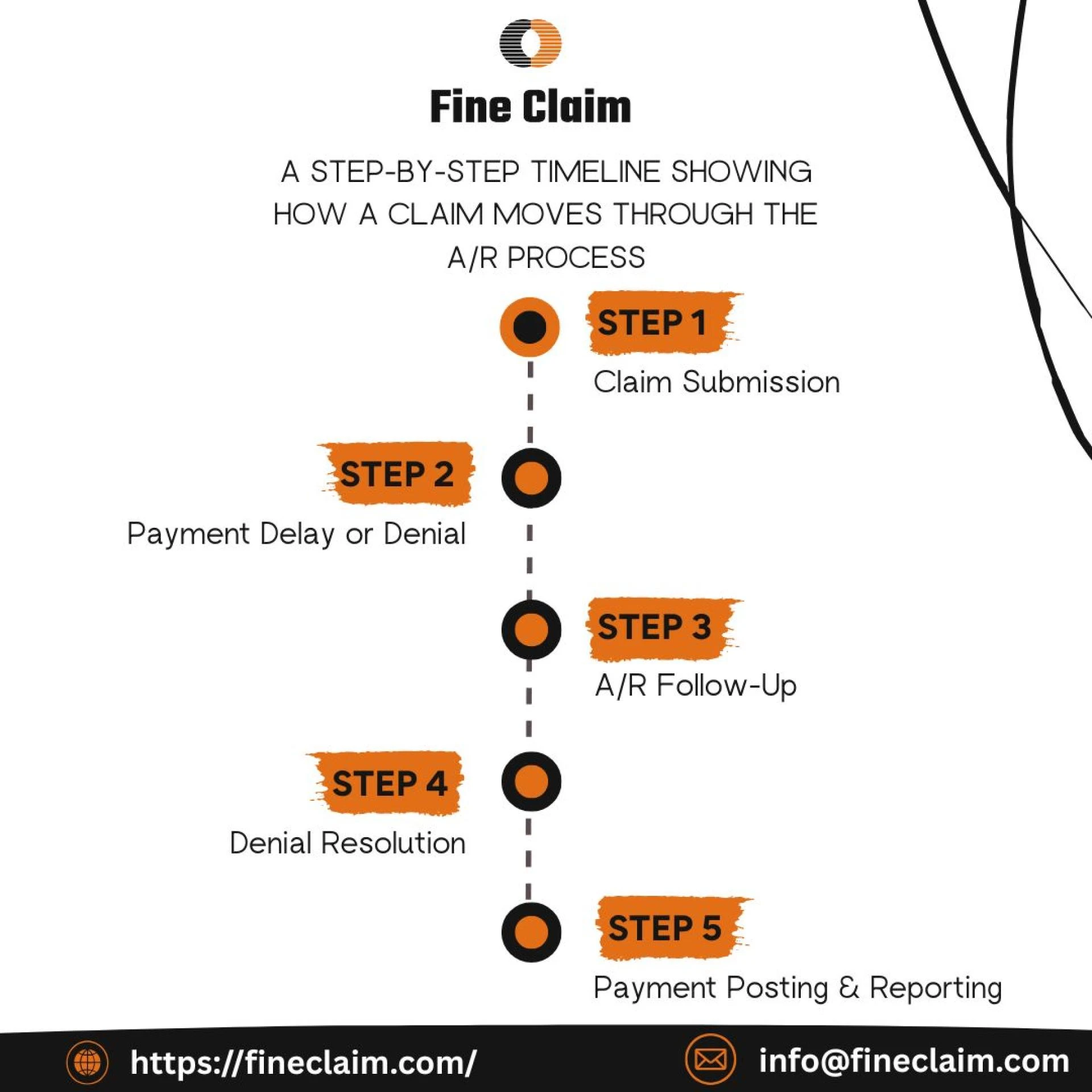
Fine Claim LLC’s Denial Management Approach
Fine Claim LLC believes that denial management isn’t just about “fixing” rejected claims — it’s about preventing them altogether.
Their proven approach combines technology, transparency, and teamwork:
- Root Cause Analysis – Every denial is dissected to identify the real issue, not just the symptom.
- Predictive Analytics – AI tools forecast which claims are most at risk of rejection.
- Process Optimization – Automated workflows ensure accuracy before submission.
- Staff Empowerment – Continuous education ensures front-end teams avoid recurring mistakes.
- Patient-Centric Communication – Billing processes are simplified to reduce confusion and improve satisfaction.
With this holistic model, Fine Claim LLC doesn’t just recover lost revenue — it transforms how organizations think about their revenue cycle.
The Human Side of Denials
Behind every denial is more than just a financial loss — there’s a patient waiting for coverage approval, a provider anxious to get paid, and a billing team working overtime to fix the issue.
Fine Claim LLC understands that at the heart of denial management lies human care. Their team brings empathy to every interaction, ensuring that while claims get corrected, the patient experience remains positive.
That’s what sets them apart — a blend of technology and humanity, working together to keep healthcare financially and emotionally healthy.
The Outcome: Turning Denials into Wins
Within just a few months, that same community hospital saw a 35% reduction in denial rates and a significant boost in cash flow. Their average claim turnaround time improved, and staff finally had time to focus on patients — not paperwork.
But perhaps the most rewarding result wasn’t financial. It was emotional. The CFO shared later:
“For the first time in years, our revenue team isn’t chasing claims. They’re leading them.”
The Future of Denial Management
The healthcare industry is changing fast — payer rules evolve, coding updates are frequent, and compliance demands never stop. But denial management no longer needs to be reactive.
With Fine Claim LLC’s data-driven RCM solutions, providers can stay ahead of denials, strengthen compliance, and secure consistent revenue flow.
It’s more than just managing claims — it’s mastering them.
Conclusion: A New Chapter for Healthcare Revenue
Every denied claim begins as a problem. But with the right partner, it can become a powerful opportunity for improvement.
Fine Claim LLC is rewriting the story of Denial Management in Healthcare — one clean claim, one recovered dollar, and one empowered team at a time.
Because in healthcare, every claim matters. And with Fine Claim LLC, every claim finds its way home.


















Sign in to leave a comment.