Wounds are a common concern, especially for the elderly and those with chronic conditions. From minor scrapes to deep ulcers, each wound type demands specific attention. Understanding the types of wounds, along with their causes, risks & management, is crucial — particularly for health professionals and caregivers dealing with non healing wound treatment scenarios.
1. Arterial Ulcers
Causes
Arterial ulcers are commonly caused by atherosclerosis, a condition where the arteries become narrowed due to plaque buildup. Smoking significantly increases the risk of arterial ulcers by impairing blood circulation. People with diabetes are particularly vulnerable due to compromised vascular health. Additionally, high cholesterol levels contribute to the narrowing of arteries, reducing blood flow to extremities.
Risks
If left untreated, arterial ulcers can lead to tissue death or necrosis. In extreme cases, gangrene may set in, necessitating amputation. The prolonged healing time also raises the risk of infection and prolonged immobility.
Management
Management often involves procedures like vascular surgery or angioplasty to restore blood flow. Patients are strongly advised to quit smoking to improve circulation. In cases where venous insufficiency is also present, wearing compression stockings can help. Maintaining the cleanliness of the wound and applying topical antibiotics reduces the risk of infection.
Also Read Risk Factors for Arterial Ulcers and How to Reduce Them
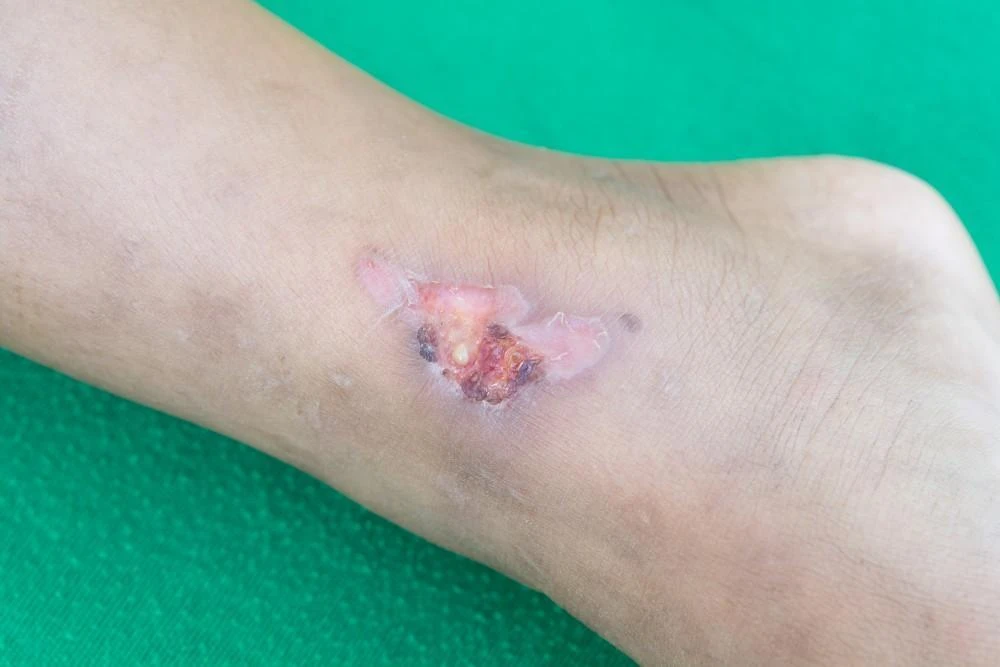
2. Chronic Non-Healing Wounds
Causes
Chronic non-healing wounds typically develop due to poor blood circulation, which hinders the delivery of oxygen and nutrients essential for tissue repair. Malnutrition also plays a role by depriving the body of proteins and vitamins needed for healing. Diabetes contributes to these wounds through poor glycaemic control and nerve damage. Lastly, persistent infections prevent the wound from closing.
Risks
These wounds can lead to chronic pain and functional impairment. If not properly treated, they may become breeding grounds for harmful bacteria, increasing the chance of systemic infections. Patients may also suffer socially due to foul odour or leakage, affecting mental health.
Management
Treating these wounds requires advanced wound care techniques such as hydrocolloid dressings that keep the wound moist and protected. Nutritional therapy ensures the patient receives adequate protein, vitamins, and minerals. Non healing wound treatment centres often offer therapies like debridement (removing dead tissue) and negative pressure wound therapy to accelerate healing.
Also check: Non healing wound treatment
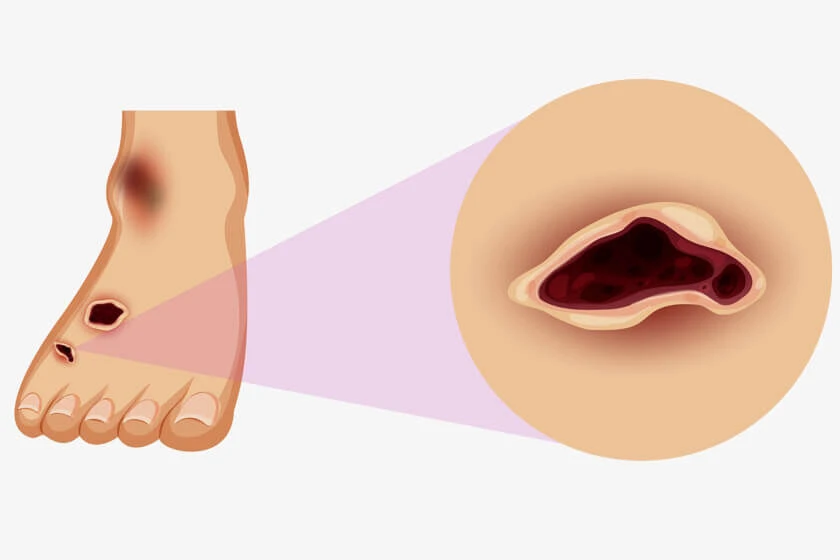
3. Diabetic Foot Ulcers
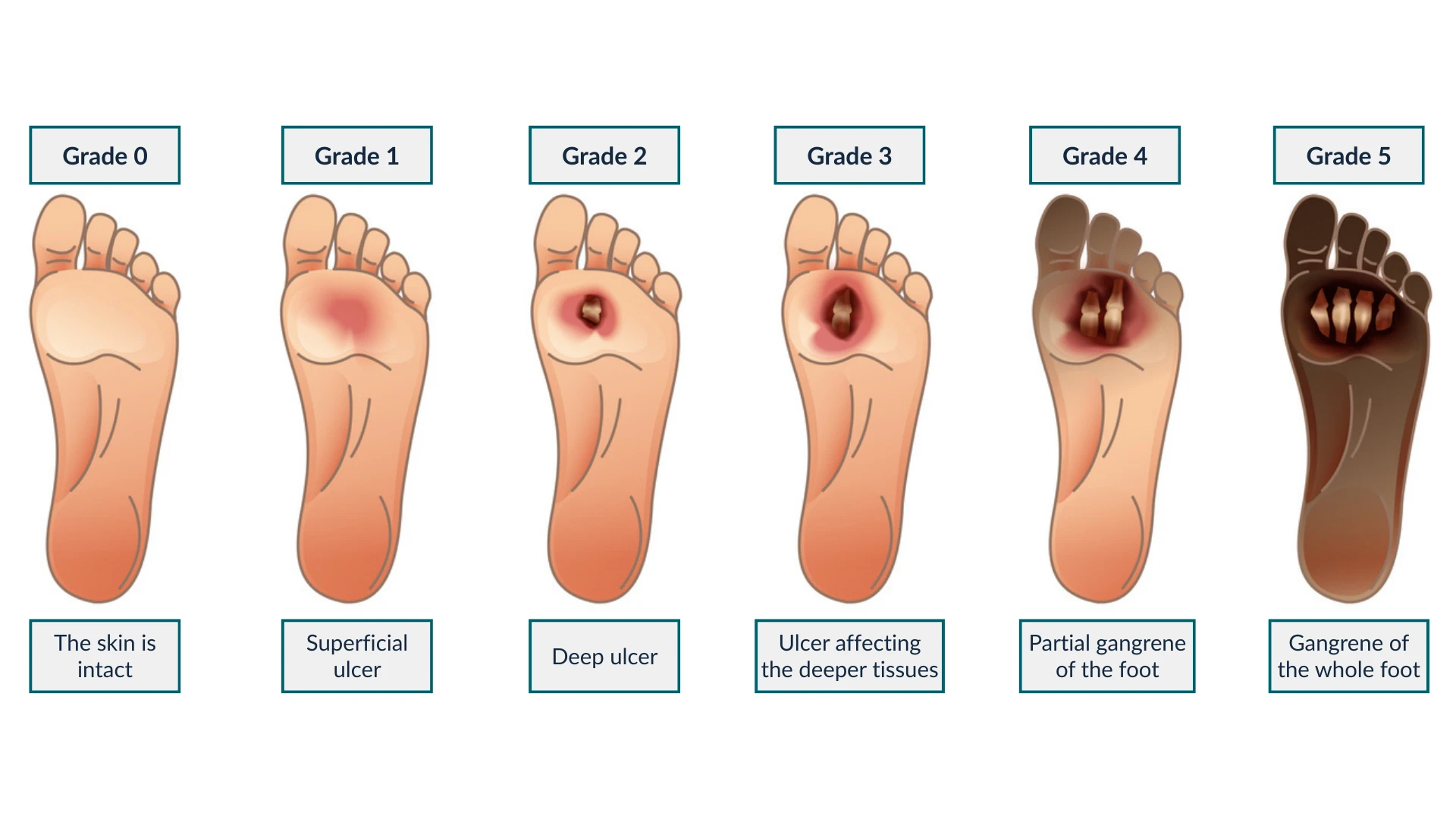
Causes (Expanded via Stages)
In the early stage of a diabetic foot ulcer, patients may notice redness, thickened skin (calluses), or small cuts that go unnoticed due to neuropathy. As it progresses through diabetic foot ulcer stages, the wound becomes deeper, affecting soft tissues and possibly exposing bone. In stage 4 diabetic foot ulcers, necrosis and gangrene are common, and amputation risk is extremely high.
Risks
These ulcers can cause life-threatening infections like cellulitis or osteomyelitis. If the wound penetrates deep tissue or bone, it may require surgical removal of the affected area. Uncontrolled ulcers can lead to sepsis or even death in vulnerable patients.
Management
Management begins with tight control of blood sugar levels to prevent worsening. Patients are advised to use custom orthotics or specialized footwear to relieve pressure on the wound. Antibiotics are used if signs of infection are present. In advanced cases like stage 4 diabetic foot ulcers, surgical intervention may be necessary to remove dead tissue or amputate.
Read the full guide: What Are Diabetic Foot Ulcers? Causes, Symptoms, and Treatment
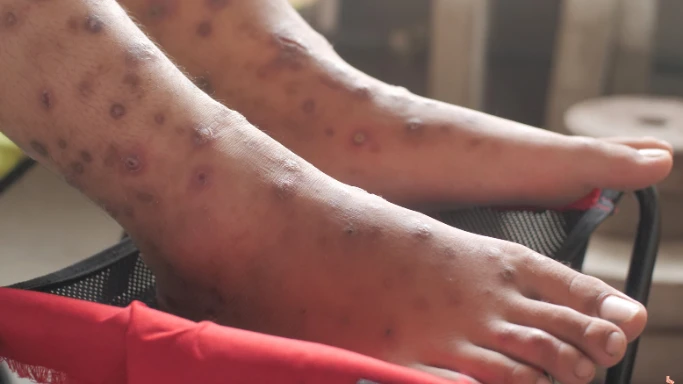
4. Infectious Wounds
Causes
Infectious wounds occur when bacteria invade an open wound, often due to improper wound cleaning. Elderly individuals with weak immune systems are more likely to develop such infections. The presence of foreign materials like surgical sutures or implants can also trigger bacterial growth.
Risks
If left untreated, infectious wounds can cause localised swelling and redness that may spread to nearby tissues. They can evolve into serious conditions like abscesses or lead to bloodstream infections (sepsis), which can be fatal.
Management
Proper wound hygiene is essential, including daily cleaning and sterile dressing changes. If infection is suspected, antibiotic therapy may be prescribed. Elder care facilities should follow stringent infection control practices to protect vulnerable patients.
Learn About:Daily Wound Care Routine to Prevent Infections
5. Venous Leg Ulcers
Causes
Venous ulcers develop due to chronic venous insufficiency, where the veins in the legs fail to circulate blood effectively. Faulty valves allow blood to pool in the legs, causing pressure that breaks down skin. Individuals with a history of Deep Vein Thrombosis (DVT) are at higher risk. Standing or sitting for long periods can also contribute.
Risks
Patients with venous leg ulcers may experience frequent infections due to fluid leakage. The skin may darken or harden, making the area prone to new wounds. Untreated ulcers can evolve into non healing wounds.
Management
Compression therapy, such as wearing compression stockings, helps improve venous return and reduce swelling. Elevating the legs frequently throughout the day also helps blood flow. Routine wound care with medicated dressings supports healing. Vascular referrals are advised for underlying circulatory issues.
Also Learn: Daily Care Tips for Venous Leg Ulcers: How to Prevent Infections
6. Pediatric Wounds
Causes
Children often sustain wounds from falls, cuts, or minor burns during play. Post-surgical wounds and congenital skin disorders may also be present. Despite faster healing, children’s wounds, or pediatric wounds, must be managed carefully due to their sensitive skin.
Risks
Improper care can lead to hypertrophic scars or keloids, which may be emotionally distressing. Infections may also develop, particularly if the child scratches the wound. If a wound becomes chronic, it may affect growth or development.
Management
Pediatric wounds are treated with gentle, non-invasive methods. Pain control is crucial, often through mild analgesics. Parents and caregivers must be educated on signs of infection and proper wound dressing techniques to ensure safe recovery.
Also Read: Understanding Pediatric Wounds: Types, Causes, and Treatments
7. Pressure Ulcers (Bedsores)
Causes
Pressure ulcers form when soft tissue is compressed between bone and a hard surface for prolonged periods. This is common in bedridden or immobile patients. Friction and shear forces caused during movement can worsen the breakdown of skin.
Risks
Without intervention, pressure ulcers can become deep wounds exposing muscle or bone. These wounds often get infected and are difficult to treat. They may extend hospital stays and increase mortality risk in elderly patients.
Management
Caregivers should implement a repositioning schedule to change the patient’s position every two hours. Specialized mattresses and cushions help reduce pressure points. Nutritional support with adequate protein and hydration accelerates tissue regeneration. Mild to moderate infections are treated with topical antibiotics.
Must read: how to prevent bed sores on a bedridden patient
Frequently Asked Questions (FAQs)
1. What are the main types of non healing wounds?
Non healing wounds include diabetic ulcers, arterial and venous ulcers, pressure sores, and infected post-surgical wounds.
2. How do I identify an early-stage diabetic foot ulcer?
Redness, swelling, and calluses with reduced sensation around the toes or foot area indicate early-stage symptoms.For more, Read this guide about Diabetic foot ulcer stages
3. What does stage 4 diabetic foot ulcer mean?
It’s the most severe stage where there’s deep tissue involvement, necrosis, or even gangrene — usually requiring surgery or amputation.
4. What is the best treatment for non healing wounds?
Treatment includes debridement, negative pressure therapy, and use of advanced dressings, along with treating underlying causes like diabetes or poor circulation.
5. How can I prevent pressure ulcers in elderly patients?
Regular repositioning, use of pressure-relieving devices, and maintaining dry, clean skin can help prevent bedsores.
6. Are venous leg ulcers curable?
Yes, with compression therapy, wound management, and proper follow-up care, most cases can be healed.
Conclusion
Understanding the types of wounds, especially in the elderly, is crucial for timely intervention and effective care. From diabetic foot ulcer stages to non healing wound treatment, every wound type demands a tailored approach.
Whether you’re a caregiver or a medical professional, addressing these wounds early with proper knowledge can prevent complications and ensure better recovery outcomes.














Sign in to leave a comment.