Introduction
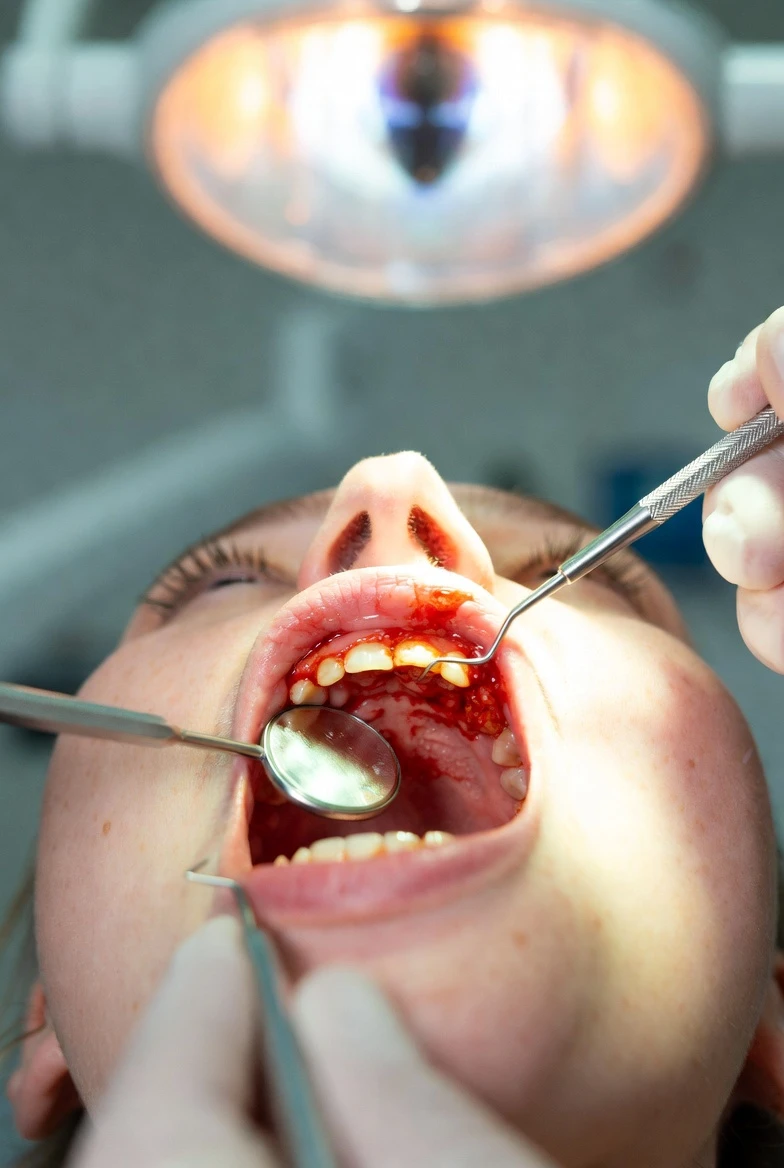
You notice it while brushing one morning—a streak of pink in the sink. Maybe your gums look a little puffy, or you realize that one tooth seems longer than its neighbors. These aren't cosmetic concerns to ignore or cover with whitening toothpaste. They're your body's warning system, and they're telling you that your gum health needs immediate attention.
I ignored bleeding gums for years, assuming they were normal or that I was brushing too hard. The reality? I was developing early periodontal disease that could have cost me teeth if left untreated. Gum disease is sneaky—it rarely hurts until it's advanced, which is exactly why routine symptoms like bleeding deserve respect, not dismissal.
The good news? Modern periodontics offers genuine solutions. Not just management, but actual regeneration and restoration. Understanding your options empowers you to take control before minor inflammation becomes major tooth loss.
Understanding the Gum-Disease Connection
Your gums aren't decorative. They form a tight seal around teeth, protecting the underlying bone and periodontal ligament that hold everything in place. When this seal breaks down, the cascade begins:
Gingivitis is the early stage—reversible inflammation caused by bacterial plaque accumulation. Gums bleed easily, may appear swollen or red, but no permanent tissue damage occurs yet. This is your window of opportunity, and seeking professional advice early can make a major difference, so visit Parramatta Green Dental for timely dental treatment and preventive care.
Periodontitis represents progression. Inflammation deepens, creating pockets between gum and tooth where bacteria thrive. The body's immune response, ironically, destroys the very bone and tissue trying to fight infection. Teeth loosen. Gums recede. Damage becomes permanent without intervention, which is why many patients visit Parramatta Green Dental to receive advanced treatment before the condition worsens.
Advanced periodontitis features significant bone loss, deep pockets, tooth mobility, and often requires extraction. This isn't inevitable aging—it's untreated disease.
| Stage | Gum Appearance | Bleeding | Bone Loss | Treatment Approach |
|---|---|---|---|---|
| Healthy | Pink, firm, knife-edged | None | None | Prevention, regular cleanings |
| Gingivitis | Red, slightly swollen | Brushing/flossing | None | Professional cleaning, improved home care |
| Mild periodontitis | Red, swollen, early recession | Spontaneous possible | 1-2mm | Scaling and root planing, localized antibiotics |
| Moderate periodontitis | Significant recession, deep pockets | Frequent | 3-4mm | Deep cleaning, possible surgical intervention |
| Advanced periodontitis | Severe recession, tooth exposure | Constant | 5mm+ | Surgery, regeneration procedures, or extraction |
Why Gums Bleed: Beyond "Brushing Too Hard"
The "you're brushing too hard" explanation is partially true but often incomplete. Aggressive brushing with stiff bristles can cause gum recession and bleeding, but it's rarely the primary culprit in persistent cases.
Bacterial infection is the most common cause. Plaque—a sticky film of bacteria—accumulates at the gumline. Your immune system responds with inflammation, increasing blood flow to the area. This makes gums fragile and prone to bleeding with minimal provocation.
Hormonal changes amplify gum sensitivity. Pregnancy, puberty, menstruation, and menopause all increase blood flow to gum tissue and may exaggerate response to plaque. This doesn't mean the plaque isn't there—it means your body reacts more strongly to it.
Medications play a surprising role. Blood thinners obviously increase bleeding tendency, but so do some antidepressants, heart medications, and oral contraceptives. Always inform your dentist about medications; they change treatment approaches.
Systemic conditions including diabetes, leukemia, and vitamin deficiencies (especially C and K) manifest in gum health. Bleeding gums can be an early warning sign of broader health issues.
Comparative Analysis: Treatment Modalities by Severity
| Treatment | Indicated For | Procedure | Recovery | Success Rate |
|---|---|---|---|---|
| Professional cleaning (prophylaxis) | Gingivitis, prevention | Remove plaque/tartar above gumline | Immediate | 95%+ with good home care |
| Scaling and root planing | Mild to moderate periodontitis | Deep cleaning below gumline, smooth roots | 24-48 hours sensitivity | 70-85% pocket reduction |
| Localized antibiotic therapy | Localized moderate disease | Place antibiotic gel in deep pockets | None | Enhances scaling results 15-20% |
| Flap surgery | Moderate to advanced periodontitis | Reflect gum tissue, clean roots, reduce pockets | 1-2 weeks | 60-80% long-term stability |
| Regenerative procedures | Vertical bone defects | Grafts, membranes, growth factors to rebuild bone | 2-4 weeks | 50-70% bone fill depending on defect |
| Gum grafting | Recession, root exposure | Transplant tissue to cover exposed roots | 2-3 weeks | 85-95% root coverage |
Scaling and Root Planing: The Deep Clean That Saves Teeth
Often called "deep cleaning," scaling and root planing is the first-line treatment for periodontitis. It's not a more intense regular cleaning—it's a completely different procedure targeting infection below the gumline.
Scaling removes plaque and tartar (calculus) from tooth surfaces and root surfaces below the gumline. Your hygienist uses ultrasonic instruments that vibrate deposits loose, combined with hand instruments for precision. This isn't comfortable—local anesthesia is standard for deeper pockets—but it's transformative.
Root planing smooths rough root surfaces where bacteria colonize. Think of it like sanding a rough board; smooth surfaces resist new plaque accumulation. This gives your gums a clean foundation to reattach.
The aftermath includes temporary sensitivity (exposed root surfaces react to temperature) and gum shrinkage as swelling resolves. This isn't recession getting worse—it's inflammation resolving to reveal the true tissue level. Pockets shrink as gums tighten against teeth.
Adjunctive therapies enhance results. Local antibiotics placed directly into pockets provide concentrated bacterial killing without systemic side effects. Laser therapy can decontaminate pocket walls and stimulate healing. These aren't replacements for mechanical cleaning but powerful additions to it.
Surgical Solutions: When Conservative Treatment Isn't Enough
Moderate to advanced periodontitis often requires surgical intervention. Modern techniques prioritize regeneration over resection—saving tissue rather than removing it.
Flap surgery provides access. The gum is gently reflected back, exposing root surfaces and bone for thorough cleaning. Your periodontist can then reshape bone to eliminate pockets and position gum tissue at a healthy level. Sutures hold everything in place during healing.
Regenerative procedures represent the cutting edge. For specific defect types (vertical bone loss with surrounding walls), your surgeon can place:
- Bone grafts (your own, donor, or synthetic) to provide scaffolding
- Barrier membranes to exclude fast-growing gum tissue while bone regenerates
- Growth factors like Emdogain or platelet-rich fibrin to accelerate healing
These techniques can actually rebuild lost bone, something impossible just decades ago. Not all cases qualify—success depends on defect shape, oral hygiene, and smoking status—but when indicated, results are remarkable.
Gum grafting addresses recession specifically. Connective tissue from your palate (or donor tissue) is transplanted to cover exposed roots. This stops progression, reduces sensitivity, and improves appearance. Techniques have evolved from invasive free gingival grafts to minimally invasive tunneling procedures with faster recovery.
The Home Care Revolution: What Actually Works
Professional treatment without home care is like repairing a roof while it's still raining. Your daily routine determines long-term success:
Toothbrush selection matters enormously. Soft bristles only—medium and hard brushes abrade enamel and traumatize gums. Electric brushes with pressure sensors prevent the "scrubbing harder is better" instinct that causes recession.
Flossing technique is where most people fail. It's not sawing back and forth—it's curving the floss into a C-shape, sliding under the gumline, and gently scraping the tooth surface. If you're snapping floss between teeth, you're damaging papilla (gum tissue between teeth).
Interdental brushes clean spaces that floss misses, especially with gum recession creating larger gaps. Sized appropriately (they should fit snugly without force), they're more effective than floss for many patients.
Antimicrobial rinses reduce bacterial load. Chlorhexidine prescription rinses are powerful short-term tools, though they stain teeth with extended use. Over-the-counter options with essential oils or cetylpyridinium chloride provide maintenance benefits.
Prevention: Stopping the Cycle Before It Starts
The best treatment is never needing it. Prevention strategies for gum health:
Professional cleanings every 6 months (or 3-4 months if you have a history of gum disease) remove calculus you can't reach. No amount of home care substitutes for this.
Smoking cessation is the single most impactful change. Smokers are 3-6 times more likely to develop periodontal disease, and treatment success rates plummet. Vaping isn't safer—nicotine reduces blood flow to gums, impairing healing and immune response.
Stress management sounds like wellness fluff, but cortisol elevation directly impairs immune function and increases inflammation. Chronic stress manifests in your mouth.
Diabetes control is bidirectional—gum disease worsens blood sugar control, and poor control accelerates gum disease. Managing one helps the other.
Conclusion
Bleeding gums aren't a life sentence, and recession isn't inevitable aging. They're signals—sometimes subtle, sometimes urgent—that your periodontal health needs attention. The treatments available today can halt disease, regenerate lost tissue, and restore both function and aesthetics.
The key is acting early, when interventions are conservative and outcomes are predictable. Waiting for pain means waiting too long. If you've noticed bleeding, swelling, recession, or persistent bad breath, schedule a periodontal evaluation. Your gums support everything else in your mouth—they deserve priority care.















Sign in to leave a comment.