The Drug That Changed How We Think About Aging
What if the key to living longer was already sitting in a doctor's prescription pad?
For decades, aging was treated as an inevitable, unstoppable process — something to manage, not reverse. But a growing body of scientific evidence is challenging that assumption. At the forefront of this shift is rapamycin, a compound discovered in the soil of Easter Island in 1964, which has since become arguably the most exciting molecule in longevity science.
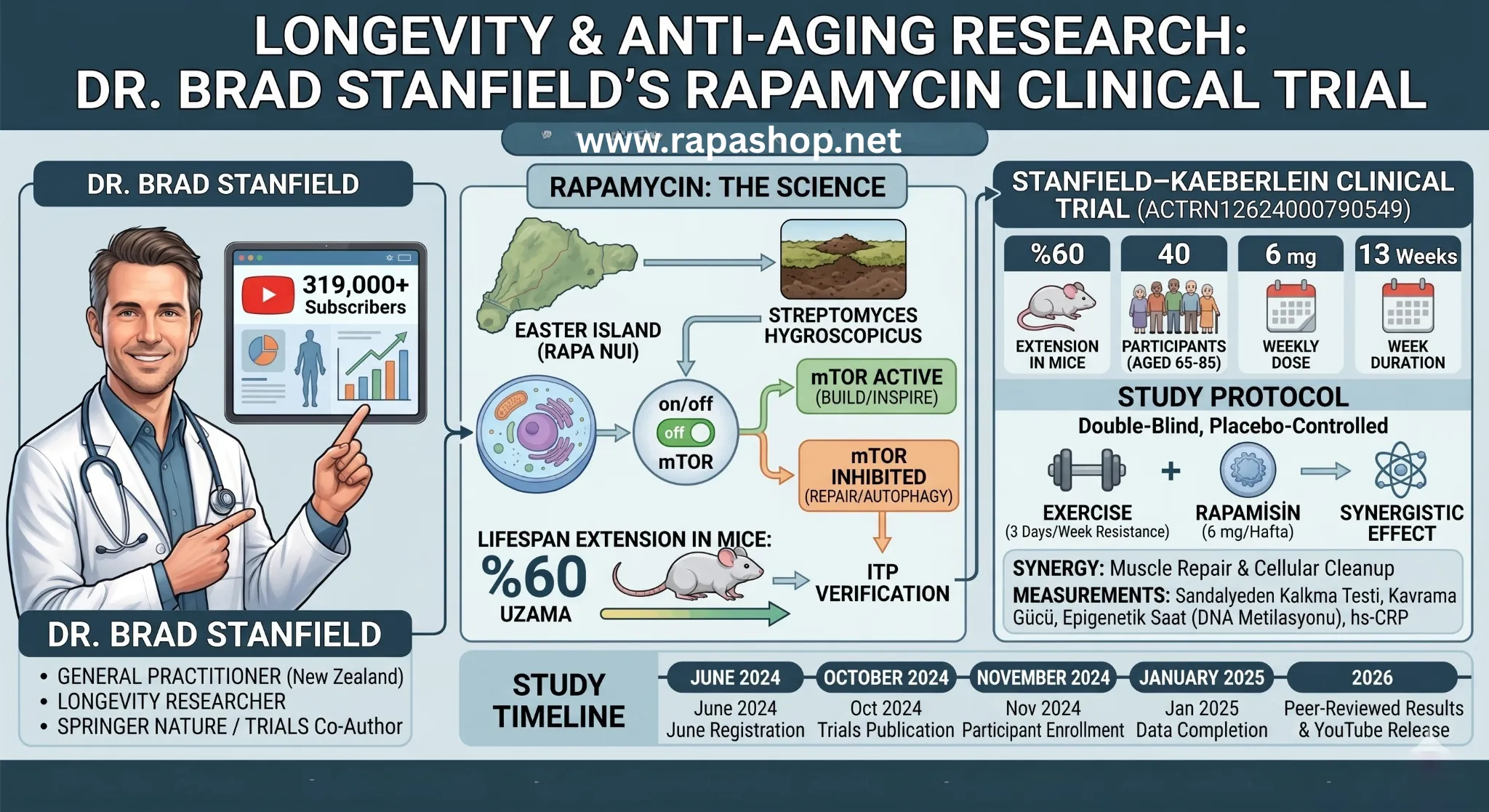
Leading the charge in bringing rapamycin research to human clinical trials is Dr. Brad Stanfield — a New Zealand General Practitioner, peer-reviewed researcher, and science communicator with over 319,000 YouTube subscribers. Together with Professor Matt Kaeberlein of the University of Washington, Dr. Stanfield has designed and launched a landmark clinical study that could reshape how medicine approaches aging.
This article breaks down the science, the study, and why the results could matter for every one of us.
Who Is Dr. Brad Stanfield?
Dr. Brad Stanfield is not a typical longevity influencer. He is a practicing General Practitioner in Auckland, New Zealand, a Fellow of the Royal New Zealand College of General Practitioners, and a clinical researcher affiliated with the University of Auckland. His work sits at the intersection of frontline medicine and cutting-edge longevity science.
What sets Dr. Stanfield apart is his insistence on evidence. On his website and YouTube channel, he consistently pushes back against supplement marketing hype, directing his audience toward interventions that have actually survived rigorous scientific scrutiny. When Dr. Stanfield calls something promising, it carries real scientific weight.
Rapamycin is one of the very few compounds he considers genuinely promising for human longevity — and he has put his own funding behind proving it.

Buy Rapamycin now
What Is Rapamycin? A Brief History
The story of rapamycin begins with an unlikely expedition. In 1964, a team of Canadian researchers traveled to Easter Island — known locally as Rapa Nui — and collected soil samples. Within those samples, a bacterium called Streptomyces hygroscopicus was producing a remarkable compound. That compound was named rapamycin after the island itself.
Initially studied for its antifungal and immune-suppressing properties, rapamycin was approved by the FDA in 1999 to prevent organ rejection in transplant patients. It is also used in certain cancer treatments. But it was its unexpected effect on a cellular signaling pathway called mTOR that eventually placed rapamycin at the heart of aging research worldwide.
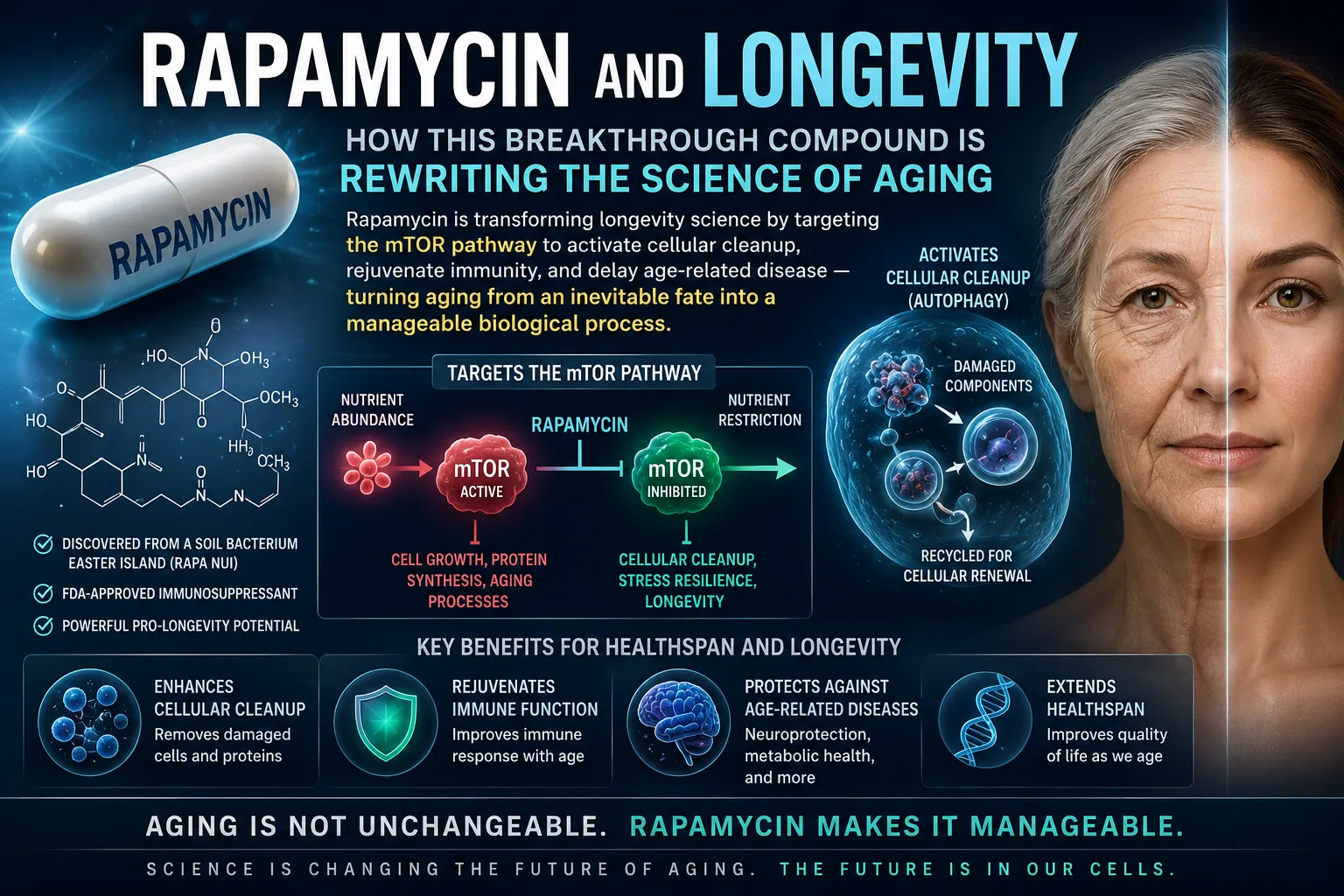
What is mTOR? mTOR stands for "mechanistic target of rapamycin." It is a protein complex inside your cells that acts like a master control switch, sensing nutrient availability and growth signals. When nutrients are abundant, mTOR switches to "build mode" — cells grow, divide, and produce proteins. When nutrients are scarce, or when rapamycin is administered, mTOR switches to "repair mode" — cells activate autophagy, clearing out damaged components and renewing themselves from within.
Chronic overactivation of mTOR — which commonly occurs as we age — is increasingly recognized as a key driver of age-related disease. Rapamycin, by periodically hitting the brakes on mTOR, may help restore the body's natural cellular maintenance systems.
What is autophagy? Autophagy literally means "self-eating" in Greek. It is the process by which cells identify and break down damaged proteins, dysfunctional organelles, and other cellular debris. Think of it as the body's internal recycling and cleanup system. Rapamycin activates this process by suppressing mTOR — and robust autophagy is strongly associated with healthy aging.
The Science: What Rapamycin Has Already Achieved
The case for rapamycin is built on some of the most rigorous longevity data available in modern science.
Lifespan Extension in Mice: A Historic Breakthrough
In 2009, the United States Interventions Testing Program (ITP) — one of the most demanding multi-site longevity testing programs in the world — published results that sent shockwaves through the scientific community. Rapamycin extended lifespan in male mice by 9% and in female mice by 14%. Science magazine named it one of the top ten scientific breakthroughs of that year.
What made the result even more remarkable was the timing. Treatment began at 600 days of age — roughly equivalent to a 60-year-old human. Rapamycin was the first drug ever demonstrated to extend mammalian lifespan when given late in life. Subsequent ITP testing confirmed the result across all three independent sites, cementing rapamycin's status as the gold standard of longevity pharmacology.
More recent animal research has expanded these findings considerably. Rapamycin has been shown to:
- Slow aging across the nervous, cardiovascular, and immune systems simultaneously
- Improve bone density and heart function in aged mice
- Increase grip strength and running capacity in rats
- Increase brain volume and blood flow in individuals genetically predisposed to Alzheimer's disease (APOE4 carriers) after just four weeks of treatment
What is the ITP? The Interventions Testing Program is a rigorous, multi-site US research initiative that tests potential longevity compounds under strict, standardized conditions across three independent laboratories simultaneously. A positive result from the ITP is considered among the strongest evidence available that a compound genuinely affects lifespan.
The mTOR–Muscle Connection: Why Aging Muscles Need Help
One of the most compelling applications of rapamycin for human health involves the aging of skeletal muscle — a process called sarcopenia.
What is sarcopenia? Sarcopenia is the progressive, age-related loss of muscle mass, strength, and function. Beginning around age 40, humans lose approximately 1% of muscle mass per year. Over decades, this leads to frailty, increased fall risk, loss of independent living, and significantly elevated mortality risk. Grip strength alone is a recognized independent predictor of longevity.
As we age, mTOR activity in muscle tissue becomes chronically elevated. Rather than cycling cleanly between growth and repair, the system gets stuck. Autophagy declines, damaged proteins accumulate inside muscle cells, and the muscle gradually loses its ability to maintain and renew itself. The result is the slow, relentless decline we call sarcopenia.
Rapamycin, by periodically suppressing this chronically overactive mTOR, may restore the cleanup cycle — allowing aging muscle cells to clear their debris and function more like younger cells. This is precisely the hypothesis that Dr. Stanfield's clinical trial is designed to test.
Buy Rapamycin online
Dr. Stanfield's Clinical Trial: The Details
In 2024, Dr. Brad Stanfield and Professor Matt Kaeberlein published a landmark clinical trial protocol in Springer Nature's Trials journal — one of the world's leading peer-reviewed clinical research publications. This study represents the first randomized, double-blind, placebo-controlled clinical protocol ever designed to evaluate the combined effect of rapamycin and structured exercise on muscle strength and endurance in older adults.
What does double-blind, placebo-controlled mean? This is the gold standard of clinical trial design. Neither the participants nor the researchers know who is receiving the actual drug and who is receiving an inactive placebo. This eliminates the placebo effect and researcher bias, ensuring that any measured outcomes are genuinely due to the intervention being studied.
Study Design at a Glance
Participants: 40 adults aged 65–85
Intervention: 6 mg of rapamycin or placebo, administered once weekly for 13 weeks, alongside a home-based resistance exercise program performed three times per week
Primary outcome: The 30-Second Chair Stand Test — how many times a participant can stand up from and sit back down on a chair within 30 seconds. This is a clinically validated, real-world measure of lower-body strength and fall risk.
Secondary outcomes: 6-minute walk test, handgrip strength, quality of life assessed via the SF-36 questionnaire
Exploratory outcomes: Biological age measured using DNA methylation-based epigenetic clocks; systemic inflammation measured via high-sensitivity C-reactive protein (hs-CRP)
What is an epigenetic clock? An epigenetic clock is a scientific tool that estimates a person's biological age — how old their cells appear at a molecular level — independent of their calendar age. It works by analyzing patterns of chemical modifications (called methylation) on DNA. If rapamycin shifts these markers toward a younger biological profile, it would be among the strongest human evidence yet that the drug genuinely slows aging at the cellular level.
The Synergy Hypothesis
The trial is built on a compelling two-phase biological logic. Exercise temporarily activates mTOR, driving muscle repair and adaptation. Rapamycin then suppresses mTOR, triggering autophagy and deep cellular cleanup. This alternating rhythm — activate, then clean — is hypothesized to produce muscle-preservation outcomes far superior to either exercise or rapamycin alone.
If confirmed, this finding would have enormous implications. Many older adults struggle to sustain high-intensity exercise programs. If rapamycin amplifies the benefit of even moderate exercise, it could dramatically lower the physical threshold required to maintain strength and independence into old age.
Timeline: Where the Research Stands Now
June 2024 — Protocol officially registered with the Australia New Zealand Clinical Trials Registry (ACTRN12624000790549)
October 2024 — Full peer-reviewed protocol published in Trials, Springer Nature
November 2024 — Dr. Stanfield confirms participant recruitment is complete
January 2025 — Target date for completion of data collection
2026 — Peer-reviewed publication of results expected; preliminary findings may be shared earlier on Dr. Stanfield's YouTube channel
The Broader Picture: Rapamycin Among Longevity Candidates
Dr. Stanfield has been unambiguous in his public writing and videos: most longevity supplements on the market today simply do not survive rigorous testing. The ITP has screened dozens of compounds over the years — the vast majority have shown no meaningful effect on lifespan.
Rapamycin is the glaring exception. It is one of only a handful of compounds — alongside acarbose and canagliflozin — that have demonstrated consistent, reproducible lifespan extension across all three ITP testing sites. That places it in extraordinarily rare scientific company.
Recent research has further expanded the case for rapamycin beyond muscle and lifespan. A 2025 study published in Alzheimer's & Dementia found that just four weeks of rapamycin treatment increased brain volume and blood flow in cognitively normal, middle-aged individuals carrying two copies of the APOE4 gene — a genetic profile associated with a 12-fold increased risk of Alzheimer's disease. These early results suggest rapamycin's benefits may extend across multiple organ systems simultaneously.
An Important Caution
Rapamycin is a prescription medication with a real side effect profile. Because it suppresses immune function, it is not appropriate for everyone and must only be considered under direct physician supervision following a thorough, individualized medical evaluation. Nothing in this article constitutes medical advice. Always consult a qualified healthcare professional before considering any prescription medication for off-label use.
Conclusion: A Pivotal Moment in Aging Research
Dr. Brad Stanfield's rapamycin trial represents something genuinely rare in modern medicine: a rigorously designed, independently funded, peer-reviewed human study that takes longevity science seriously without falling into the hype that surrounds so much of the field.
The results, expected in 2026, could provide the first robust human evidence that rapamycin — already proven to extend lifespan in mammals — can meaningfully slow the physical decline associated with aging. If the synergy hypothesis holds, we may be looking at a future where the combination of moderate exercise and a weekly pill helps older adults stay stronger, more independent, and biologically younger for longer.
That future is not a fantasy. It is a clinical trial, and the data is already being collected.

Get Rapamycin now
Frequently Asked Questions (FAQs)
What is rapamycin and what is it currently approved for? Rapamycin (sirolimus) is an FDA-approved prescription drug originally used to prevent organ transplant rejection and treat certain cancers. It is now being investigated as a potential longevity and anti-aging intervention in human clinical trials.
How does rapamycin work in the body? It inhibits a protein complex called mTOR, flipping cellular metabolism from "build mode" into "repair mode." This activates autophagy — the cell's internal cleanup system — which removes damaged proteins and cellular debris. This shift is believed to underlie many of rapamycin's anti-aging effects.
What exactly did Dr. Stanfield's trial test? The trial tested whether 6 mg of rapamycin taken once weekly, combined with a structured home exercise program three times per week, improves muscle strength and endurance in adults aged 65–85 over a 13-week period.
Has rapamycin been proven to extend human lifespan? Not yet in humans. In mice, it extended lifespan by 9–14% even when treatment began late in life — the first drug ever to achieve this in mammals. Dr. Stanfield's and other ongoing trials are the critical next step toward understanding human applicability.
What is sarcopenia and why is it a priority target? Sarcopenia is the age-related progressive loss of muscle mass and strength, beginning around age 40 at roughly 1% per year. It increases fall risk, reduces independence, and is independently associated with earlier death. It is one of the most clinically meaningful consequences of biological aging.
Why combine rapamycin with exercise rather than using either alone? The hypothesis is synergistic: exercise activates mTOR to trigger muscle repair, then rapamycin suppresses mTOR to activate cellular cleanup. This alternating cycle is expected to produce significantly better muscle-preservation results than either intervention could achieve independently.
Is rapamycin safe for older adults? Prior clinical trials have found intermittent, low-dose rapamycin to be generally well-tolerated in older adults. However, because it suppresses immune function, it carries real risks and must only be taken under direct physician supervision following individual medical assessment. It is not a supplement.
What is an epigenetic clock and why does the trial use one? An epigenetic clock measures biological age — how old a person's cells appear at the molecular level — based on DNA methylation patterns, independent of calendar age. The trial uses this tool to determine whether rapamycin plus exercise produces measurable biological rejuvenation, not just physical performance gains.
When will the trial results be published? Data collection was targeted for completion by January 2025. A peer-reviewed journal publication is expected around 2026. Dr. Stanfield may share preliminary findings earlier on his YouTube channel.
Could rapamycin become a mainstream anti-aging treatment? This trial is designed as a Phase 2a feasibility study — a stepping stone toward a larger Phase 3 trial of 400–500 participants. Positive results would meaningfully strengthen the case for rapamycin as a validated longevity intervention, though regulatory approval for this specific use remains a longer-term prospect.

















Sign in to leave a comment.