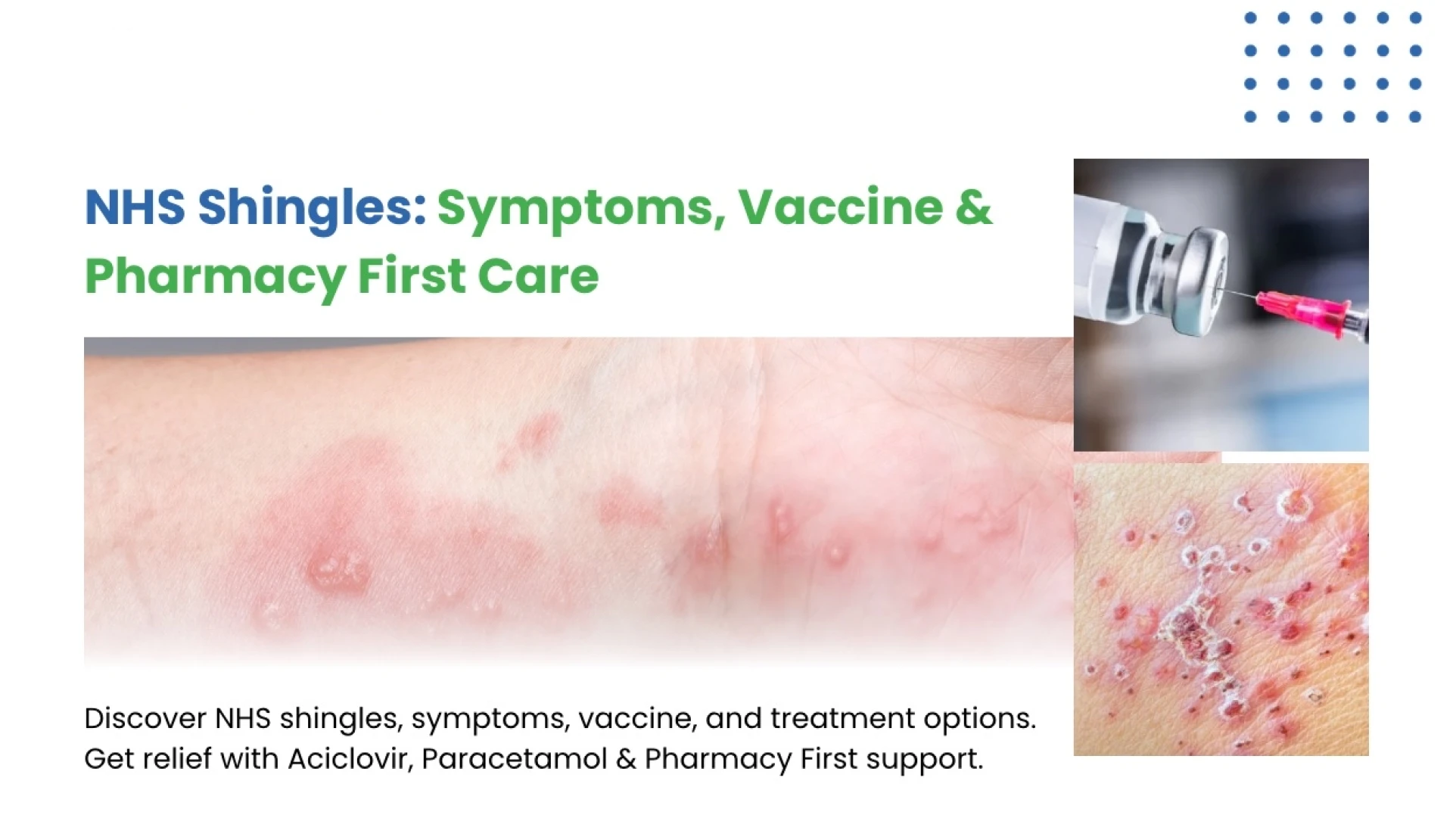
Shingles is a shocking condition that often leaves people in shock. It is also transmitted by the same virus that causes chicken pox, and even though most individuals undergo chicken pox only once in their lives, the virus is not expelled from the body. It also gets into the advances, where it manifests later in life as shingles. When patients in the UK look for help, they often search for NHS shingles services because these provide trusted guidance, treatment, and prevention options.
There is an insidious beginning of the infection, which can be felt by sensitivity or some tingling along one side of the body. A painful smattering of blisters immediately succeeds this. Although in the majority of instances a process passes within a couple of weeks, shingles may occasionally result in such complications as permanent nerve damage. The pain experienced physically, combined with the fear of having to cope with an unknown disease, implies that having access to quality care is critical.
This is why community health programs are relevant. It is possible to help people manage shingles in a timely and effective manner by making information, treatment, and vaccination widely available so that they can handle them.
Understanding How Shingles Develops
Once an individual recovers from chickenpox, the virus (varicella-zoster) does not go away. Rather, it gets stagnant within the nervous system. Years later, nhs shingles can reactivate, travelling along nerve fibres to the skin, producing the classic shingles rash.
Not all people who have contracted chicken pox will suffer shingles, although the risk increases with age and is comparatively high. Immunodeficient patients who have been exposed to medication, diseases, or stress factors can get attacked easily.
This is not one of the reasons why shingles is not merely a skin disorder, but it is what reminds one that viruses can rest unnotice, silently over decades before a reappearance.
Early Symptoms That Shouldn’t Be Ignored
Before the development of the rash, individuals tend to complain of an odd, frustrating, or itching sensation or anguish that occurs in an area of skin. After a few days, the red blotches will be followed by fluid-filled blisters. This rash comes in its tracks along the route of a nerve, taking a band-like form on only one side of the body.
Other symptoms can also be observed:
- Fatigue and general malaise
- Hypersabor in the locality.
- In a few instances, there is a fever or headache.
It is also important to identify these signs at the earliest stage since the treatment is best developed within a short period.
NHS Shingles: Pathways for Diagnosis and Care
In the case of the symptoms, the first step should be to contact a GP. The appearance of the rash and nerve pain can usually enable doctors to make a diagnosis of shingles. Additional tests can be requested in unusual situations where there is a doubt about the diagnosis.
The patients potentially obtain via its care pathway:
- The anti-viral prescriptions are used to manage the infection.
- Smoothing pain according to symptom severity.
- Recommendations on how to care for the skin to prevent secondary infection.
- Emergency referrals to specialists in case of any complication.
This can be done systematically to make sure that patients will not be left to treat painful symptoms without being counseled accordingly.
When Shingles Leads to Complications.
Despite the cases of most individuals recovering without professional complications in the long run, shingles poses a dilemma of problematic complications. Postherpetic neuralgia is the most widespread condition that is continuous nerve pain experienced for weeks or months after the rash disappears. This discomfort may disrupt rest, focus, and routine.
Other potential complications are:
- Eyes: Vision issues in the event of shingles on the eyes.
- In open blisters, secondary skin infections are possible.
- Uncommon neurological reactions, including brain or spinal cord inflammation.
Knowledge of such possibilities motivates people to turn to medical assistance early enough rather than letting the rash worsen.
NHS Shingles: The Role of Vaccination
Preventing shingles through immunization is one of the best alternatives when IT comes to decreasing the shingles burden. The NHS provides the shingles vaccine to some groups, especially older people who are especially vulnerable to the problems.
Although the vaccine does not provide total immunity, it greatly reduces the possibility of getting shingles, and when one does get shingles, the symptoms tend to be less severe and brief in duration. It also lowers the chances of post-herpetic neuralgia.
It is a preventive measure based on a broader target of what is in the field of health, i., ensuring that individuals have less effect when it comes to the influence of disease, not only of their own general health but also in the healthcare system as a whole.
Preventing Transmission to Others
Although shingles is not transmitted like the flu is, the virus has the potential to infect a person who has never had chickenpox, resulting in poor health. Because of this, it is more advisable for individuals with a case:
- Do not have close contact with pregnant women without chicken pox.
- Limit contact with infants and weakly immunised persons.
- Cover the rash with a cover until it forms crusts with blisters.
These measures are basic yet effective/important, particularly in defending the weak.
Long-Term Outlook and Lifestyle Choices
After the clearing of shingles, a larger number of individuals resume normal lives. Nevertheless, it can be that nerve pain persists and needs to be addressed. Precautionary regimes, including mild physical exercises, relaxation, and constant medical care, may assist patients to comfortably coexist with their persistent symptoms.
The immune system can also be boosted by building healthy habits, whether it be in stress management or physical activity, which will lessen the chances of contracting additional illnesses.
NHS Shingles: A Public Health Perspective
In a broader perspective, shingles is not a single issue. It is a great burden on the healthcare resources, especially with an aging population. Through enhancing her vaccination programmes, availing antiviral, and pain management, the NHS lowers the cost of administration and consequences of sickness in particular persons and in healthcare in general.
The antivirals are most effective during the critical window of treatment of patients, and it is through those campaigns conducted in the population that individuals are encouraged to do it early.
Looking Ahead for Patients and Communities
Shingles is a costly condition to live with, and with the right combination of medical assistance, personal care, and belief in prevention, the condition gets easier to heal. The NHS remains a key ingredient in ensuring that patients can access what they require, whether an antiviral medication, among others.
On the personal level, the meaning is simple and straightforward: pay attention to the warning signs, act immediately, and address the available preventive resources. To society, this becomes just as important as it aims to minimize the burden of shingles in general and make people live healthier as long as possible.













Sign in to leave a comment.