Living with chronic back pain can feel absolutely overwhelming and exhausting. Every movement becomes a calculated decision, and simple daily tasks transform into significant challenges. When conservative treatments like physical therapy and medications stop providing relief, many people face a critical crossroads in their healthcare journey.
The question then becomes whether to pursue non-invasive options or consider surgical intervention. Understanding the fundamental differences between these approaches helps patients make informed decisions. Your spine health deserves careful consideration and thoughtful evaluation of all available options.
Understanding Your Spinal Condition
The human spine consists of vertebrae, discs, nerves, and supporting tissues. When these structures become compressed or damaged, debilitating symptoms often follow quickly. Herniated discs, spinal stenosis, and degenerative disc disease represent common culprits.
Nerve compression creates pain that radiates down your legs or arms. Numbness, tingling, and weakness frequently accompany these uncomfortable sensations throughout your body. Some patients experience difficulty walking or maintaining balance during normal activities.
Accurate diagnosis requires comprehensive evaluation by qualified healthcare professionals with specialized training. Imaging studies like MRI scans reveal the exact location and severity. Your medical history and physical examination provide crucial context for treatment planning.
What Non-Surgical Decompression Involves
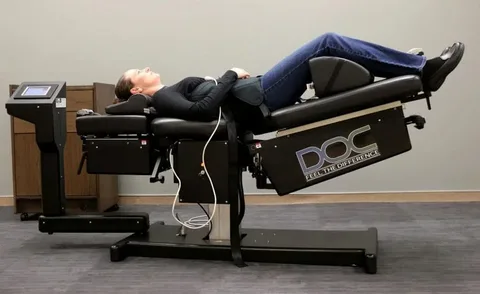
Spinal decompression treatment uses mechanical traction to gently stretch the spine carefully. This process creates negative pressure within the affected discs over time. The goal involves reducing pressure on compressed nerves and promoting healing.
Patients lie comfortably on a specialized table during treatment sessions typically. The equipment applies controlled force to specific areas of your spine. Sessions usually last between twenty and forty-five minutes per appointment.
Most treatment plans require multiple sessions spread over several weeks consistently. The gradual approach allows tissues to adapt and heal without trauma. Many patients report feeling relief after just a few initial sessions.
This conservative method carries minimal risks compared to invasive surgical procedures. Side effects remain rare and typically involve mild soreness afterward temporarily. Most people return to normal activities immediately following each treatment session.
The Surgical Approach Explained
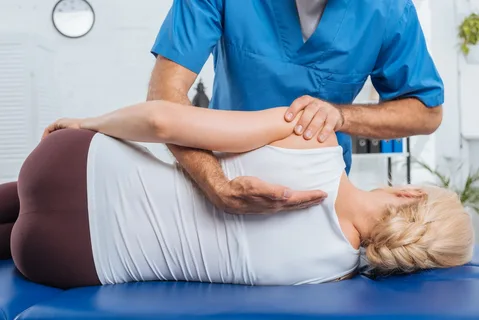
Spinal surgery becomes necessary when conservative treatments fail to provide relief. Procedures like laminectomy, discectomy, and spinal fusion address specific structural problems. Surgeons remove damaged tissue or stabilize unstable vertebrae during these operations.
Laminectomy involves removing part of the vertebra to create more space. This relieves pressure on the spinal cord and nerve roots effectively. Discectomy removes herniated disc material pressing against nerves in your spine.
Spinal fusion permanently joins two or more vertebrae together using hardware. This eliminates painful motion between damaged vertebrae in the affected area. The procedure provides long-term stability but reduces flexibility in that region.
These operations require general anesthesia and hospital stays ranging from overnight. Recovery periods extend from several weeks to several months depending fully. Physical therapy becomes essential for regaining strength and mobility after surgery.
Comparing Treatment Outcomes
Non-surgical decompression shows effectiveness for many patients with specific conditions appropriately. Studies indicate success rates ranging from seventy to ninety percent overall. Patients with herniated discs and stenosis often respond particularly well.
The benefits accumulate gradually as treatment progresses over multiple weeks consistently. Pain reduction, improved mobility, and better quality of life emerge progressively. Some patients achieve complete resolution while others experience significant improvement.
Surgical outcomes vary based on the specific procedure and individual factors. Success rates for properly selected candidates reach eighty to ninety percent. However, results depend heavily on patient selection and surgical technique.
Some patients experience immediate relief following successful surgical intervention in hospitals. Others require extended recovery periods before noticing substantial improvements in symptoms. Complications, though uncommon, can include infection, bleeding, or nerve damage.
Recovery Time Considerations
Non-surgical treatment allows patients to maintain relatively normal schedules throughout care. Most people continue working and managing daily responsibilities without significant interruption. The gradual nature means no extended downtime or recovery period.
Minor discomfort may occur initially as your body adjusts to treatment. This typically resolves within a day or two after sessions. No special restrictions apply to most everyday activities between appointments.
Surgical recovery demands significantly more time away from work and activities. Initial hospital recovery lasts anywhere from one to several days. Returning to desk work might take four to six weeks.
Physical labor positions require three to six months before full duty. Lifting restrictions, activity limitations, and rehabilitation exercises dominate the recovery phase. Some patients never regain full pre-surgery function despite successful operations.
Cost Analysis
Non-surgical decompression typically costs less than surgical interventions when comparing directly. Treatment packages range from a few thousand to several thousand. Insurance coverage varies widely depending on your specific plan and provider.
Many clinics offer payment plans to make treatment more accessible. The absence of hospital fees, anesthesia costs, and surgical expenses. This makes the overall financial burden considerably lighter for most families.
Spinal surgery expenses can reach tens of thousands of dollars easily. Hospital charges, surgeon fees, anesthesia, and imaging studies accumulate rapidly. Post-operative care, medications, and rehabilitation add substantial additional costs.
Insurance generally covers medically necessary surgical procedures after prior authorization approval. However, deductibles and co-insurance mean significant out-of-pocket expenses remain common. Lost wages during extended recovery periods represent another financial consideration.
Evaluating Your Risk Factors
Non-surgical approaches carry minimal risk for most patients seeking relief safely. The main contraindications include pregnancy, fractures, tumors, and severe osteoporosis. Advanced imaging rules out these conditions before treatment begins typically.
Temporary soreness represents the most common side effect patients report experiencing. Serious complications from non-surgical decompression remain extremely rare in practice. The reversible nature means stopping treatment carries no lasting consequences.
Surgery inherently carries higher risks due to its invasive nature always. General anesthesia complications, though rare, can include serious adverse reactions. Surgical site infections occur in approximately one to three percent.
Nerve damage, blood clots, and chronic pain represent potential serious complications. Failed back surgery syndrome affects ten to forty percent of patients. Adjacent segment degeneration may require additional surgeries years later eventually.
Making Your Decision
Your specific diagnosis plays the most critical role in determining suitability. Some conditions respond better to conservative care while others require surgery. Consulting with multiple specialists provides valuable perspectives on your unique situation.
Consider your overall health status, age, and personal treatment goals carefully. Younger patients might prefer preserving surgical options for later if possible. Older patients with multiple health issues may favor less invasive approaches.
Quality of life considerations matter tremendously in this important healthcare decision. Some people cannot afford extended recovery periods due to responsibilities. Others prioritize avoiding surgery unless absolutely medically necessary for survival.
Research providers thoroughly, checking credentials, experience, and patient reviews extensively online. Ask detailed questions about success rates, potential complications, and alternatives. Trust your instincts about the healthcare professionals guiding your care.
Finding the Right Path Forward
Both surgical and non-surgical options offer valid pathways toward pain relief. The right choice depends entirely on your individual circumstances and needs. Many patients successfully avoid surgery by pursuing conservative treatments first diligently.
Starting with less invasive options makes sense for most people initially. This preserves surgical intervention as a backup if needed later. Progressive treatment approaches maximize healing potential while minimizing unnecessary risks.
Working closely with experienced healthcare providers ensures appropriate care selection always. Regular communication about symptoms, progress, and concerns remains essential throughout treatment. Your active participation in the decision-making process leads to better outcomes.
Remember that back pain management often requires patience and persistence consistently. Quick fixes rarely exist for complex spinal conditions causing chronic pain. Committing to your chosen treatment path gives it the best chance.


















Sign in to leave a comment.