In today’s evolving healthcare ecosystem, the Social Determinants of Health (SDOH) are emerging as the most vital indicators of patient well-being. Traditional clinical metrics like lab tests or vitals only tell half the story. The unseen half — where patients live, work, and eat — profoundly shapes their health outcomes. Understanding and capturing this invisible data is where modern care gains its greatest power.
The concept of SDOH bridges the medical world with the real world. It reveals how everyday conditions—such as housing, transportation, employment, and food access—impact the success of clinical care. When health teams actively collect and use this data, they gain insights that guide both personalized treatment and system-wide improvement.
Why SDOH Defines Modern Healthcare
Health outcomes no longer hinge solely on medical expertise or hospital resources. Instead, they depend on the social and environmental factors that influence daily life. For instance, a patient might have access to the best diabetes treatment, yet lack transportation to refill their prescriptions or access to nutritious food to maintain proper glucose levels.
Understanding SDOH allows clinicians to:
- Identify underlying risks: From unsafe housing to job instability, identifying early warnings helps clinicians prevent health crises.
- Build realistic care plans: Knowing a patient’s daily challenges leads to achievable, sustainable treatment goals.
- Improve patient trust: When care teams acknowledge social struggles, patients feel seen, respected, and engaged.
- Reduce avoidable hospital visits: Proactive SDOH awareness prevents escalation of minor issues into emergency cases.
This holistic view is revolutionizing patient care — not through high-tech devices, but through high-context understanding.
The Dimensions of SDOH: Beyond the Medical Chart
To harness the full potential of SDOH, healthcare teams focus on seven core categories that paint a complete picture of a patient’s life:
- Housing Stability: Frequent relocations or unsafe conditions can derail recovery and medication adherence.
- Food Security: Access to nutritious food affects chronic disease management and overall energy levels.
- Transportation: Lack of reliable transport leads to missed appointments and medication lapses.
- Employment and Income: Financial strain and irregular work hours limit follow-up care.
- Education and Health Literacy: Patients may struggle to interpret medical instructions or use digital health tools.
- Social Support Networks: Isolation can worsen both mental and physical conditions.
- Neighborhood Safety: Unsafe environments restrict physical activity and amplify stress levels.
Together, these data points tell clinicians what lab results cannot — how life circumstances directly dictate health trajectories.
The Art and Science of SDOH Data Collection
Collecting SDOH information requires both technical integration and empathetic communication. It’s not merely about adding new fields to an Electronic Health Record (EHR); it’s about building trust and efficiency into every patient interaction.
Modern collection methods include:
- Standardized Screening Tools: Instruments like PRAPARE or AHC-HRSN ensure consistent data gathering across populations.
- EHR-Integrated Workflows: Embedding SDOH fields into digital forms avoids duplication and streamlines staff duties.
- Nurse-Led Conversations: Nurses often uncover social risks through personal, extended dialogues.
- Self-Reported Surveys: Digital forms via portals or tablets encourage honest, stigma-free disclosure.
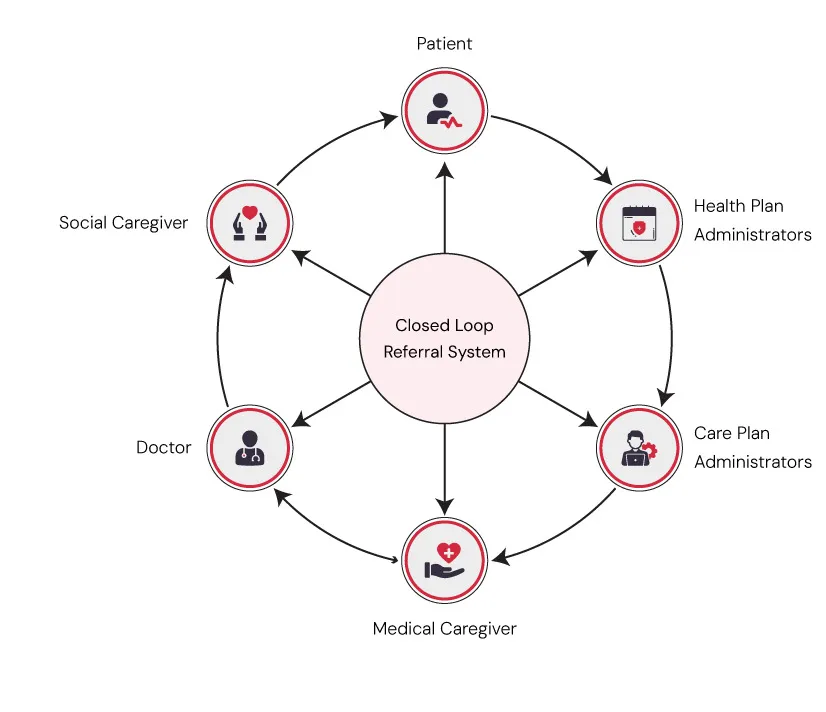
- Referral and Tracking Systems: These close the loop between identifying needs and ensuring patients receive actual support.
Each method contributes to an ecosystem of data-driven empathy—where technology meets human understanding.
The Challenges: Turning Data into Action
Even the best-intentioned healthcare systems face roadblocks when implementing SDOH strategies. Common issues include:
- Inconsistent Screening: Staff may skip questions during busy shifts, leading to incomplete profiles.
- Fragmented Data Storage: Scattered information across PDFs, spreadsheets, and EHRs reduces usability.
- Limited Training: Staff may lack skills for sensitive conversations about social hardships.
- Undefined Referral Processes: Identified needs often go unresolved due to workflow gaps.
- Lack of Follow-up Visibility: Clinics rarely track whether patients actually receive support after referrals.
Solving these challenges requires organizational alignment and clear data governance — not just digital tools.
The Payoff: Transforming Care Through SDOH Insights
When SDOH data is collected, shared, and analyzed effectively, the benefits ripple through every layer of care delivery.
- Predictive Care: Anticipating who might miss appointments or face complications allows proactive interventions.
- Operational Efficiency: Coordinated teams spend less time searching for information and more time delivering value.
- Compliance and Reporting: Accurate SDOH documentation enhances eligibility for value-based care programs.
- Community Partnerships: Reliable data fosters collaboration with food banks, housing agencies, and local nonprofits.
- Enhanced Patient Relationships: Care becomes more personalized, inclusive, and outcome-oriented.
In essence, strong SDOH systems convert data into compassion and insight into action.
The Digital Backbone: Technology Meets Humanity
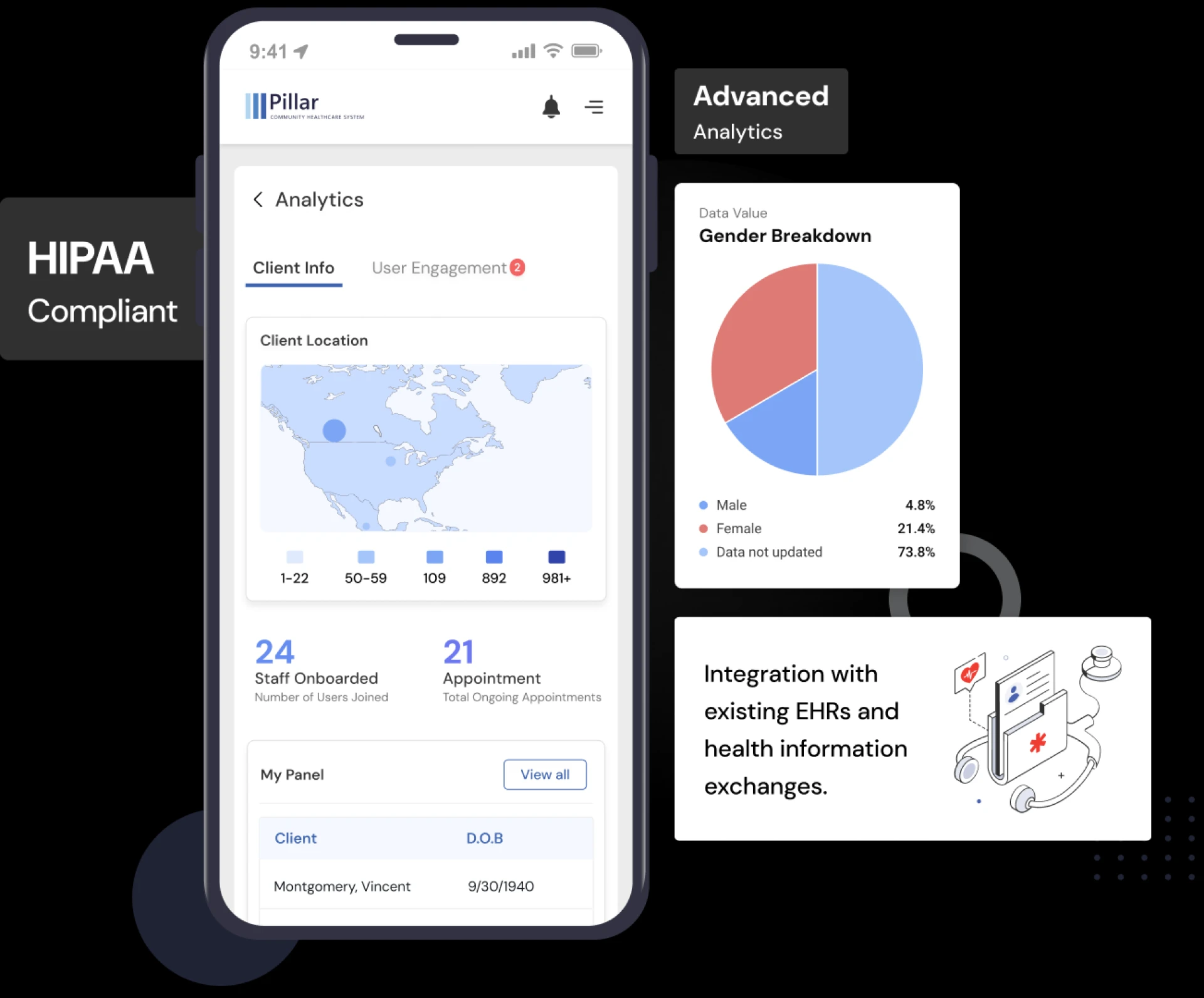
Tools like Pillar by SocialRoots.ai exemplify how technology can streamline this process. Their platform integrates SDOH assessments, referral tracking, and community coordination—all within a user-friendly interface. By combining automation with empathy, such solutions ensure no patient falls through the cracks.
For organizations seeking to implement or refine their SDOH strategies, adopting a structured, interoperable solution is no longer optional—it’s essential for sustainability.
Building the Future of Care: Collaboration and Trust
The evolution of SDOH frameworks depends not just on software, but on mindset shifts across the healthcare ecosystem. Administrators, clinicians, and social workers must all see social data as a core part of medical care. Patients, too, must feel confident that sharing this information leads to real-world benefits, not judgment or bureaucracy.
When healthcare embraces the full spectrum of human experience, care moves from reactive to preventive, from clinical to compassionate.
Conclusion: From Data Points to Life Stories
Ultimately, SDOH work reminds us that every patient is more than a chart — they’re a story of environment, opportunity, and resilience. By mastering SDOH integration, care teams unlock a new level of precision and empathy in healthcare delivery.
And as the industry moves toward equitable and patient-centered systems, the key lies in consistent, compassionate SDOH Data Collection — not as an administrative task, but as a bridge to understanding the full human condition.




Sign in to leave a comment.