Diabetic retinopathy is a serious eye condition that affects individuals with diabetes, potentially leading to vision loss if not addressed early. A diabetic retinopathy specialist plays a critical role in diagnosing and treating this condition to preserve vision and improve patients’ quality of life. This article explores the expertise of a diabetic retinopathy specialist, the diagnostic process, treatment options, and preventive measures to manage this sight-threatening disease.
Understanding Diabetic Retinopathy
Diabetic retinopathy is a complication of diabetes that damages the blood vessels in the retina, the light-sensitive layer at the back of the eye. High blood sugar levels weaken these vessels, causing them to leak fluid or bleed, which can distort vision. In advanced stages, abnormal blood vessels may grow on the retina, leading to severe complications like retinal detachment or glaucoma. Early detection and intervention by a diabetic retinopathy specialist are crucial to prevent irreversible damage.
This condition progresses through stages:
- Non-proliferative diabetic retinopathy (NPDR): Early stage with mild symptoms, such as microaneurysms or small hemorrhages in the retina.
- Proliferative diabetic retinopathy (PDR): Advanced stage where new, fragile blood vessels grow, increasing the risk of severe vision loss.
A diabetic retinopathy specialist, typically an ophthalmologist with advanced training in retinal diseases, is uniquely qualified to manage this condition through precise diagnostics and tailored treatments.
The Role of a Diabetic Retinopathy Specialist
A diabetic retinopathy specialist is a medical professional with expertise in diagnosing and treating retinal disorders, particularly those caused by diabetes. These specialists undergo extensive training, including medical school, residency in ophthalmology, and often a fellowship in vitreoretinal surgery or medical retina. Their deep understanding of the retina and its associated conditions allows them to provide comprehensive care for diabetic retinopathy patients.
The specialist’s role includes:
- Conducting thorough eye examinations to detect early signs of retinopathy.
- Using advanced imaging technologies to assess retinal damage.
- Developing personalized treatment plans based on the severity of the condition.
- Collaborating with endocrinologists and primary care physicians to manage underlying diabetes.
- Educating patients on lifestyle changes to prevent disease progression.
By leveraging cutting-edge tools and techniques, a diabetic retinopathy specialist ensures accurate diagnosis and effective management of the condition.
Diagnostic Process for Diabetic Retinopathy
Diagnosing diabetic retinopathy requires a combination of clinical evaluations and advanced imaging. A diabetic retinopathy specialist employs a systematic approach to assess the retina and determine the extent of damage. Below are the key steps in the diagnostic process:
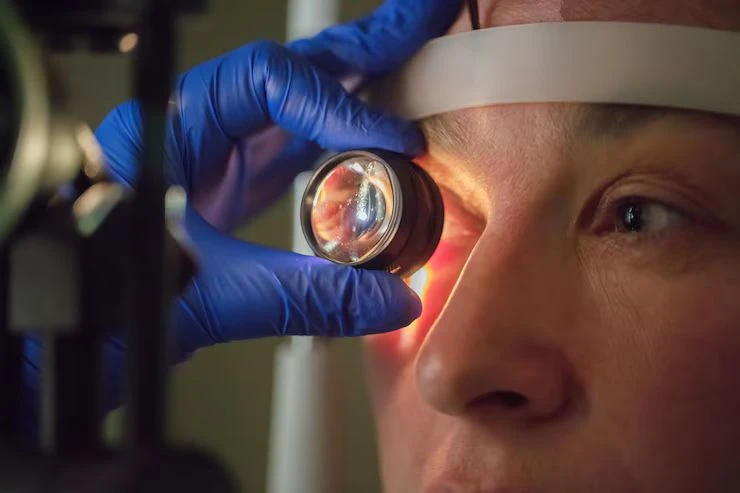
1. Comprehensive Eye Examination
The specialist begins with a detailed eye exam to evaluate overall eye health. This includes:
- Visual Acuity Test: Measures how well the patient can see at various distances using an eye chart.
- Dilated Eye Exam: The specialist uses eye drops to dilate the pupils, allowing a clear view of the retina and optic nerve. This helps identify abnormalities like swelling (macular edema) or hemorrhages.
- Tonometry: Measures intraocular pressure to rule out glaucoma, which can accompany diabetic retinopathy.
2. Fundus Photography
Fundus photography captures detailed images of the retina. The diabetic retinopathy specialist uses these images to identify microaneurysms, hemorrhages, or abnormal blood vessels. This non-invasive technique provides a baseline for monitoring disease progression.
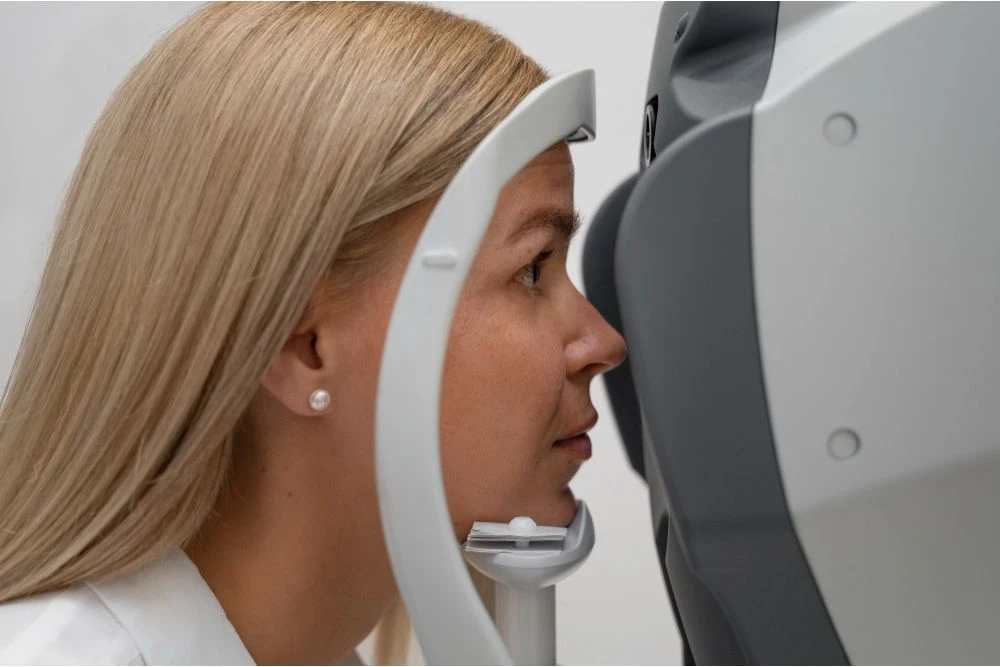
3. Optical Coherence Tomography (OCT)
OCT is a critical tool for diagnosing diabetic retinopathy. This imaging technique creates high-resolution, cross-sectional images of the retina, allowing the specialist to detect macular edema or retinal thickening. OCT helps the diabetic retinopathy specialist assess the severity of the condition and guide treatment decisions.
4. Fluorescein Angiography
In cases of suspected proliferative diabetic retinopathy, the specialist may perform fluorescein angiography. A dye is injected into the patient’s arm, which travels to the retinal blood vessels. A series of photographs captures the dye’s movement, highlighting leaks or abnormal vessel growth. This test helps the diabetic retinopathy specialist pinpoint areas requiring treatment.
5. Medical History Review
The specialist reviews the patient’s medical history, focusing on diabetes duration, blood sugar control, and other risk factors like hypertension or high cholesterol. Poorly controlled diabetes increases the likelihood of retinopathy, guiding the specialist’s diagnostic and treatment approach.
By combining these methods, a diabetic retinopathy specialist can accurately diagnose the condition and determine its stage, enabling timely intervention.
Treatment Options for Diabetic Retinopathy
Once diagnosed, diabetic retinopathy is managed through a combination of medical interventions, lifestyle changes, and, in some cases, surgical procedures. A diabetic retinopathy specialist tailors treatment to the patient’s specific needs, considering the disease stage and overall health. Below are the primary treatment options:
1. Blood Sugar and Blood Pressure Control
Tight control of blood sugar and blood pressure is the cornerstone of diabetic retinopathy management. A diabetic retinopathy specialist works closely with the patient’s primary care team to optimize diabetes management. This may involve:
- Adjusting insulin or oral medications.
- Monitoring HbA1c levels to ensure blood sugar remains within target ranges.
- Managing hypertension with medications or lifestyle changes.
Effective diabetes control can slow or halt the progression of retinopathy, especially in the early stages.
2. Anti-VEGF Injections
For patients with macular edema or proliferative diabetic retinopathy, anti-vascular endothelial growth factor (anti-VEGF) injections are a common treatment. These medications, such as ranibizumab or aflibercept, reduce abnormal blood vessel growth and leakage. The diabetic retinopathy specialist administers these injections directly into the eye, typically under local anesthesia. Regular injections may be required to maintain results.
3. Laser Therapy
Laser treatments, such as focal laser therapy or panretinal photocoagulation, are used to manage diabetic retinopathy. Focal laser therapy targets specific leaking blood vessels, while panretinal photocoagulation reduces abnormal vessel growth in proliferative retinopathy. The diabetic retinopathy specialist uses precise laser techniques to stabilize the retina and prevent further damage.
4. Corticosteroid Injections
In cases where anti-VEGF injections are insufficient, corticosteroid injections or implants may be used to reduce inflammation and swelling in the retina. These treatments are carefully monitored by the diabetic retinopathy specialist to minimize side effects, such as increased intraocular pressure.
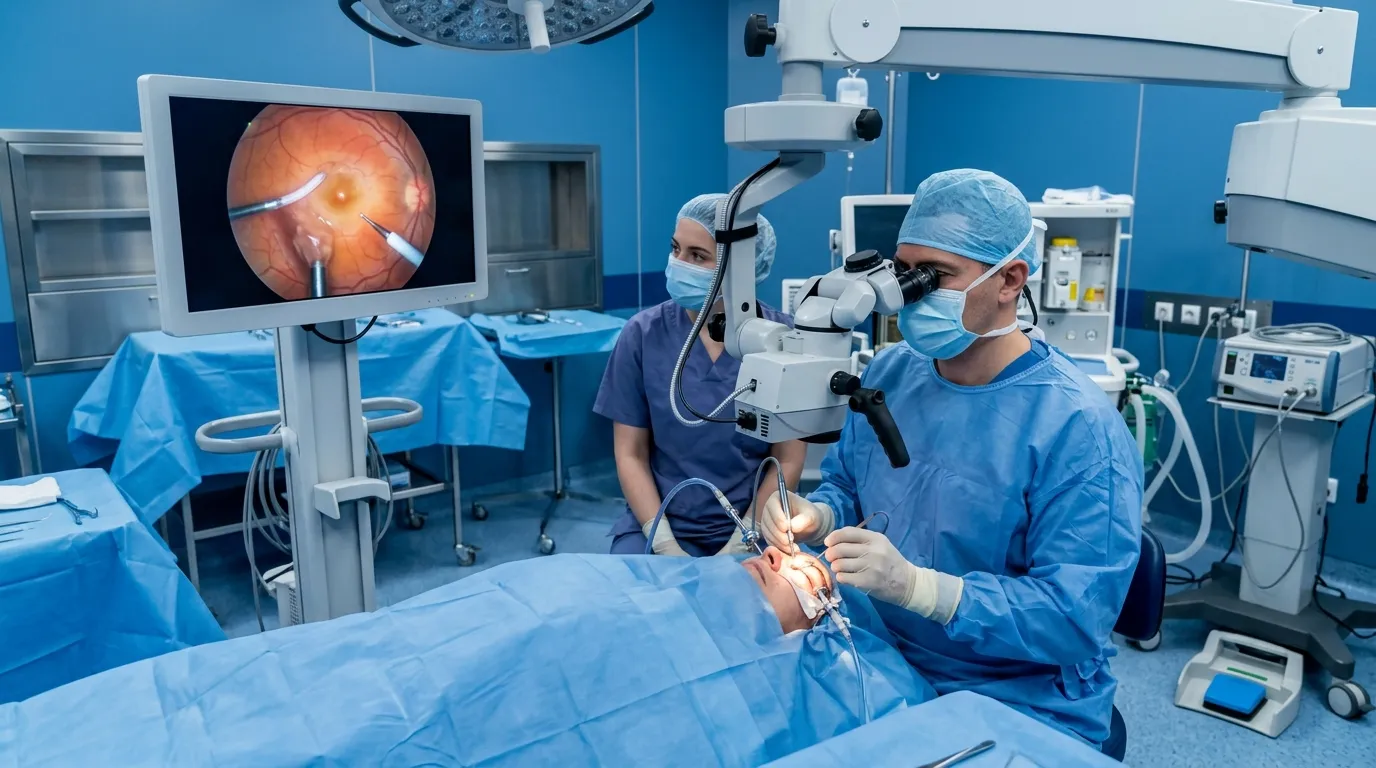
5. Vitrectomy
For advanced cases involving severe bleeding or retinal detachment, a diabetic retinopathy specialist may recommend vitrectomy. This surgical procedure removes blood and scar tissue from the vitreous (the gel-like substance in the eye) to restore vision and prevent further complications. Vitrectomy is typically reserved for severe proliferative diabetic retinopathy.
6. Ongoing Monitoring
Even after treatment, regular follow-ups with a diabetic retinopathy specialist are essential. The specialist monitors the retina for changes, adjusts treatments as needed, and ensures the patient maintains optimal diabetes control.
Preventive Measures and Patient Education
Prevention is a key focus for a diabetic retinopathy specialist. By educating patients on risk factors and lifestyle modifications, specialists empower individuals to protect their vision. Key preventive strategies include:
- Regular Eye Exams: Annual or biannual screenings to detect early signs of retinopathy.
- Healthy Diet: A balanced diet rich in fruits, vegetables, and whole grains to support blood sugar control.
- Physical Activity: Regular exercise to improve circulation and manage diabetes.
- Smoking Cessation: Quitting smoking to reduce vascular damage.
- Medication Adherence: Following prescribed diabetes and hypertension treatments.
A diabetic retinopathy specialist also educates patients about the importance of monitoring symptoms, such as blurred vision, floaters, or sudden vision loss, and seeking immediate care if these occur.
The Importance of Early Intervention
Early detection and treatment by a diabetic retinopathy specialist can significantly reduce the risk of vision loss. Studies show that timely intervention can prevent up to 90% of severe vision loss in diabetic retinopathy patients. Regular screenings, especially for those with long-standing diabetes or poor blood sugar control, are critical to catching the disease in its early, more manageable stages.
Choosing the Right Diabetic Retinopathy Specialist
Selecting a qualified diabetic retinopathy specialist is essential for effective care. Patients should look for:
- Board certification in ophthalmology with a subspecialty in retinal diseases.
- Experience in treating diabetic retinopathy using advanced diagnostic and therapeutic techniques.
- A collaborative approach, working with other healthcare providers to address systemic health issues.
- Access to state-of-the-art imaging and treatment facilities.
Referrals from primary care physicians or endocrinologists can help identify a trusted specialist. Patient reviews and credentials can also guide the decision-making process.
Conclusion
Diabetic retinopathy is a complex condition that requires specialized care to preserve vision and prevent complications. A diabetic retinopathy specialist plays a pivotal role in diagnosing the disease through advanced imaging and comprehensive exams, offering treatments ranging from lifestyle interventions to surgical procedures. By prioritizing early detection, personalized treatment, and patient education, these specialists help patients manage diabetic retinopathy effectively. For individuals with diabetes, regular eye exams and collaboration with a diabetic retinopathy specialist are vital steps toward maintaining healthy vision and a high quality of life.















Sign in to leave a comment.