Surgery fixes the structural problem. What happens after is what determines how well you actually recover.
That's not an exaggeration. Two patients can have identical procedures and end up with very different outcomes at six months — and the difference is almost always in the quality and consistency of their post-operative rehabilitation.
Post surgical physiotherapy in Noida has become an essential part of surgical care precisely because surgeons and patients alike have seen what happens when recovery is left to chance versus when it's guided properly. The results aren't even close.
This article explains how post-surgical physiotherapy works, why timing matters, what the process looks like for common procedures, and how to give yourself the best possible chance of a full, fast recovery.
Why Surgery Alone Isn't Enough
A successful operation creates the conditions for recovery. It doesn't deliver recovery on its own.
After surgery, your body goes through a predictable healing sequence — inflammation, tissue repair, remodeling. During this process, muscles weaken from disuse, joints stiffen from immobilization, scar tissue forms and can restrict movement, and the nervous system adapts to protect the area. These are normal biological responses. Left unmanaged, they become obstacles.
Without structured rehabilitation, patients often plateau well short of their potential. They regain some function but not full strength. They move differently than they did before — guarding, compensating — and those patterns can persist for years and create secondary problems.
Physiotherapy manages the healing process actively. It guides tissue loading at each stage, prevents the complications that slow recovery, and progressively rebuilds the strength and movement that surgery can't restore on its own.
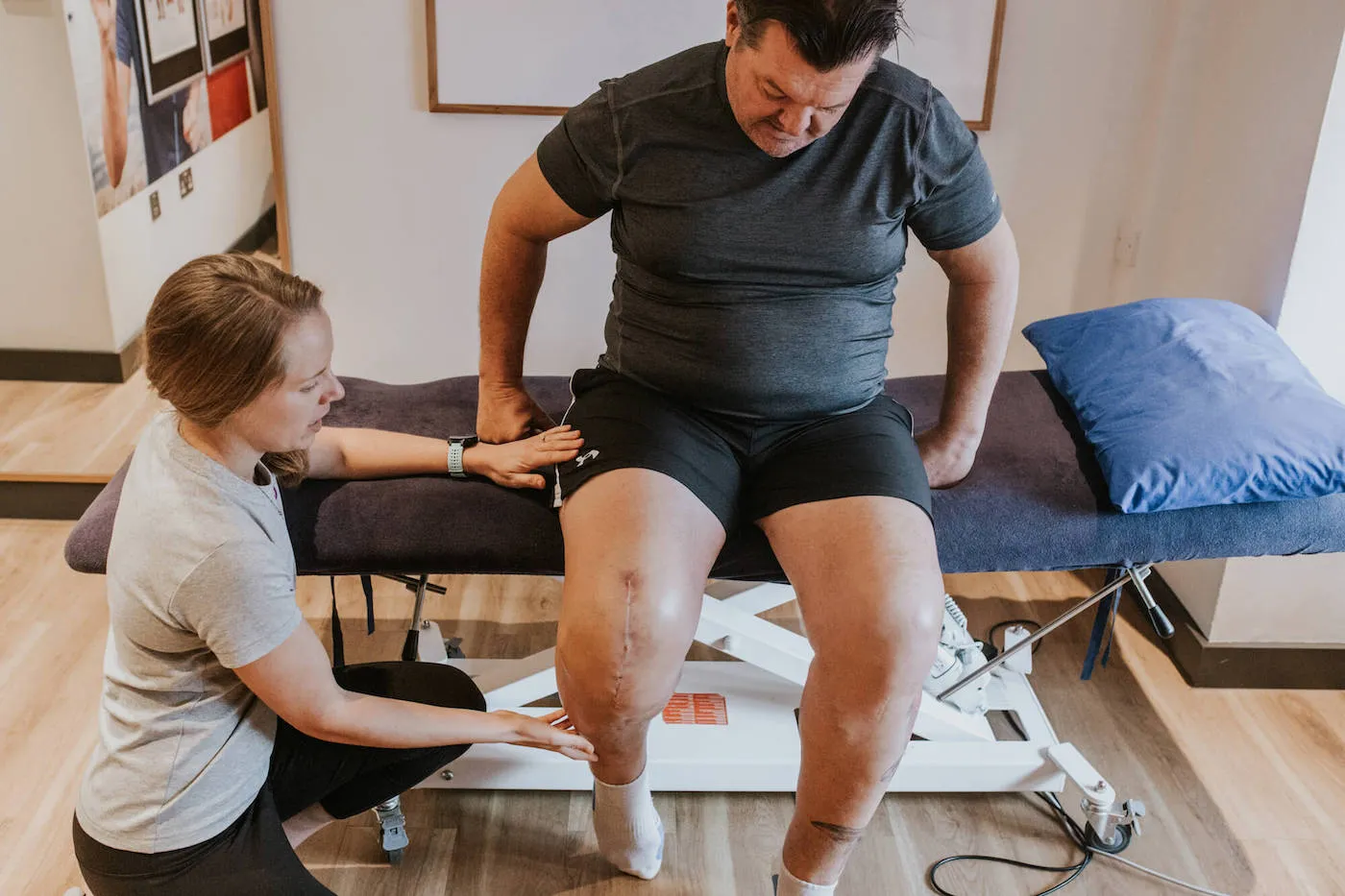
The Phases of Post Surgical Physiotherapy
Phase 1 — Early Post-Operative (Days 1–2 Weeks)
The goal in this phase isn't strength. It's protection and early activation.
Swelling and pain management come first — through positioning, ice, compression, and gentle movement that promotes circulation without stressing healing tissue. Early weight-bearing or range of motion work begins here, within the specific parameters the surgeon has set.
This phase also addresses something often overlooked: muscle inhibition. After surgery, the nervous system effectively shuts down muscles around the operated area as a protective response. Even if the muscles aren't damaged, they don't fire properly. Gentle neuromuscular activation work begins this process of re-establishing normal muscle recruitment.
Starting physiotherapy early — even in the first 24–48 hours after some procedures — is associated with significantly better outcomes. It's not about pushing hard. It's about keeping the healing process moving in the right direction from the start.
Phase 2 — Intermediate Rehabilitation (Weeks 2–6)
This is where the real work begins. Swelling is reducing, tissue is healing, and the focus shifts to restoring range of motion and beginning progressive strength work.
Manual therapy — joint mobilization, scar tissue management, soft tissue work — plays a significant role in this phase. Scar tissue, if not managed early, can form adhesions that restrict movement and cause pain well beyond the initial recovery period. A physiotherapist works the scar tissue while it's still malleable, preventing restrictions from becoming permanent.
Strength training in this phase is carefully graded. Too much load too early risks the repair. Too little and you lose the window for optimal muscle rebuilding. Getting that balance right is exactly what an experienced physiotherapist does.
Phase 3 — Functional Rehabilitation (Weeks 6–12+)
By this stage, structural healing is largely complete and the focus shifts to functional recovery — restoring the movement patterns, strength levels, and endurance needed for real life.
What "functional" means depends entirely on the patient. For a 70-year-old recovering from a hip replacement, it means walking confidently on different surfaces, managing stairs, getting in and out of a car. For a 30-year-old athlete recovering from ACL reconstruction, it means returning to cutting, pivoting, and sport-specific movement under load.
The physiotherapy program in this phase is highly individualized. Generic protocols only take you so far. The final stretch of recovery — the part that gets you back to everything you want to do — requires a program built around your specific goals and demands.
Post Surgical Physiotherapy in Noida — Common Procedures and What Recovery Involves
Knee Replacement Rehabilitation
Total knee replacement is one of the most common orthopedic procedures, and post-surgical physiotherapy is not optional for a good outcome — it's fundamental.
In the first two weeks, the focus is on managing swelling, achieving basic range of motion targets (typically 0–90 degrees of flexion), and getting safe independent mobility with a walking aid. Quadriceps activation is a priority from day one — the quad shuts down dramatically after knee surgery and needs deliberate retraining.
By six weeks, most patients are working on walking without aids, managing stairs, and progressing strength work. By three months, a well-rehabilitated patient is typically driving, managing daily activities independently, and working toward full functional recovery.
Without proper physiotherapy, knee replacement patients often plateau around 90 degrees of flexion, develop a persistent limp, and struggle with stairs and uneven ground long-term. The surgery was successful — but the outcome isn't what it should have been.
ACL Reconstruction Recovery
ACL reconstruction has one of the longest and most demanding rehabilitation timelines in orthopedic surgery — typically 9–12 months to return to sport.
The extended timeline isn't arbitrary. Research is clear that returning to cutting and pivoting sport before 9 months significantly increases re-rupture risk. The graft needs time to undergo ligamentization — the biological process of becoming true ligament tissue — and the neuromuscular control needed for safe sport participation takes months of progressive training to rebuild.
A good ACL rehabilitation program at a quality physiotherapy clinic in Noida follows a criteria-based progression rather than a purely time-based one. You advance to the next phase when you meet specific strength, stability, and movement quality benchmarks — not just because a certain number of weeks have passed.
Shoulder Surgery Recovery — Rotator Cuff Repair
Rotator cuff repair is one of the more demanding post-surgical rehabilitation journeys because the repaired tendon needs significant protection in the early weeks while it heals, followed by a carefully graduated loading program to rebuild full strength.
The first 4–6 weeks typically involve immobilization in a sling with only pendulum exercises and passive motion permitted. This is frustrating, but the repair needs this window. Loading the tendon too early risks failure of the repair.
From 6–12 weeks, active range of motion work begins and the sling is progressively discontinued. Strengthening starts in earnest after 12 weeks and continues for 6–9 months for patients wanting full return to overhead activity or sport.
The physiotherapy in the final phase — rebuilding rotator cuff strength, scapular control, and dynamic shoulder stability — is what determines whether the repaired shoulder functions properly long-term.
Spinal Surgery Rehabilitation
Post-surgical physiotherapy after spinal procedures — lumbar discectomy, spinal fusion, laminectomy — requires particular care because the management of load on the spine is critical during healing.
Early mobilization is important. Patients who get moving carefully in the first days after spinal surgery have better outcomes than those who remain bed-bound. But the type and amount of movement matters enormously.
Core stabilization work, postural retraining, and a gradual return to activities of daily living are the cornerstones of spinal post-surgical rehab. The goal is a spine that's strong, well-controlled, and protected by muscles that are doing their job properly — not a spine that relies on guarding and restriction to stay out of pain.
The Best Physiotherapy Clinic in Noida — What Good Post-Surgical Care Looks Like
Not all physiotherapy is equal in quality, and for post-surgical rehabilitation specifically, the difference matters more than it does for general musculoskeletal complaints.
Close Coordination With Your Surgeon
Your physiotherapist needs to know exactly what was done in surgery, what the surgeon's specific precautions are, and what the timeline for progression looks like. A physiotherapy clinic operating without this information is working blind.
The best physiotherapy clinic in Noida for post-surgical care maintains active communication with surgical teams — either through direct referral relationships or through clear documentation protocols. Before your first physiotherapy session, your therapist should have reviewed the surgical report and any specific post-operative instructions.
Criteria-Based Progression, Not Just Time
Good post-surgical physiotherapy advances your program based on what your body is actually doing — not just how many weeks have passed since your operation.
Can you achieve the required range of motion before adding load? Is the swelling controlled before progressing exercise intensity? Does your single-leg strength reach the required threshold before you return to running? These criteria-based decisions produce better outcomes than calendar-based protocols.
One-on-One Time With a Qualified Physiotherapist
Post-surgical rehabilitation is not the right context for high-volume clinic models where patients rotate through exercise stations supervised by assistants. You need hands-on assessment, manual therapy, and clinical decision-making from a qualified physiotherapist at every session.
MotionRX structures post-surgical rehabilitation around this principle — one-on-one sessions with a qualified physiotherapist who knows your case, monitors your progress, and makes real-time adjustments based on how you're responding.
Practical Tips for a Faster, Better Post-Surgical Recovery
Start physiotherapy as early as your surgeon permits. Early mobilization — even simple things like ankle pumps and gentle range of motion work — prevents the complications that make later rehabilitation harder.
Do your home exercises. Clinic sessions are typically 2–3 times per week. What you do on the other days determines whether you progress or plateau. Take the home program seriously.
Manage swelling actively. Persistent swelling inhibits muscle function and slows recovery. Ice, compression, elevation, and movement within permitted ranges all help keep swelling under control.
Communicate with your physiotherapist about pain. Some discomfort during rehabilitation is normal and expected. Sharp pain, significant increases in swelling after exercise, or pain that doesn't settle within an hour of finishing — these need to be reported. Don't push through warning signals without flagging them.
Be patient with the timeline but don't use it as an excuse to reduce effort. Recovery takes the time it takes — but effort and consistency within that timeline determine the quality of the outcome. Showing up and doing the work matters.
Set functional goals, not just pain goals. "Being pain-free" is a starting point, not an endpoint. Tell your physiotherapist what you want to be able to do — what activities, what sports, what daily tasks — so the program is built toward real-life function, not just clinical metrics.
What Patients Commonly Get Wrong After Surgery
A few patterns come up repeatedly and are worth naming directly.
Stopping physiotherapy too early. Pain and basic mobility return before full strength and movement quality do. Many patients feel good at 6–8 weeks and conclude they're done. They're not — and stopping here often leads to the persistent weakness and compensatory patterns that cause problems years later.
Overdoing it early. The opposite problem. Pushing too hard in the protection phase because you feel impatient creates setbacks — increased swelling, pain flares, and occasionally re-injury. Trust the phased approach.
Not following precautions. Surgeons give post-operative precautions — weight-bearing restrictions, movement limits, sling protocols — for specific reasons. Ignoring them because you feel better than expected is how repairs fail.
Why MotionRX Approaches Post-Surgical Rehab Differently
MotionRX takes post-surgical physiotherapy seriously as a clinical specialty rather than a general service.
Every post-surgical patient receives a program built around their specific procedure, their surgeon's protocol, their personal goals, and their physical baseline. Progress is tracked objectively at regular intervals. The program evolves as the patient does.
That level of individualization is what produces the outcomes patients actually want — not just a cleared surgical site, but a body that works properly and a life they can fully return to.
Conclusion
Surgery changes what's possible. Post surgical physiotherapy in Noida determines whether you actually get there.
The patients who recover fastest and most completely aren't necessarily the ones who had the most technically perfect operations. They're the ones who took rehabilitation seriously — who started early, worked consistently, followed the program, and had a physiotherapist guiding them through each phase with clinical precision.
If you've had surgery or one is coming, find a physiotherapy clinic you trust and treat the rehabilitation with the same seriousness you gave to the surgical decision. That's where the real recovery happens.















Sign in to leave a comment.