Healthcare organizations are not held back by a lack of software. They are held back by software ecosystems that were never designed to evolve.
Most healthcare systems today run on legacy data vendors that combine storage, workflows, reporting, and integrations into tightly controlled platforms. While this structure once made sense, it now creates long-term rigidity that limits how data can be accessed, shared, and used.
The core issue is not functionality. It is dependency.
Why legacy healthcare systems become a bottleneck
Over time, healthcare organizations accumulate systems that are difficult to replace or modify. These platforms tend to:
- Lock data inside proprietary structures
- Limit interoperability with modern tools
- Require vendor involvement for even small changes
- Create fragmented data across departments
- Increase operational complexity instead of reducing it
What starts as an “all-in-one solution” gradually becomes a constraint on innovation.
As healthcare becomes more data-driven, this fragmentation directly impacts decision-making speed and clinical efficiency.
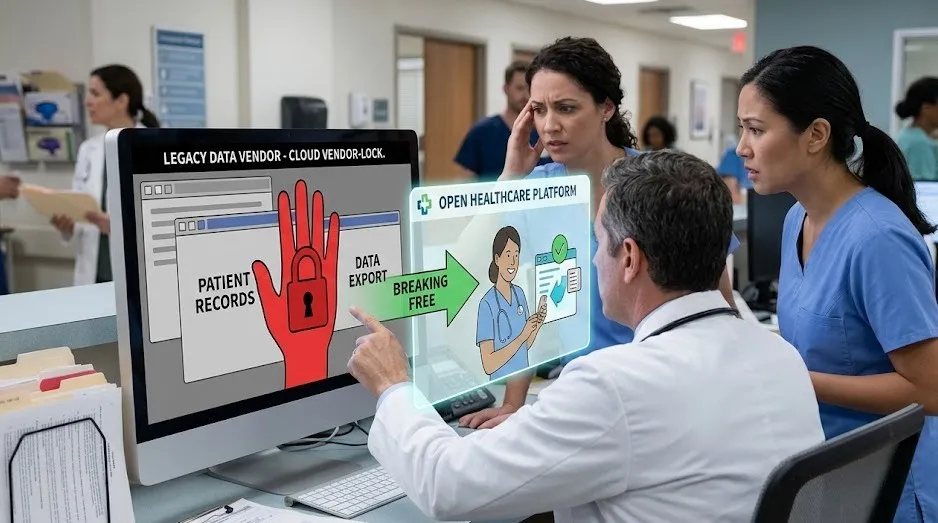
The hidden cost of vendor lock-in
Legacy healthcare data vendors often create ecosystems where data and applications are tightly coupled. This means:
- Data cannot be easily extracted or reused
- New tools require complex integration workarounds
- System upgrades are slow and expensive
- Organizations lose flexibility over time
The result is long-term dependency, where healthcare providers effectively operate within boundaries defined by the vendor rather than their own needs.
Why full system replacement rarely works
A common assumption is that modernization requires replacing legacy systems entirely.
In healthcare, this approach is often unrealistic.
Clinical environments require continuous uptime. Patient data must remain accessible at all times, and compliance requirements make large-scale migrations risky.
A full replacement introduces challenges such as:
- Operational disruption during migration
- High implementation cost and long timelines
- Risk of data loss or inconsistency
- Regulatory and compliance complexity
As a result, many organizations delay modernization even when existing systems clearly limit performance.
A more practical approach: decoupling data from systems
Instead of replacing everything at once, a more sustainable strategy is emerging.
The focus shifts from system replacement to data decoupling.
This involves:
- Extracting data from legacy platforms
- Centralizing it in independent data layers
- Exposing it through APIs
- Allowing new applications to operate on top of existing infrastructure
This approach enables modernization without interrupting ongoing clinical operations.
What changes when data is decoupled
Once healthcare data is no longer locked inside vendor systems, several improvements become possible:
1. Improved interoperability
Systems can communicate without heavy custom integration work.
2. Faster access to insights
Reporting and analytics are no longer constrained by legacy tools.
3. Enablement of modern technologies
AI, automation, and predictive analytics can operate directly on unified datasets.
4. Reduced vendor dependency
Organizations regain control over how their data is used and accessed.
Incremental modernization over disruption
Healthcare systems cannot afford sudden transformation. Change must be incremental and controlled.
A practical modernization path typically includes:
- Mapping existing systems and dependencies
- Identifying critical data sources
- Extracting and centralizing data step by step
- Introducing API-based access layers
- Gradually modernizing applications over time
This reduces operational risk while allowing continuous improvement.
The broader shift in healthcare architecture
Healthcare IT is gradually moving from monolithic platforms toward modular, data-centric architectures.
In this model:
- Data becomes independent of applications
- Systems become replaceable instead of permanent
- Integration becomes standardized
- Innovation happens without disrupting core operations
The focus shifts from owning software to controlling data flow and access.
Final perspective
Legacy healthcare data vendors are not just a technology challenge. They represent a structural limitation on how healthcare systems evolve.
Modernization does not require immediate replacement of existing systems. It requires removing the dependency barriers that prevent data from being used effectively.
Organizations that prioritize decoupling over replacement can modernize safely, maintain operational continuity, and regain long-term control over their data strategy.

















Sign in to leave a comment.