Rapamycin — originally developed for organ transplant patients — is now showing remarkable potential for cardiovascular health, reversing arterial stiffness, clearing cardiac cellular debris, and restoring heart function that aging has quietly eroded.
When it comes to rapamycin cardiovascular health, the science is pointing toward something genuinely exciting — a compound that does not simply manage heart disease symptoms but may actually reverse the biological aging of the heart and arteries. Originally approved by the FDA for organ transplant patients, rapamycin is now the most consistently studied geroprotector in preclinical cardiovascular research, delivering results that no traditional therapy has replicated.
Cardiovascular disease remains the world's leading cause of death — and its primary driver is not diet or lifestyle alone. It is aging itself. Long before symptoms appear, the heart quietly stiffens, accumulates cellular debris, and loses the youthful flexibility of its blood vessels. Rapamycin targets this process at its biological root.
"Rapamycin does not simply manage cardiovascular risk — growing evidence suggests it biologically reverses the aging of the heart and arteries."
Buy Rapamycin online
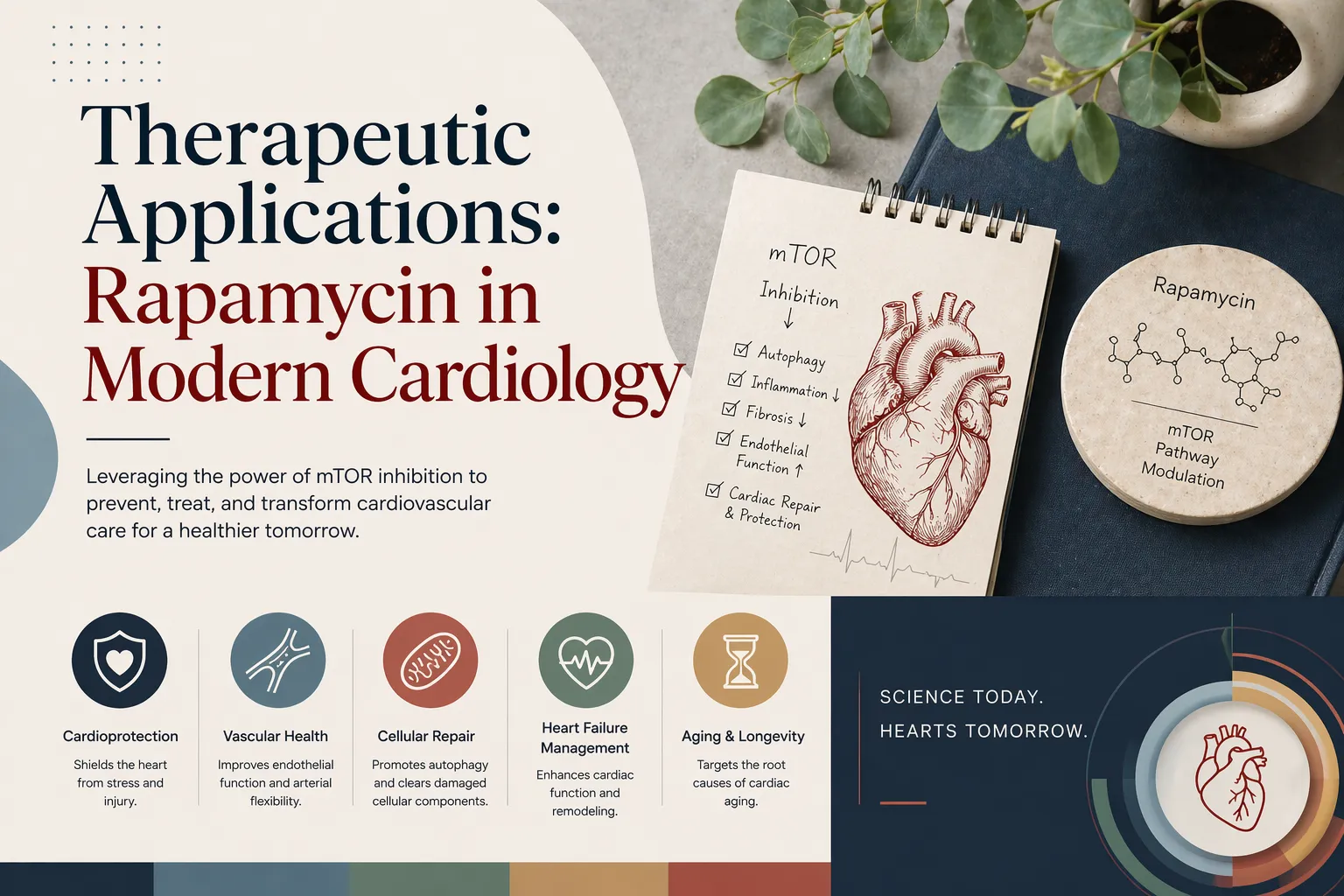
What Is Rapamycin and How Does It Work?
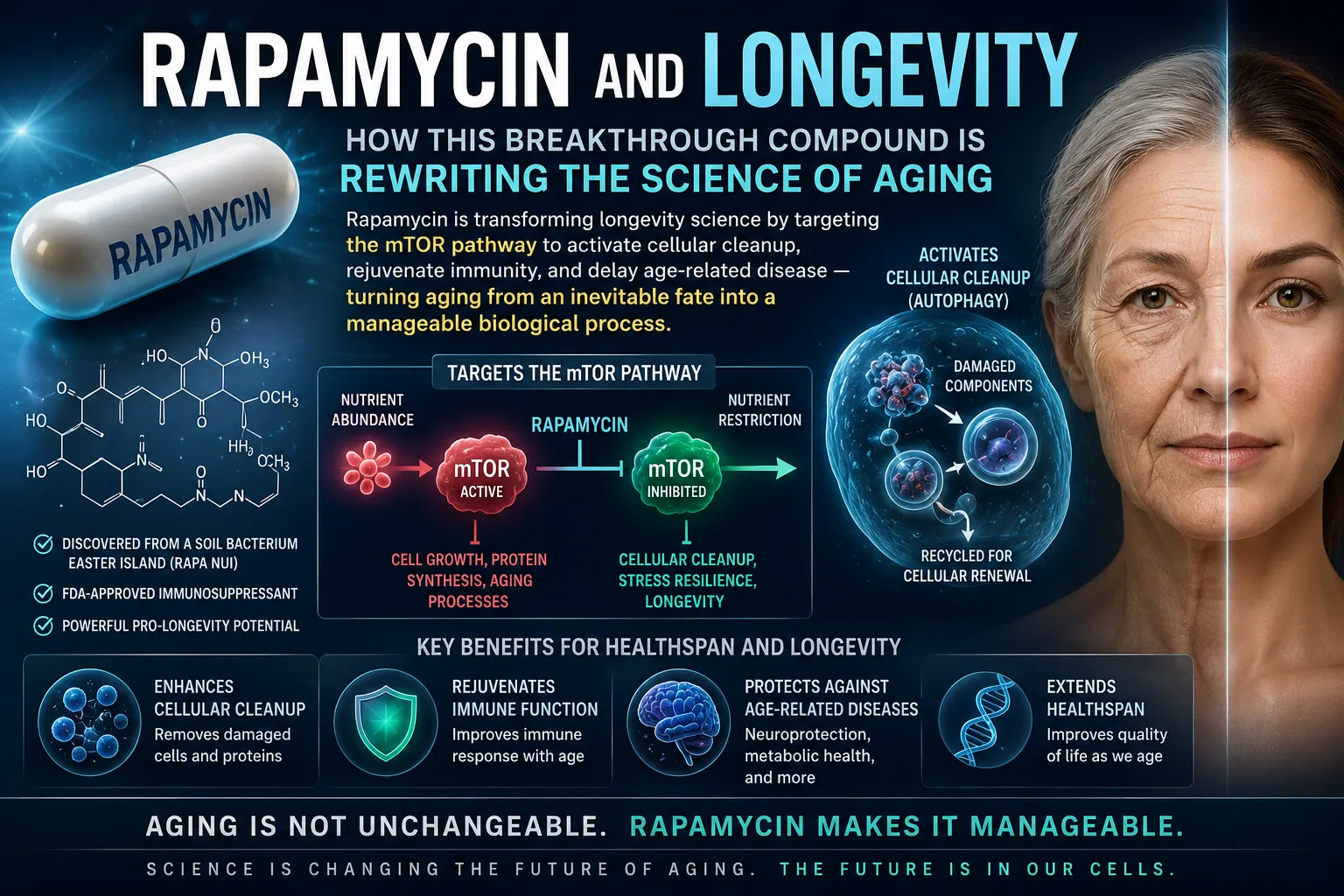
Rapamycin (also known as sirolimus) is an FDA-approved compound first discovered in soil bacteria from Easter Island in the 1970s. Its cardiovascular benefits stem from its ability to block a cellular pathway called mTOR — specifically the mTORC1 branch — which acts as a master growth switch inside your cells.
In youth, mTOR balances growth and repair beautifully. But as we age, mTORC1 becomes chronically overactivated — stuck in growth mode. Cells stop clearing damaged proteins and dysfunctional mitochondria. Inflammation quietly builds. Arterial walls stiffen. The heart thickens and loses the ability to relax properly between beats. Rapamycin corrects this by inhibiting mTORC1, flipping the switch back toward cellular repair — closely mimicking the proven longevity effects of caloric restriction.
Why Rapamycin Is Unique
Unlike blood pressure medications or statins — which manage individual risk factors — rapamycin targets the root biological mechanisms of cardiac aging: mTOR dysregulation, autophagy failure, and progressive vascular stiffening. No other approved drug does all three simultaneously.
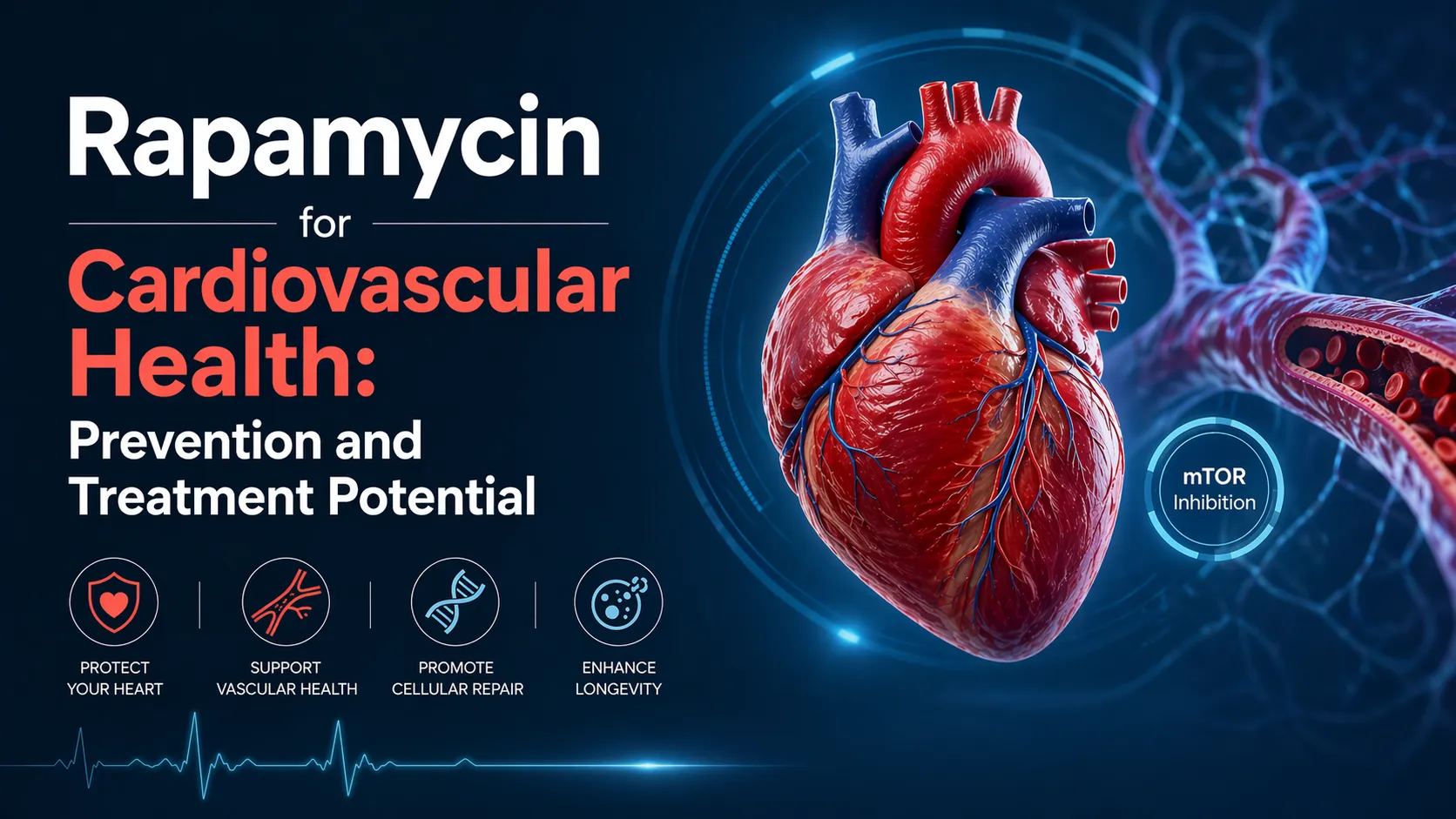
5 Powerful Ways Rapamycin Protects Your Heart
1.Autophagy activation
Triggers cellular "self-cleaning" — removing toxic debris, misfolded proteins, and damaged organelles from heart muscle cells.
2.Cardiac hypertrophy reversal
Regresses abnormal thickening of heart walls — even after it has already established itself.
3.Arterial flexibility restored
Reduces collagen buildup and AGE cross-links that make blood vessels stiff and unresponsive with age.
4.Nitric oxide boost
Improves nitric oxide availability, helping vessels dilate and reducing the heart's workload.
5.Plaque stabilisation
Enhances stability of arterial plaques, shrinks their necrotic cores, and inhibits foam cell formation.
The standout mechanism is autophagy. When mTORC1 is chronically overactive, autophagy is suppressed — and heart cells stop clearing the accumulated cellular "trash" that compromises their function. Rapamycin lifts that suppression, enabling a genuine housecleaning at the cellular level. It also triggers mitophagy, the removal of damaged mitochondria that would otherwise leak harmful reactive oxygen species into heart tissue.
The "Rapamycin Memory" Effect — Benefits That Last
One of the most striking discoveries in rapamycin cardiovascular research is that its benefits persist long after treatment ends. In aged mice, an 8-week course improved diastolic function and reduced myocardial stiffness — with those improvements remaining intact two full months after the last dose.
This "rapamycin memory" effect suggests the drug is biologically resetting the heart's aging program, not simply suppressing symptoms while being taken. It makes intermittent, low-dose strategies highly practical — and far more attractive than lifelong daily medication.
Human Trial Highlight
A pilot human study found that just 1 mg of rapamycin daily for 8 weeks produced measurable improvements in diastolic filling and endothelial function. Participants' hearts performed structurally and physiologically like those of people 10 to 15 years younger.
Buy Rapamycin now
Rapamycin vs. Traditional Heart Treatments
| Feature | Rapamycin | Traditional therapies |
|---|---|---|
| Primary goal | Biological rejuvenation | Symptom management |
| What it targets | mTOR pathway & autophagy | Blood pressure, cholesterol |
| Effect on aging | Directly reverses aging biology | No direct impact on aging rate |
| Duration of benefit | Persists after stopping treatment | Requires lifelong daily use |
| Clinical application | Already used in drug-eluting stents | Standard bare-metal stents |
Rapamycin and statins are not rivals — they are increasingly viewed as complementary. Statins excel at managing cholesterol and preventing thrombotic events. Rapamycin uniquely addresses the biological aging of the heart and vessels — reversing mTOR dysregulation, restoring autophagy, and reducing arterial stiffness — dimensions that statins simply do not reach.
What Human Evidence Shows So Far
The PEARL trial — currently the longest randomized controlled trial of rapamycin in healthy adults — confirmed that low-dose intermittent rapamycin is safe and well-tolerated in aging cohorts. A notable finding: women showed significantly greater improvements in lean muscle mass and quality of life than men, suggesting personalised protocols will matter going forward.
Ongoing trials including RESTOR (humans) and TRIAD (dogs) are further refining optimal dosing. The emerging consensus points to once-weekly low-dose protocols — typically 3 to 10 mg — a far safer approach than the high daily doses used in transplant medicine and with encouraging results across multiple cardiovascular markers.

Get Rapamycin now
Frequently Asked Questions About Rapamycin and Heart Health
FAQ
How does rapamycin cardiovascular health work at a cellular level?
Rapamycin inhibits the mTORC1 pathway, shifting heart cells away from chronic growth and inflammation toward repair and maintenance. The core mechanism is triggering autophagy — allowing heart muscle cells to finally clear out toxic proteins, damaged mitochondria, and cellular debris that accumulate and progressively impair cardiac function with age.
FAQ
Can rapamycin reverse arterial stiffness that already exists?
Preclinical research strongly suggests yes. Rapamycin modifies arterial wall composition — reducing collagen accumulation and the advanced glycation end-products (AGEs) that cause vessels to harden with age. Studies in older animals show restoration of arterial flexibility that closely resembles much younger vascular tissue.
FAQ
What exactly is the "rapamycin memory" effect?
This refers to the persistence of cardiovascular benefits long after treatment ends. Animal studies showed lasting improvements in diastolic function and reduced arterial stiffness for months beyond the final dose — suggesting rapamycin biologically resets the heart's aging program rather than simply suppressing symptoms while being taken.
FAQ
Is rapamycin better than statins for heart disease?
They are complementary rather than competing. Statins remain excellent for cholesterol management and preventing blood clots. Rapamycin uniquely targets the biological aging of the heart and arteries — reversing mTOR dysregulation, restoring autophagy, and reducing arterial stiffness — things statins do not address. Many researchers now advocate combining both for maximum cardiovascular benefit.
FAQ
Does rapamycin help with heart failure?
It shows significant promise, particularly for heart failure with preserved ejection fraction (HFpEF) — the most common form in older adults. By reversing pathological cardiac hypertrophy and stimulating autophagy, rapamycin directly addresses the stiffness and impaired relaxation that drive HFpEF. Preclinical models show meaningful functional improvement even when treatment begins after heart failure has developed.
FAQ
What is the recommended dose of rapamycin for heart longevity?
Research has shifted decisively toward once-weekly low-dose protocols — typically 3 to 10 mg per week — rather than the high daily doses used in transplant medicine. This approach appears to capture the geroprotective cardiovascular benefits while minimizing metabolic and immune-related side effects. Always consult a physician, as this remains experimental outside its approved transplant indication.
FAQ
Can rapamycin stabilise arterial plaques?
Yes. Research shows rapamycin enhances plaque stability by reducing necrotic cores and local inflammation. It inhibits foam cell formation — a primary driver of plaque growth — by reducing cholesterol uptake in macrophages while promoting its removal. Its anti-proliferative properties are already clinically applied in drug-eluting stents to prevent post-surgical artery re-narrowing.
FAQ
Is rapamycin safe for healthy people without existing heart disease?
Early human trials including the PEARL trial found low-dose intermittent rapamycin to be well-tolerated in healthy aging adults with no major adverse events reported. It remains an experimental use outside its approved transplant indication. Medical supervision is essential — a knowledgeable physician can monitor for any metabolic or immune effects and personalise the protocol appropriately.
Final Thoughts
Rapamycin cardiovascular health research represents one of the most exciting shifts in modern medicine — from treating disease after it develops to addressing the biological aging process that drives it. By targeting mTOR dysregulation and restoring autophagy, rapamycin offers a genuine path toward preventing arterial stiffness, reversing cardiac decline, and stabilising advanced disease. As ongoing human trials refine safe dosing protocols, rapamycin is on course to become a cornerstone of longevity-focused cardiovascular care.


















Sign in to leave a comment.